7T MRI Reveals New Insights into Some RRMS Features
Written by |
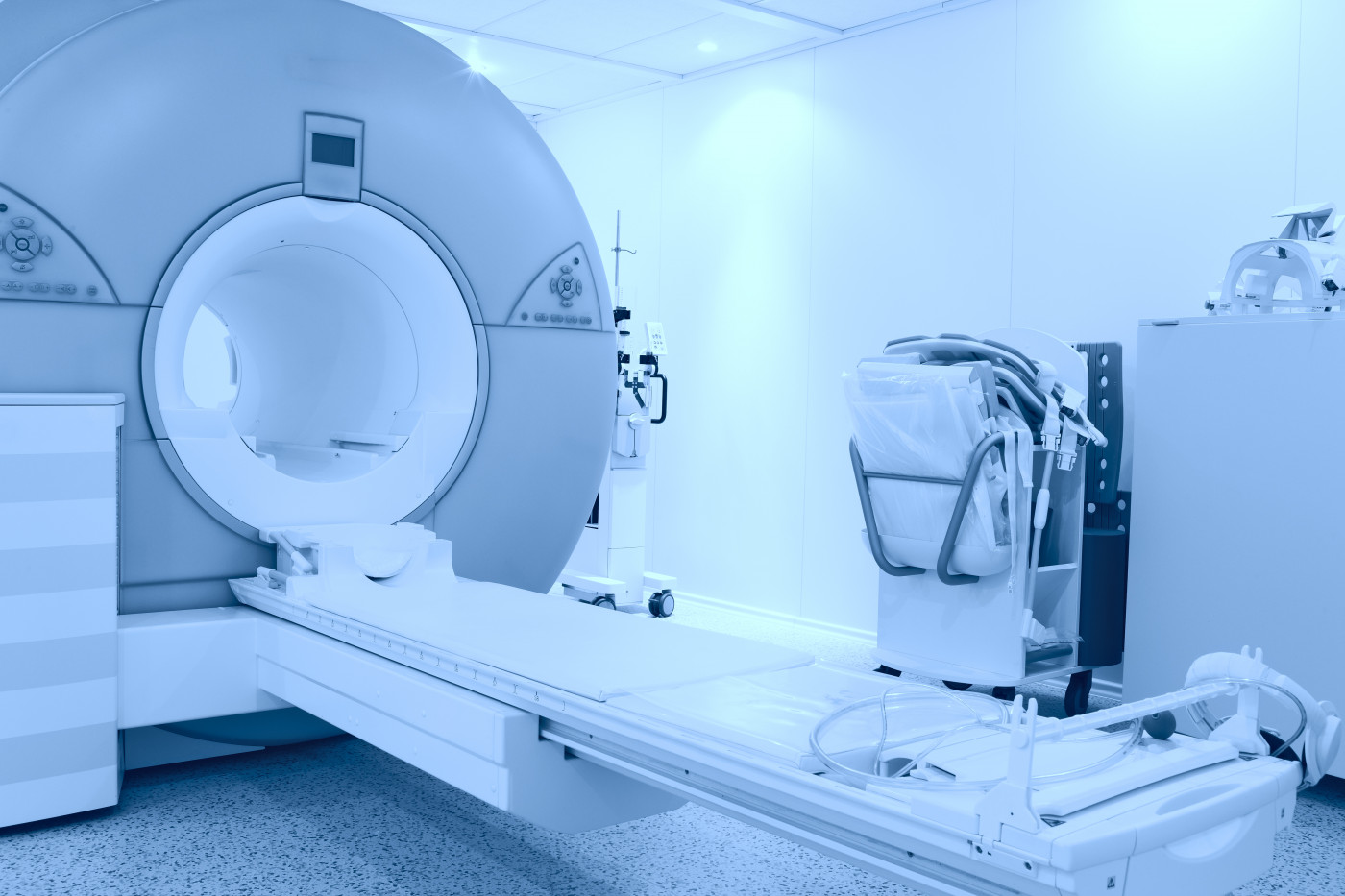
With the help of 7 Tesla magnetic resonance imaging (MRI), investigators discovered that leptomeningeal enhancement — a radiographic finding indicative of brain inflammation — is more common than previously thought in people with relapsing-remitting multiple sclerosis (RRMS), and is tied to lesions in specific regions of the brain.
The findings were reported in the study, “7T MRI cerebral leptomeningeal enhancement is common in relapsing-remitting multiple sclerosis and is associated with cortical and thalamic lesions,” published recently in the Multiple Sclerosis Journal.
MS is a neurodegenerative and autoimmune disease that affects the central nervous system (consisting of the brain and spinal cord). Some studies suggest that inflammation in the brain meninges — the thin layers of tissue that protect the brain and spinal cord — might contribute to the formation of gray matter lesions, and help explain how the disease progresses from RRMS to a secondary progressive form (SPMS) in some people. (Of note, ray matter are areas of the central nervous system made up of neuron cell bodies.)
Leptomeningeal enhancement (LME) is a radiographic finding in which the meninges surrounding the brain and spinal cord appear enhanced in MRI scans due to inflammation. LME may become apparent early on in the course of MS, and usually increases as the disease progresses. For that reason, some studies have proposed the use of LME as a marker of brain inflammation.
However, most MRI scanners used in clinical practice nowadays are based on 3 Tesla (3T) MRI technology, which offers only a limited view of LME in patients with MS.
In the study, researchers from Brigham and Women’s Hospital in Boston, Massachusetts, used 7 Tesla (7T) MRI, a more advanced form of MRI technology, to investigate if LME could be associated with the formation of gray matter lesions in people with RRMS.
The 7T MRI scanner at arrived at the hospital in 2017 and is only the second one in the country being used in clinical practice.
“The 7T MRI scanner affords us new ways of viewing areas of damage in neurologic diseases such as MS that were not well seen using 3T MRI; it’s capturing nuances that we would otherwise miss,” Jonathan Zurawski, MD, said in a press release. Zurawski is a neurologist at Brigham and Women’s Hospital and corresponding author of the study.
During the study, Zurawski and colleagues analyzed 7T MRI scans from 30 people with RRMS and 15 healthy subjects (controls) to look for signs of LME and gray matter lesions.
They found that 20 of the 30 RRMS patients enrolled showed signs of LME in MRI scans, whereas only one of the 15 healthy subjects did so. This meant that LME was 10 times more common in RRMS patients compared to controls.
In addition, researchers found that RRMS patients showing signs of LME had four to five times more lesions in the cortex and thalamus — two brain regions that control consciousness and alertness — compared to those who did not have signs of LME. These were telltale signs that LME was linked to a higher incidence of gray matter lesions, which was later confirmed by correlation analyses.
“Gray matter injury is an important part of MS, which may be a key factor leading to disease progression. Our hope is that by finding new markers of this progression, it opens up the opportunity for developing treatments that can prevent progression before lesions become widespread,” Zurawski said.
The team noted that some of their findings may be limited by the small number of patients participating in the study, and is now working on expanding the number of participants to be enrolled in future studies.
At this point researchers cannot draw any definite conclusions regarding the effect of LME on MS progression, or how these findings may also apply to people living with progressive MS. However, the team is planning to continue monitoring patients who participated in the study to examine how LME and their gray matter lesions evolve in the coming years.


Fitzs
This MRI could be used to detect nuero problems from many diseases, Lyme and other tbds too.