Multiple sclerosis symptoms
The symptoms of multiple sclerosis (MS), an autoimmune disease affecting the brain and spinal cord, can vary widely, although patients often experience movement problems, fatigue, pain, vision issues, bowel and bladder problems, and mood disturbances.
MS occurs when the immune system mistakenly attacks myelin, a fatty substance that surrounds and protects nerve cells, disrupting nerve signaling and causing nerve cell damage. The symptoms a person experiences depend on which parts of the brain and spinal cord are affected, the extent of inflammation and nerve damage, and individual factors such as age and sex, all of which can influence the pattern and severity of symptoms.
While MS symptoms can interfere with daily functioning and overall quality of life, a range of MS treatment options, including medications and complementary approaches, can help manage these issues.
What are the early signs of MS?
The initial symptoms of MS are variable, so there isn’t a single definitive list of early signs of MS. However, some symptoms that are commonly seen early on include:
- fatigue
- numbness, tingling, or other abnormal sensations
- difficulty walking or loss of balance
- vision problems
- pain
- muscle spasms and stiffness
- changes in bladder, bowel, or sexual function
- difficulty thinking
These symptoms are not exclusive to MS, and not everyone who experiences them will be diagnosed with the condition. Still, anyone who notices potential MS warning signs should consult a doctor.
Bringing a detailed record of specific symptoms, their severity, and duration can help healthcare professionals confirm or rule out an MS diagnosis. If MS is suspected, patients are usually referred to a neurologist or other specialist in nervous system disorders to confirm the diagnosis.
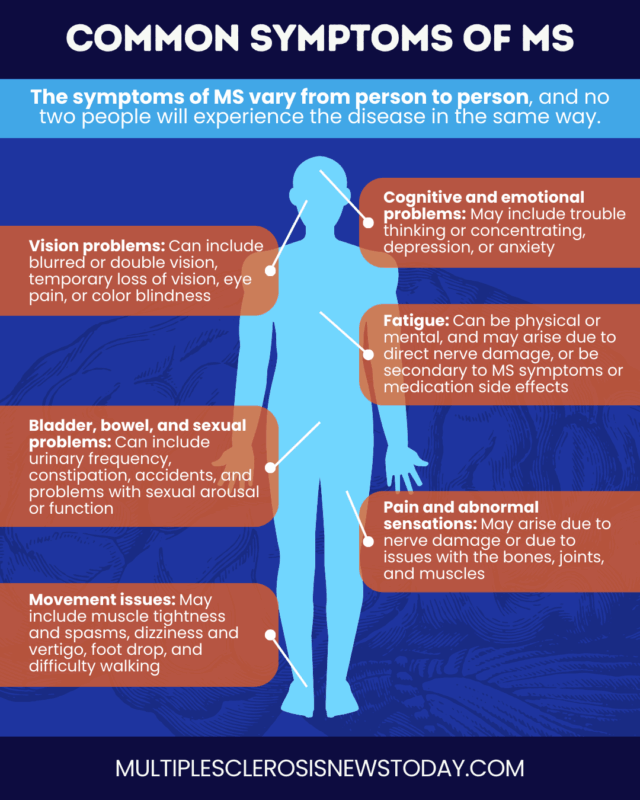
What are the common symptoms of MS?
Because the pattern and severity of MS symptoms vary widely from person to person, everyone with MS will have a different experience.
The most common symptoms of MS include:
- movement problems
- fatigue
- pain and other abnormal sensations
- bladder, bowel, and sexual problems
- cognitive problems
- depression and other emotional changes
- vision problems
Most patients will experience only a few of these symptoms, and the combination of symptoms varies significantly. No two people have exactly the same symptoms, and symptoms can also change or fluctuate over time.
| MS symptoms | Percentage of patients who experience the symptom |
|---|---|
| Movement problems | Up to 90% |
| Fatigue | About 80% |
| Chronic pain | About 50%-75% |
| Bladder and bowel issues | About 80% |
| Sexual problems | Up to 90% |
| Vision problems | About 70% |
| Cognitive changes | More than 50% |
| Mental health problems | About 50% |
Movement problems
One of the most common MS symptoms is spasticity, or abnormal muscle tightness and spasms, which is estimated to affect up to 90% of MS patients at some point.
Other movement-related issues in MS can include:
- dizziness and vertigo, due to damage to parts of the nervous system that regulate balance
- tremors, or uncontrolled shaking
- foot drop, in which the front of the foot is not adequately lifted during walking due to muscle weakness
- walking difficulties, which can arise from a combination of spasticity, weakness, balance problems, and fatigue
Fatigue
Fatigue, defined as mental or physical exhaustion that interferes with daily activities, affects about 80% of people with MS.
There are two main types of MS fatigue:
- Primary fatigue, or lassitude, is directly caused by nervous system damage. It is unique to MS and differs from other types of fatigue, as it occurs suddenly, is more severe, is exacerbated by heat or humidity, and does not improve with restful sleep.
- Secondary fatigue is caused indirectly by other MS symptoms, such as depression and stress, side effects from medications, and sleep problems.
Pain and abnormal sensations
Around 50% to 75% of people with MS experience chronic pain, which can generally be categorized as:
- Neuropathic pain: This refers to pain caused by nerve damage and is the most common type of pain associated with MS. It can be felt as a persistent and burning pain, although it may also manifest as abnormal sensations.
- Musculoskeletal pain refers to pain resulting from issues affecting muscles, joints, and bones. In MS, it occurs mainly as a result of spasticity, muscle weakness, and mobility issues.
Beyond pain, people with MS can also experience other abnormal sensations, such as numbness, tingling, burning, or itching, as a result of nerve damage. This is called dysesthesia, and it may take a number of different forms in MS, including:

Living with MS
Mental health and MS

Living with MS
Symptoms of MS vision problems

Living with MS
High-dose vitamin D delays MS progression
- the MS hug, characterized by a sensation of tightness or squeezing around the chest or abdomen
- trigeminal neuralgia, a sudden and severe electric shock-like MS pain that affects the face
- the Lhermitte’s sign, characterized by a sudden electric shock-like sensation running down the spine and into the limbs, often triggered by bending the head forward
Bladder, bowel, and sexual complaints
Inflammatory damage in MS can affect the nerves and muscles controlling bladder, bowel, and sexual function. Problems with these systems can affect up to 90% of MS patients.
- Signs of bladder problems in MS may include frequent urination, difficulty urinating, leaking urine, or having accidents
- Bowel problems could include constipation, stool leakage, or accidents
- Sexual problems can include altered genital sensations, low sexual desire, difficulty achieving orgasm, erectile dysfunction, and vaginal dryness
Emotional and cognitive problems
Mental health problems, such as anxiety, depression, and mood swings, are common symptoms in MS. They are estimated to affect about 50% of patients.
These emotional changes can be directly caused by nervous system damage or occur indirectly due to the emotional impact of living with a chronic disease or medication side effects.
Some people with MS may also experience pseudobulbar affect, a condition marked by sudden bursts of uncontrollable laughter or crying that do not match the person’s emotional state.
Damage to the nervous system can cause difficulties with thinking, reasoning, learning, problem-solving, and planning. More than half of MS patients will experience problems with cognition. These changes are usually mild, but more severe cognitive impairment can occur.
Vision problems
MS can cause damage to the optic nerves, which transmit information between the eyes and the brain. As a result, about 70% of patients will experience vision problems at some point in the course of their disease, which may include:
- blurred or double vision
- temporary loss of vision
- eye pain (especially when moving the eye)
- eye twitching
- color blindness
How does MS type affect symptoms?
MS is classified into four main types. While symptoms of MS can be experienced in all four types, their pattern and severity can differ.
- Clinically isolated syndrome (CIS) refers to a first episode of neurological symptoms that are suggestive of MS. People with CIS may never have another episode of symptoms, or they could progress to full MS.
- Relapsing-remitting multiple sclerosis (RRMS) is the most common type of MS. It is characterized by relapses, where symptoms worsen or new symptoms appear, followed by periods of remission where symptoms ease.
- Secondary progressive multiple sclerosis (SPMS) is a form of disease that follows RRMS and is marked by symptoms that steadily worsen, even in the absence of relapses. Relapses may still occur in SPMS, but they are usually less frequent, and symptoms do not completely disappear during remission periods.
- Primary progressive multiple sclerosis (PPMS) is a form of MS where symptoms steadily worsen from disease onset. Patients may occasionally experience relapses, but symptoms will continue to worsen.
How are MS symptoms different between men and women?
MS is up to three times more common in women than it is in men. Although most of the symptoms of MS in women are similar to those in men, there are some sex-specific differences.
| MS in men | MS in women |
|---|---|
| More likely to have PPMS than women | More likely to have RRMS than men |
| Often experience greater brain volume loss | Commonly experience better relapse recovery |
| Have more lesions with irreversible nerve cell damage | Have more lesions with active inflammation |
| More likely to have balance and walking issues | More likely to have vision problems |
Symptoms of MS in women
Some symptoms that are of particular relevance to women with MS include:
- menstrual and menopausal issues
- sexual problems
- pregnancy-related symptoms
Menstrual and menopausal issues
Some women with MS report that their symptoms are worse in the days leading up to and at the start of their period, although the reasons for this are not completely understood.
Some women also report that menopause symptoms, such as hot flashes, exacerbate their MS symptoms.
Additional research is necessary to understand the specific ways in which MS might affect women’s bodies.
Sexual problems
Women with MS may experience specific sexual issues, including reduced or painful sensations in the vaginal or clitoral area, vaginal dryness, and problems with orgasm.
Being able to discuss sex-related issues with healthcare providers and others is important for coming up with solutions that enable a healthy sex life.
Pregnancy-related symptoms
In general, MS does not affect a woman’s fertility, and there is no evidence that women with MS are at a higher risk of pregnancy complications than women without the disease.
While women tend to have fewer MS relapses during pregnancy, some report that certain MS symptoms feel worse during pregnancy, which may require adjusting treatment.
Symptoms of MS in men
While men are less likely to develop MS, they often experience a more aggressive disease course than women. For example:
- Men are more commonly diagnosed with PPMS than women, so their symptoms are more likely to take on a progressive course from disease onset
- Men recover more poorly from relapses, show faster disability progression, and reach certain disability milestones earlier than women
- Men have faster brain volume loss and more lesions with irreversible nerve damage
- Men more commonly experience poor balance and walking problems, and have more severe cognitive issues
Sexual problems for men with MS may include erectile dysfunction, reduced sexual desire, decreased genital sensation, and difficulty reaching orgasm. As with women, open communication with healthcare providers and partners can play an important role in addressing these issues and supporting a healthier sexual life.
Multiple Sclerosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
 Fact-checked by
Fact-checked by