#MSParis2017 – Siponimod Leads to Dramatic Drop in MS Lesions, Phase 3 Trial Shows
Written by |
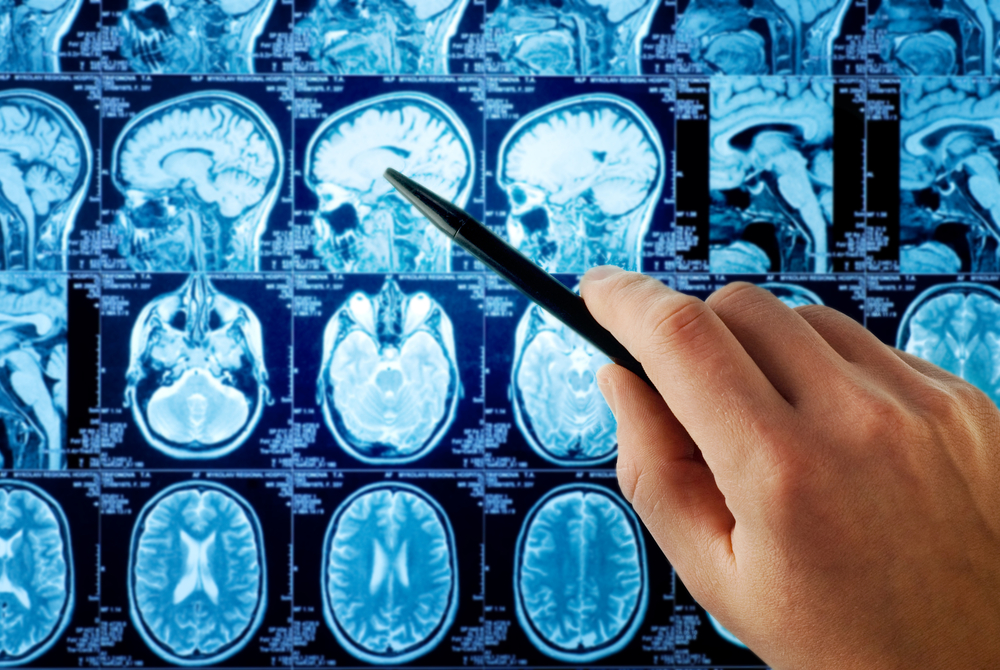
Novartis’ Siponimod led to a dramatic drop in the number of inflammation patches in the brains and spinal cords of secondary progressive multiple sclerosis patients, according to a Phase 3 clinical trial.
Robert Fox of the Cleveland Clinic’s Mellen Center for Treatment and Research in Multiple Sclerosis presented the findings on what scientists call MS lesions at the 7th Joint ECTRIMS-ACTRIMS Meeting in Paris. One of the largest congregations of multiple sclerosis scientists worldwide, the conference started Oct. 25 and runs to Oct. 28.
The results that Fox presented strengthened earlier findings demonstrating that siponimod slowed the progression of SPMS.
His presentation focused on magnetic resonance imaging measurements of lesions during the Phase 3 EXPAND trial (NCT01665144). It was titled “Effects of siponimod on MRI outcomes in patients with secondary progressive multiple sclerosis: results of the phase 3 EXPAND study.”
The trial covered 1,645 patients randomly assigned to treatment with either siponimod or a placebo. For every patient receiving a placebo, two received siponimod, for a total of 1,099 siponimod-treated patients.
Participants had MRI scans at the beginning of the study and every 12 months afterward.
Researchers recorded both the number of new lesions and the number of existing ones that were growing. They also recorded the number of lesions with active inflammation, and patients’ brain volume loss.
A key finding was that siponimod reduced the number of patients’ gadolinium-enhancing inflammatory lesions by 86.6 percent after a year. After two years, the average reduction was even better — 91.1 percent. Gadolinium-enhancing lesions indicate that inflammation is ongoing.
Another important finding was that siponimod-treated patients had experienced 39 percent less brain volume loss than placebo-treated patients after a year.
“Siponimod significantly reduced MRI lesion activity and slowed brain volume loss in patients with SPMS as early as month 12, with effects sustained to month 24,” Fox said.
These results, together with a reduction in patients’ disability that previous trials had demonstrated, “support the overall beneficial effect of siponimod in patients with SPMS,” Fox said.
MS is an autoimmune disease, or one in which the immune system attacks healthy cells rather than invaders.
Siponimod binds to two sphingosine-1-phosphate receptors found on immune cells known as lymphocytes. The binding keeps lymphocytes in lymph tissue rather than entering the brain and spinal cord, reducing inflammation.
Preclinical-trial studies have suggested that siponimod can help repair damaged myelin, or the protective coating around nerve cells, and the nerve cells themselves. Myelin and nerve cell damage are hallmarks of MS.


Leave a comment
Fill in the required fields to post. Your email address will not be published.