Know which questions to ask your neurologist about MRIs
Written by |
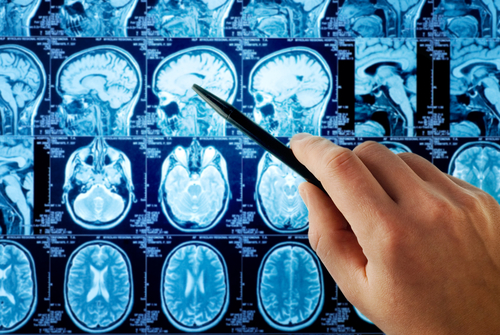
 I’m sure all of us with multiple sclerosis have had at least one magnetic resonance imaging (MRI) scan. Most likely, more than one.
I’m sure all of us with multiple sclerosis have had at least one magnetic resonance imaging (MRI) scan. Most likely, more than one.
MRIs are designed to scan and provide detailed pictures of the body, the brain included.
The test can reveal scars (plaque lesions) on the brain and the spinal cord. Even though there are no definitive tests for MS, the plaque lesions that appear on MRI photos can be a good indication that MS is the culprit.
In my experiences in dealing with MRI reports I have been left feeling I wasn’t given the whole story. Maybe I didn’t ask the correct questions, but my doctor didn’t offer any pertinent information, either.
The 2016 summer issue of Momentum Magazine, published by the national MS Society, has a very good article by Susan Worley titled Demystifying MRIs. It discusses that MRIs offer useful information. But it also shines light on the fact they are limited in what they can report.
The main information in the article comes from Daniel Reich, MD, PhD, of the National Institutes of Health.
He states that the majority of lesions that show up on MRIs do not have symptoms or relapses associated with them. So, it can be very difficult for experts to predict what path new lesions will take.
It is unknown if the lesions will produce symptoms or if they will repair themselves. He says lesion repair is part of the reason people recover from relapses.
Reich adds that another difficulty of reading MRIs is “whenever there is new inflammation in the body there tends to be a lot of swelling, which causes more water than usual between the cells of the brain.” He adds that the water makes it difficult to see “how much of the myelin and how many of the nerve cells have been damaged.”
Knowing the correct questions to ask may help decipher some of the unknowns of MS.
Another doctor mentioned in the article is Lily Henson, MD, of Piedmont Healthcare in Atlanta. She offers some questions that you can ask your neurologist when going over your MRI report, and suggests letting your doctor know if there is something you don’t understand.
Ask questions such as: “Do you see any new scars or any evidence of permanent nerve cell loss?” Ask if there were any changes on the MRI because those changes can lead to disability.
Hansen said “Even when no new scarring is apparent, the scars that have occurred in the past are still there, and there could be activity occurring underneath the surface.”
She ends with “perhaps most importantly the absence of new lesions doesn’t mean that a patient can start thinking about discontinuing his or her medications. Previous activity may be under control because of the disease-modifying agent a patient is taking.”
The article helped me realize that an MRI is not the see-all I thought it was, and that by asking my neurologist direct questions and tracking my symptoms, I will have a better picture of this disease.


Maytha Frankford
Thanks for this information! It will be helpful for me in communicating with my Dr.
Debi
You're welcome Maytha!:)
Michelle Burnett
Thanks so much! I was so confused when I had my MRI. They said my Brain scan was stable but didn't add much but they were happy with results and to keep taking Copaxone.
Thank you
Michelle
Debi
You're welcome Michelle!:)
Chris Arnold
My new neurologist wants a new MRI (it’s been 10 years). What new information can be learned that will be useful? MRI’s are not cheap. I have made great progress on my own via diet and exercise (no meds). If the MRI shows progression, I really don’t care to hear about it (or pay for it) just to satisfy my neurologist’s curiosity!
Taylor Hansen
It's good to know that you should ask about any permanent nerve cell loss after an MRI. My uncle is scheduled to meet with a neurosurgeon next week and he is worried about what they will find in the MRI and if it's cancer on his brain or not. I'll be sure to send him this so he knows what to ask the doctor when the time comes.