Multiple Sclerosis Drug Gilenya May Also Stop Chemotherapy Pain, According To Research
Written by |
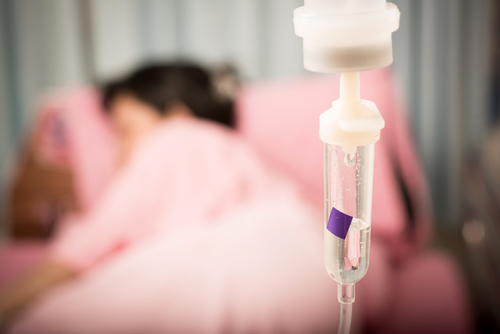
 A team of researchers from the University of Saint Louis has found a molecular pathway involved in a painful chemotherapy side effects, and a drug that might be able to stop it. Paclitaxel (also known as Taxol) is a chemotherapy drug commonly used to treat different forms of cancer such as ovarian, breast and lung. However, in 30 to 90% of patients treated it results in a devastating side effect called chemotherapy induced peripheral neuropathy (CIPN), a condition characterized by tingling or numbness in the hands and feet, burning pain in the limbs and hot/cold temperature extremes.
A team of researchers from the University of Saint Louis has found a molecular pathway involved in a painful chemotherapy side effects, and a drug that might be able to stop it. Paclitaxel (also known as Taxol) is a chemotherapy drug commonly used to treat different forms of cancer such as ovarian, breast and lung. However, in 30 to 90% of patients treated it results in a devastating side effect called chemotherapy induced peripheral neuropathy (CIPN), a condition characterized by tingling or numbness in the hands and feet, burning pain in the limbs and hot/cold temperature extremes.
The team studied paclitaxel and discovered that the pain pathway is dependent on the activation of sphingosine1-phosphate receptor subtype 1 (S1PR1), a type of G protein-coupled receptor involved in many biological processes such as cell proliferation, angiogenesis, migration and immune cell trafficking. When S1PR1 is activated in the central nervous system, a series of damaging neuro-inflammatory processes are initiated, ultimately leading to pain.
A Novartis drug that modulates S1PR1, called FTY720 (Gilenya), is already being commercialized as an FDA approved therapy for multiple sclerosis and when the researchers tested this drug in the lab, they found that by blocking S1PR1, the CIPN effect caused by paclitaxel was blocked and reversed without affecting its anticancer effects. Additionally, it seems that the beneficial effects of FTY720 were extended to oxaliplatin, another chemotherapeutic agent commonly used in colon and other gastrointestinal cancers.
Although clinical trials will be necessary to understand the safety and efficacy of using FTY720 to treat CIPN, this approach seems promising not only to relieve cancer patients of debilitating pain improving their quality of life, but also to allow the administration of larger and more effective doses of chemotherapy drugs.
[adrotate group=”4″]
This study, led by Dr. Daniela Salvemini, professor of pharmacological and physiological sciences at the University of Saint Louis, was funded by the Leukemia and Lymphoma Society Translational Research Program and the Mayday Fund, and was recently published in the Journal of Biological Chemistry.


Leave a comment
Fill in the required fields to post. Your email address will not be published.