MRI Scans Could Identify Children at High Risk for MS, Yale Study Finds
Written by |
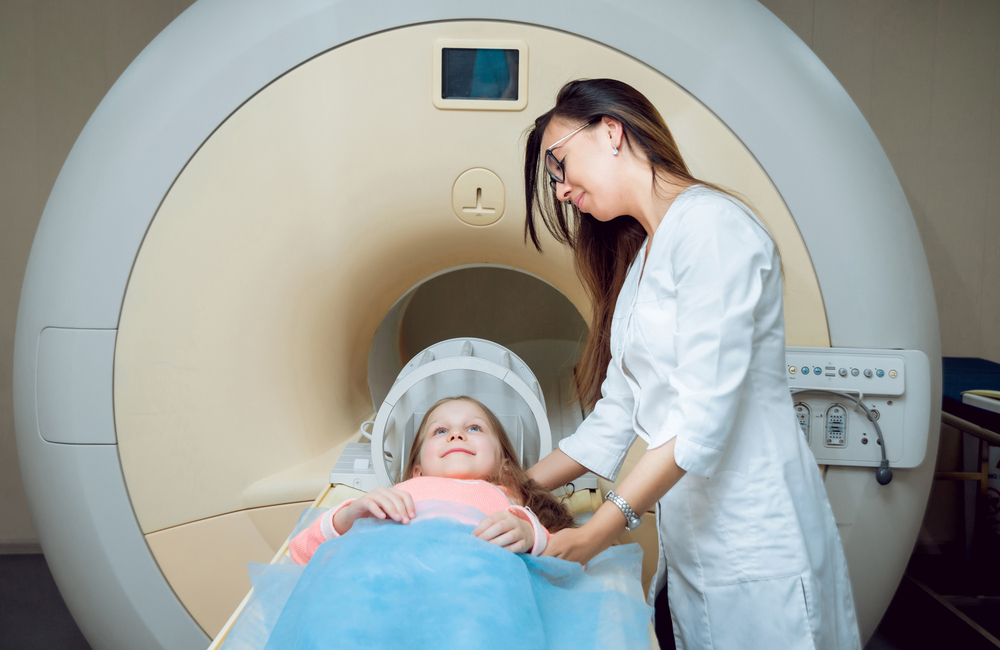
Magnetic resonance imaging (MRI) brain scans of children could reveal changes associated with multiple sclerosis (MS) before any symptoms are developed, according to a study by scientists at Yale University School of Medicine. The findings suggest that brain and spinal cord scans can identify children at high risk for developing MS.
Children who had signs of antibodies in their spinal fluid or lesions in the spinal cord were more likely to develop MS symptoms, researchers found.
The study participants had what researchers call radiologically isolated syndrome (RIS), which are MRI lesions that indicate a loss of myelin. RIS has been studied in adults, and researchers know that about one-third of adults with these lesions eventually develop MS symptoms. But until now, no one had studied RIS in children.
“For the first time we have proposed a definition of RIS in children,” Naila Makhani, MD, assistant professor of pediatrics and neurology at Yale and lead author of the study, said in a press release.
Published in the journal Neurology: Neuroimmunology & Neuroinflammation, the study followed 38 children who had an MRI scan in which researchers found demyelinating lesions. The children underwent the scan for other reasons, including headaches, depression, seizures, and concussions. Headaches were the cause of the scans in more than half of the cases.
According to the report, “Radiologically isolated syndrome in children — Clinical and radiologic outcomes,” more than two-thirds of the children were girls. Participants were followed for an average of 4.8 years. Among them, 29 had spinal cord MRI scans and 23 also had a spinal tap done to test the spinal fluid.
Fifty-seven percent had signs of antibodies — so-called oligoclonal bands — and 17 percent had spinal cord lesions.
In the entire group, 42 percent developed MS symptoms within a median time of two years. While the group was small, the data indicate that children with RIS develop MS symptoms sooner than adults, who typically have a five-year delay between MRI lesions and first symptoms.
A large percentage of the children — 61 percent — also had new lesions that were detected during follow-up scans.
“Children with RIS may represent a high-risk group of children that need to be followed more closely for the later development of clinical multiple sclerosis,” Makhani said.
In an attempt to look for factors that made it more likely to predict who would go on to develop symptoms, researchers analyzed a range of parameters. After taking age and sex into account, they found that children who had signs of antibodies in their spinal fluid were up to 11 times more likely to develop symptoms compared with those who did not have them. Children with spinal cord lesions were about 8 times more likely.
Five of the children with RIS received Interferon beta 1a before they developed symptoms, and three did not show disease signs after a follow-up of 1.7–15.3 years.
The study demonstrated that children with RIS share many of the same characteristics as adults with the syndrome. Because spinal cord lesions were linked to symptom development, the team argued that all children with RIS should have spinal cord MRI scans to identify those in need of closer follow-up.
It is also crucial, they said, to develop guidelines for treatment of children with RIS.
“We hope that our work will help inform expert guidelines for how to follow up children with RIS and help us accurately inform families of the risk of later developing multiple sclerosis, something we were previously unable to do,” Makhani said.

Leave a comment
Fill in the required fields to post. Your email address will not be published.