Brace Yourself: My Ups and Downs with AFOs
Written by |

It was late May 2014, and my wife and I were on our first trip to the Cleveland Clinic. We’d been to Cleveland for a wedding a few years earlier but had been too busy to explore. We booked a room at the Tudor Arms, a cool, old hotel near the clinic’s Mellen Center for Multiple Sclerosis, hoping for a chance to look around.
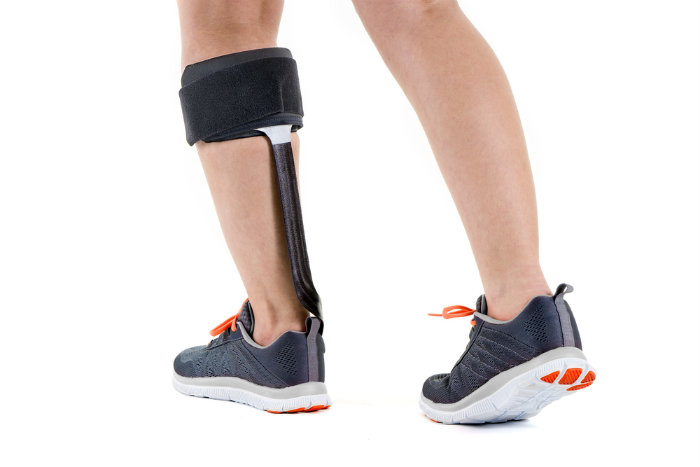
I had only recently received my ankle-foot orthosis (AFO) to compensate for my ever-worsening foot drop. Appropriately named “the BlueRocker,” the carbon composite AFO that was Velcro-strapped around my right calf had a support “rod” curling around my leg and a “springboard” fitting in below my right foot, under the sole insert in my shoe. The demo unit I tried was pretty remarkable. Very light, and at the time, very effective at reciprocating the energy I was expending with each step. It reliably “rocked” my body weight through my stride, pushing my toes and foot upward into the correct position as I walked.
But I had barely used the AFO before our trip, for a few reasons. First, I hadn’t thought through how the brace might actually integrate into my life — how and when to use it. Devil, say hello to details. Over time, I learned that it worked well for me when I had straight, flat terrain. Steps, bumps, any sort of nuance or flexibility, not so much.
(AFO Pro Tip #1: Don’t try and drive a car with a fixed-position AFO. Unless you want to accelerate very quickly and then brake in the same manner. I also found it challenging on stairs.)
Second, I struggled to find shoes that comfortably accommodated the stiff, intrusive device. I asked the orthotist who fitted me for a suggestion and she said to try larger shoes. Which I did. But the added weight and length made it harder to lift my foot, and I cheated by “swinging” my leg through as a result.
(AFO Pro Tip #2: Running shoe companies often sell models designed to accommodate clunky, thick inserts that are similarly intrusive. Though sometimes expensive at $100 or more, they are light, durable, and occasionally cool looking.)
By the time we got to Cleveland, we’d worked our way through those wrinkles. We spent the morning at the clinic and, with extra time on our hands and sunny, late spring weather, we decided to go for a walk.
Like a dog unleashed, I wanted to walk everywhere. We walked downtown and took in its architecture. We walked by the lake and by the Rock & Roll Hall of Fame. My guess is that we maybe walked 2 or 3 miles before my right leg simply wouldn’t lift any longer.
Four years later, I can no longer lift my foot high enough while wearing the AFO for it to clear the ground properly, increasing the likelihood of me catching the front of my foot and then toppling forward. So, I don’t use it anymore. I can still walk a short distance (maybe a few hundred feet) with little assistance, and then my right leg gets tired and my knee wants to snap and lock out backward — a freaky and untenable stride. I can still make a few trips up and down the stairs, but I can now barely — barely — walk around the block, even with my rollator walker.
Some of that is likely due to MS. Some of it is the dearth of walking I’ve done as it has become harder. Use it or lose it, right?
(AFO Pro Tip #3: Like everything else with MS, I understand I have to push through and do things I don’t like doing to achieve a greater good. I’ll quickly admit that this may be my least favorite — and least followed — AFO Pro Tip.)
Not long ago, I met with my physical therapist to talk about what I can do to keep walking. She asked me to bring my AFO to my next appointment. “I can see why this isn’t working for you,” she said, pointing out that the brace’s design wasn’t doing me any favors when I presented it to her. I told her that the brace was the one that had been prescribed for me, presumably because somewhere along the line, someone thought it was the best solution for me.
Which leads me to:
(AFO Pro Tip #4: There are a lot of AFOs out there, each providing varying levels of assistance.)
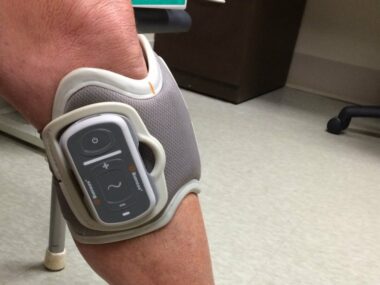
The trick, for me at least, has been finding the right person to recommend the right one, as my needs changed. Now my physical therapist and I are looking at alternatives. And as I write this, I am wearing an in-home trial unit of a functional electronic stimulation (FES) device. I have it for two weeks. More — lots more — about it, soon.
***
Note: Multiple Sclerosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Multiple Sclerosis News Today or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to multiple sclerosis.


Lisa
I used an FES, as a trial one summer. Loved the positive results...then my insurance company would not cover cost for me to take one home. :(
I believe they might cover costs now, but honestly, I did not know how the system would work under long, thick, winter pants...so I've been postponing retrying. I'm still debating the FES and a new wardrobe of pants.
Thanks for the story of your triumphs and mishaps. We all get excited by any positive change and tend to overdo it. I hope the system works wonders for you.
Mike Knight
Thank you, Lisa, I appreciate you reading my column and letting me share my experiences. My hope is that something I write will somehow be helpful to someone else as she or he navigates this extraordinarily complex disease and the myriad issues it creates. Our insurance also does not cover the device and it would be an extraordinarily expensive investment should we choose to make it (for a lot of different reasons). More soon, and thanks again!
Renee Sistrunk
I started my first ocrevus infusion today. I feel good right now.
Sue
I have the Turbomed AFO, I live in the UK. It’s a Canadian AFO. It works on the pricipal of pulling your foot up so that you don’t trip. I find it so much more reliable than the nhs plastic one. This one I can wear with a selection of shoes, easily fitted. So far I am pleased with it.
Mike Knight
Thanks so much!
Caroline
Hi Sue
Can you send a picture of the Afo you have. Thanks
Mike Knight
It's on its way, Thanks!
Carmela
Thanks for sharing about Turbomed. I was wondering how well this works.
Cheryl McGovern
Are you still using Turbo Med?
Teresa Barr
Mike- also look into exercise for foot drop. The MS gym- Trevor Wicken.
Remarkable!
Mike Knight
Thank you, Teresa, I will!
Tana
The MS Gym is helping me. I have the AFO that is pictured in this article but I only wear it for long walking times, this helps keep my muscles from getting used to it. Mine is the left leg so I can still drive when wearing it. Lol.
Frances Worness
I am having my first full dose next Tuesday. Having completed the first two half doses last October, I remember having more energy and ability to move around one to one and one-half months after the initial split infusion. Right now,less than one week from having the fist full infusion (second treatment), I am wondering if I should have just stayed on Aubagio. My body has NO energy. I feel like I have been hit by a Mack truck. The complete lack of energy and will to even move is something I have not dealt with before to this degree and I am going to be using my emergency wheelchair to get to the infusion center. I am hoping that, like some of the other MS drugs (especially Tysabri), my body just needs it's refill. I am wondering if anyone else newly on Ocrevus is experiencing similar symptoms?
Mandy Hagler
I hear ya! I feel like I've been hit by a Mac truck and then some. I have to get a BAG of Solu-Medrol before my Ocrevus. Then, I have to remember that I am NOT Wonder Woman the next couple of days and then I am back to feeling like I've been ran over by several semi-trucks. I hate feeling like this, and NOW, I have to be fitted for an AFO for my left leg/foot. All while trying to compensate for my right hip, which has to be replaced, completely. I am only 39! Does anyone else ever feel like you're a "walking" medical disaster, or is it just me?
Sorry for the rant. Just very aggravated and no one here understands.
Susan
I started with an AFO and quickly switched to an FES, even though insurance did not cover it. It’s been extraordinarily helpful and I believe I’m still walking because of it.
It works fine under all sorts of clothes, except skinny-leg pants, even under long underwear.
I don’t wear it all the time, just when I’m out of the house.
Mike Knight
Thank you Susan!
Dennis
I have a stimulator called a walkaide, it is about a 4 inch wide cloth cuff with 2 electrodes in it. I wear this just below my knee on my affected leg and every time I take a step it applies a small shock to my foot and lifts it up. The cuff has a small electronic module about the size of a small deck of cards held to the cuff with Velcro that provides the signal to give you the shock when you bend your leg to take a step and is adjustable for the amount of power you need. I have wore this device for about 4 years now with much success, however when I have this on my leg it does prevent getting down on your knee without getting it out of the way if you fall and need to get back up.
Dennis
Mike Knight
Thank you, Dennis, I appreciate it!
Michael McDonald
I also used them, but Don’t drive ever with any of them!!
I believe that the nerves damage Must be rebuilt. I look at it as an electrical Short. The coating of baby’s nerves are developed in their first two years, researching that process, how can we stimulate it to rebuild our nerves? Baby food? Mothers breast milk?
Natural methods such as pine bark, help to stop the immune systems destroying the sheath.
Any questions?
Lindsey
where did you get this product from?
Phil Longford
The FES takes a while to set up. Newer pads, in good condition, make a big difference. Very easy, even for the experts, to put the pads in the wrong place. A few centimetres out, and foot does all kinds of strange movements. Allow a few minutes, to get wired up.
Mike Knight
Thanks, will do!
Joe
I have tried 3 different AFO's and the best one for me was a plastic one where they molded plaster around half my foot, ankle and up to my calf. After it was made they put a valcro strap that looped around the front of the ankle and another around the top of my calf. They put the bottom under the cushion of my shoe. The mold was very uncomfortable so I put the brace on top of the cushion and it was much better. Next I had to get rid of the upper strap because when I would lose my balance, I would hyperextend my knee trying to regain my balance. After all that, it has been very good to me. I have used it for 12 years now. I have SPMS and now I mostly use a roller walker and sometimes two canes for balance, but I wouldn't be able walk with out it. It does get uncomfortable when using it all day. The fiber one that was more flexible only lasted a year because it splintered. A person that makes artificial limbs made this for me and my insurance paid for this. I only use my wheel chair for long day activities.
Mike Knight
Thank you, Joe, for reading the article and also for the great information you're sharing here. As you are pointing out, there is a certain amount of trial and error with these things, and it isn't always immediately apparent that there are some fairly fine nuances that can make a big difference. I really appreciate it
GARY SHAMBLEN
For me the Bioness L200 became my choice over the AFO for 5 yrs or the Walkaide trial. After 3 yrs. much nerve/muscle function was reestablished. Battle your insurance Co. if they refuse to pay. Start with a letter of medical necessity from your Neuro. and don't back off.
Gary Shamblen
[email protected]
Mike Knight
Thank you, I really appreciate you reading the column and also the feedback and recommendations!
Marcia Gartland
My insurance won’t pay for it & $6000 is a lot to pay out. Plus they wanted a few hundred dollars for a trial period. I wear a Soft AFO. You can buy them on Amazon. It has helped so far. There are a couple different kinds. One will allow use with sandals. The other with tie shoes. Not expensive either. I selected mine from Ossur
Suze H
I am so annoyed over the AFO. I am on my 3rd. I wanted something that I could wear with skirts and dresses. I was given one that went the whole length of my foot. Firstly, my foot burned. I was told it was either in my mind or neuro pain.NOT! Had to take pictures of what eventually became huge blood blisters. Then I found out from new physical therapy doctor that it had caused me to hyperextend my right. Also, I was told my shoes were too small. So, I have a new one that I call Frankie as in Frankestein - big bolts on ankle. Bought larger wide ugly shoes. Guess what? Same burning and worse had it on today for 8 hours and can barely walk, excruciating pain.
Early on with Frankie, decided I am going to figure out how to 3D print my own
Mike Knight
Thanks, Suze, I hate that you're having the problem but your comment made me smile because it seems like you're taking all of this in stride (sorry not sorry for the pun). All kidding aside, I read not too long ago about how important it is for AFO users that the device takes fashion and appearance into account as that plays a large role in how often the devices used, etc. It's here if you wish to read it: http://lermagazine.com/article/finding-fashion-options-that-accommodate-afos. Thanks for reading the column and good luck!
Elizabeth Henehan
I have used a Walkaide for at least 5 years. It is less expensive than the Bioness. I use it whenever I go out and sometimes in the house. You can put it in exercise mode and it lifts your toes while you're sitting. Insurance wouldn't cover it but I'm glad I purchased it. It's supposed to have a residual effect.
Andrew Braunstein
My most comfortable AFO is a pair of lightweight work boots from a discount shoe store. Driving is easier and I simply tie the laces tighter for more foot drop support.
I am planning to get some lightweight mid height hiking boots next for the summertime.
Allan Miller
I have mild foot drop and I use a NaviGait brace that fits around my calf. It has a band in front that attaches with a hook to the shoelace or Velcro strap at the bottom of my instep. Nothing in the shoe and it’s very comfortable and effective.
CHRISTINE DePALMA-CUNNINGHAM
I went through 4 different hideous MAFOs for foot drop on my right side due to MS. I Finally found the FES WalkAide. I’ve been a loyal WalkAide user for about 4 years now. My insurance also denied the device however, I wouldn’t accept that as an answer. I was fortunate that I could find the $4k cost and then began a concerted effort to get them to cover it. I went to multiple physical therapists and asked them to evaluate my walking using the EDSS timed walking with nothing, my WalkAide, and then with the MAFO of the moment. Three different therapists all separately all came to same conclusion. The WalkAide was clearly what was helping...to be honest I was better with nothing rather than the MAFO with ridiculous huge clown shoes needed to fit the uncomfortable MAFO ! Added to those documents, I had my physiatrist write a few letters. It seemed they would’ve paid for The WalkAide if the foot drop was caused by a spinal column injury ....and that the use of a WalkAide for MS is experimental and they don’t pay for experimental equipment..... my doctors letters focused on the fact that MS is a spinal column injury caused by my own body! Seems after the third rejection the insurance company’s policy was to then to have it reviewed by a specialist in field rather then a claims adjuster ....and I was finally reimbursed what I’d spent. The moral of my tale....don’t stop trying until you know you can’t go any further...it just might work. Good Luck
Mike Knight
Thank you for sharing this, Christine, this is such great information to have and I really appreciate it. Our insurance is taking a similar position (i.e., they don't want to pay for it, as is unfortunately common, at least in the U.S.). In a bigger way, though, my hope in writing about all of this is that it might help arm others as they fight the same battles, not only to try and walk better, but to get their insurance companies to help with what is obviously a game changer for so many people with MS. It's pretty easy to develop an ROI calculation that demonstrates why it's actually smarter investment for the insurance companies to cover the costs of these devices due to fewer PT visits and fewer injuries/claims from falling, etc. Again, thanks for reading the column and thanks so much for the valuable insight!
Cheryl
I have been wearing a carbon-fiber AFO since 2008. I was a runner before I was diagnosed with MS in 2006. Drop foot was one of my first symptoms, but I did not want to give up running. My orthotist from Hanger Clinic outfitted me with a Noodle AFO. I have completed 44 marathons with the Noodle. I tried Bioness and Walk-Aide, but had trouble with them staying on my leg while running. The TurboMed founder sent me samples of his AFO and I like how it does not insert into my shoe and that my calf can activate (I have atrophy from all the years in an AFO). I still have to "learn" how to run with it. I am also working with the makers of the SpryStep AFO on a sleeker and lighter device to help with my running. There are so many products and ideas out there. You have to be your own advocate and find them. Hooray for google! Cheers and thank you for writing this article!
Mike Knight
Thank you Cheryl, this is such great information (and I am totally in awe of the 44 marathons). Thanks so much for sharing, I’ll look into the Noodle!
CHRISTINE DePALMA-CUNNINGHAM
Thanks Cheryl....I’m going to check with my orthodist at Hanger about this type of device...it seems I might be too compliant with wearing my WalkAide and sometimes I need to take a break from it cause I get a rash under the electrodes .....BTW the WalkAide is actually made and maintained by Hanger
Pate Kelleher
I use a ago device that actually works pretty good. It’s plastics and my foot sits in it and goes up the back of my calf are almost to the knee. It was molded for me specifically. I need to go up a size in shoe in order for it to fit; sketchers/crocs work vest for me easy to get on.
Joni
I have been using a carbon fiber afo for the last six years. It works so well for me that I forget how much I depend on it until I take it off. I wear custom orthotics over the top of it that make it very comfortable. My only gripe is that I only have two pairs of shoes that I can wear. It’s a bummer that I can’t wear dresses because of the look but I’m so grateful that I found something comfortable that helps me walk.
Carol
I too have had problems from my afo, while it stops the foot drop it has caused me to have hip and low back pain due to my arthritis in my hips and herniated disc. I imagine that if you're only dealing with me it's a viable alternative. I now don't use it, I just use more caution while walking! Walker with seat for testing helps alot!
Tracy
I started out with an AFO and my physical th erspist recommended bioness. It changed my life. It was for my right leg and totally fixed my foot drop. At the time insurance paid in full. Fast forward 6 years I now need one for left leg and current insurance will not pay for it. They feel fes is experimental. Unfortunately i am not in position to pay for one. If you can I highly recommend getting one. It is amazing!
Ursula Tracy
I recently obtained the Bioness system. What I thought was going to be the answer for my drop foot, has just left me looking for different options. My right foot does not clear the floor unless I vault my leg not bending my knee. I hate having this ‘monster walk’. I’m going to Vegas in over a month and my gf said I should get a wheelchair. I never thought I would be debating this. Thank You all for your comments and shares.
Mike Knight
Thanks so much for reading the column and for your input and experience on this. But ugh. I totally get where you're at on all of this and it sounds as if we're at roughly the same place in progression. Does your Bioness include the hip "unit" as well? For some reason I thought that was part of their approach to "hoisting" your leg and foot more. Maybe not. I'm working my way through trials of both WalkAide and Bioness and may likely also try additional focused PT/strengthening just to be thorough before integrating a chair of some nature (transport, self-propelled, etc.). Good luck...and have fun in Vegas!
dee middleton
Thanks, very interesting I can relate to so much of it. I am in an AFO and would like to try the Walk Aide but I keep falling and breaking things, (ankle, hip, femur) so once I get all of the medical bills caught up, I will give it a try. I appreciate the information.
Gillian
Hi - I have MS and I was sold an AFO by hanger which I don't think was the right decision for me. I also tried the Bioness and the Walkaide but in both cases they could not get a good "connection". Thanks to your article I am now looking into the turbomed product. I like the fact that it is an external AFO - I won't have to throw out all my shoes and even better buy bigger sizes. Oh the joys of the MS roundabout. Thanks for the article.
Mike Knight
You are sure welcome, Gillian. I am actually "test walking" this product. I've had it for about a week and so far it's been helpful though I did trip and fall while wearing it, though that was really my fault for overdoing it. Yes, the joys…
Lisa Trimarchi
Thanks so much for sharing your story, Mike. I’ve been debating getting an AFO for 6 months. I’m turned off by the limited selection of fashionable shows and also the Velcro (I don’t want it to snag my dresses.)
I’m considering trying a different orthotist. What do you think about that?
Mike Knight
Hi Lisa! I no longer use an AFO (no longer effective) but I had similar issues and concerns re: footwear, not so much for snagging my dresses though;-). I totally get wanting to maintain a sense of style though (it's part of a sense of self to me and to so many with disabilities...https://www.washingtonpost.com/health/for-people-with-disabilities-finding-clothing-that-is-stylish-and-meets-their-needs-is-getting-easier/2019/08/02/1889990a-87cf-11e9-98c1-e945ae5db8fb_story.html).
If you haven't shared that perspective with your present orthotist, you might.
I can't give you medical advice, but I keep getting the chance to learn that is ALWAYS later than I think with my particular brand of MS and that I've got to run the show. I can't get panicky, but I gotta keep moving. The AFO really made a big difference to me for 12-18 months and then it didn't. I tried one of these (https://www.saebo.com/shop/saebostep/) and kinda liked it (but it was too late for it to be helpful to me). I sure hope that's somehow helpful. Thanks for the note and the very best to you!
Marcia
Looking for tall winter boots to accommodate a third grade boy with AFOs.
Sofia lim
Reading about your experience with the ankle foot orthosis (AFO) is incredibly uplifting! Thank you for sharing your story and reminding us all of the power of perseverance. Keep shining bright!