Rosacea Appears to Be Linked to Multiple Sclerosis in Women, Study Reports
Written by |
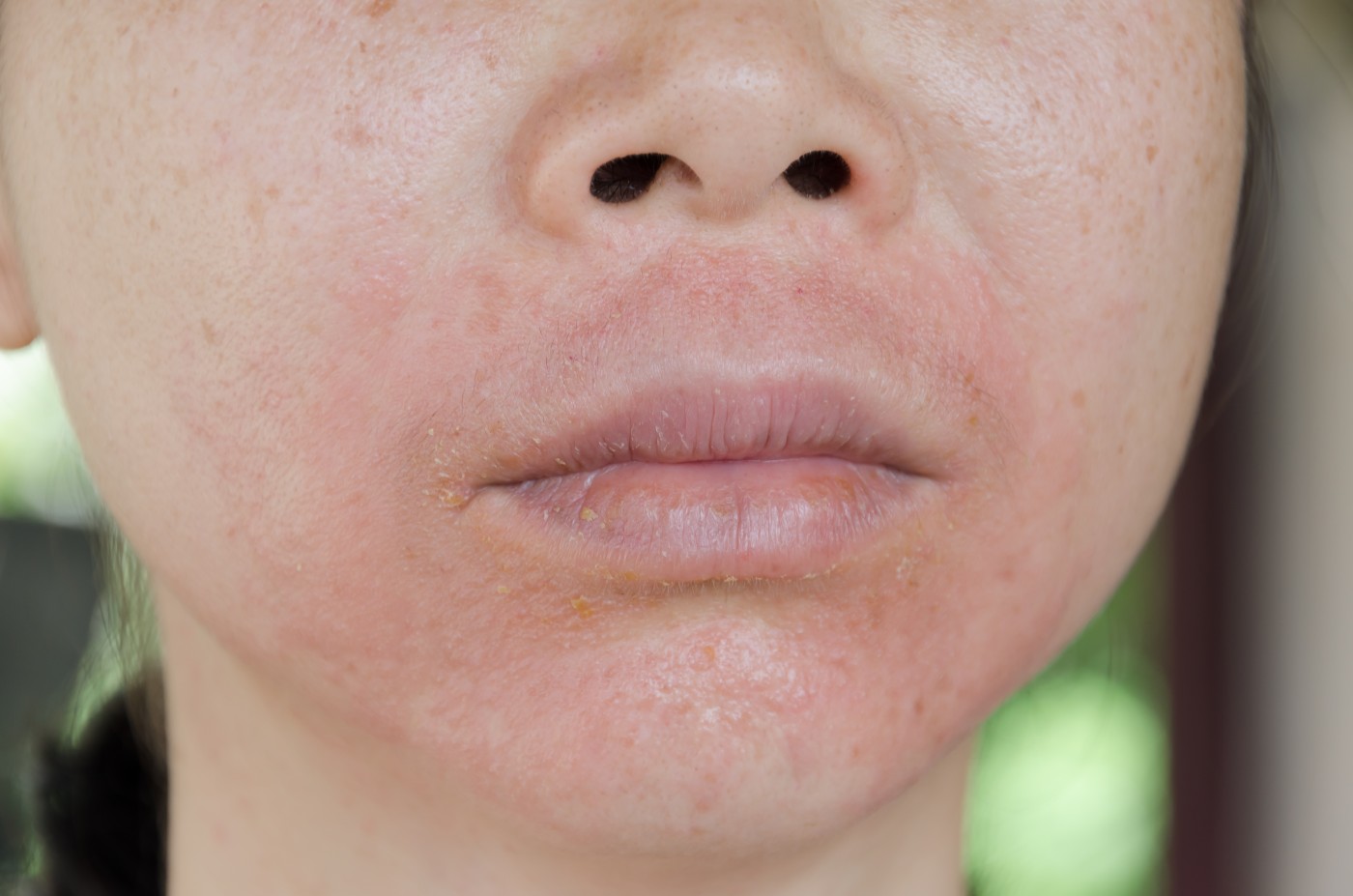
Rosacea is an inflammatory skin condition affecting mostly fair-skinned individuals. A study from the University of Copenhagen, Denmark, recently showed that the condition in women is also associated with multiple sclerosis (MS).
Recent genome wide association studies (GWAS) have pinpointed genetic risk factors of the disease that also increase risk for type 1 diabetes and celiac disease. Several other studies have shown that genetic risk factors for a number of autoimmune diseases tend to cluster, and another GWAS found as many as 90 shared genetic regions linked to rheumatoid arthritis, celiac disease, multiple sclerosis, and type 1 diabetes.
Given the large genetic overlap between various autoimmune and inflammatory conditions, the study — “Clustering of autoimmune diseases in patients with rosacea,“ published in the JAAD — set out to explore if rosacea could be linked to multiple sclerosis, as well as a number of other autoimmune diseases.
The research team identified all patients diagnosed with rosacea in Denmark between Jan. 1, 1997, and Dec. 31, 2011, as either hospital in-patients or out-patients. The team then matched each patient with five controls of the same age, sex, and calendar time. In total, the study encompasses 6,759 rosacea patients and 33,795 controls.
Within this study group, researchers then identified all individuals with an MS diagnosis, and found that patients with rosacea had a 1.5-fold increased risk of MS compared to those without rosacea. Moreover, when scientists divided the sample by sex, they noted that the association was only valid in women.
Findings also showed that including cases identified by claimed prescriptions for metronidazole — a rosacea treatment seldom used for other skin conditions in Denmark — produced similar results.
The study also reported associations between rosacea and type 1 diabetes, celiac disease, and rheumatoid arthritis.
Since the study merely made observations of diagnoses in the general population, the researchers could not prove that the conditions share disease mechanisms. Earlier studies exploring other skin conditions and autoimmune diseases have found no, or even inverse, relationships, making it likely that shared genetic or environmental factors contributing to both diseases really exist.



Lisa
Interesting. Not only do I have MS, but so do 2 of my sisters, and my mom did, too. My mom has a cousin who has been crippled with RC for decades; I have rosacea. Now if only someone would put this together resulting in real changes to these diseases.
Lisa
I meant to say "RA," for rheumatoid arthritis, not RC.
Lisa
I don't have any problems reading the site. The only way to get rid of pop-ups is to spend money on a "professional" site instead of the free one offered by WordPress.
Michelle Bike
What do you use for rosacea?
Trish
I have Progressive MS and have suffered Rosacea for years as well. When I started the Overcoming MS diet and cut out all dairy my Rosacea ceased. It does however make a return if I am stressed or when the weather gets too warm.
Shasha
HI, I need no gluten (wheat/barley/rye/oats/corn) and no dairy/soy/sugar/GMO/bad fats/saturated fat/heated oil/flax and more. People who can't have dairy usually can't have gluten. I take vitamins/good oils/minerals...probiotic...LDN...detox. LDN helps block hidden gluten. Gluten may be hidden in nuts not sold in the shell/meat basting/some spices/certified gluten free/air/some supplements and more. I detox by Far Infrared sauna (removes heavy metals/chemicals/kills Lyme/yeast etc.) and EDTA/DMPS IV chelations (removes heavy metals/unclogs blood vessels). Zinc/Mg/fish oil/HCl and enzymes with meals/Vit B12 methylcobalamin shot/intrinsic factor/MTHF/rhodiola/coenyzme Q10/coenzymated B vitamins/Vit D/Vit D3 5000IU/biotin 5000mcg and more help me. Stress may use up more zinc/B vitamins and steal progesterone to make cortisol.
ned
Hi Sasha,
Have you manageg to contain the rosacea spread
Martin Matko'
Chronic Cerebrospinal Venous Insufficiency (CCSVI) is a recognized medical condition science established in 44 Neurological afflictions !