Paramagnetic Rim Lesions Showing Promise as Diagnostic Marker of MS
Written by |
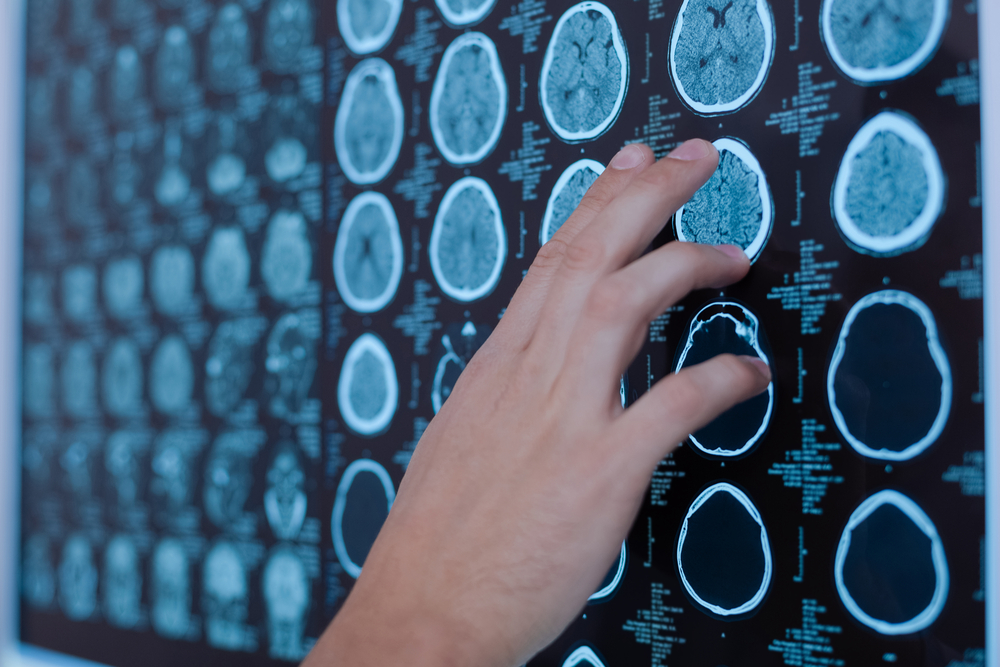
Inflammatory lesions within the brain, called paramagnetic rim lesions, visible on imaging scans may improve the accuracy of a multiple sclerosis (MS) diagnosis, especially when used in combination with other imaging-based biomarkers, a study reported.
If corroborated in larger future studies, these white matter lesions may serve as an early diagnostic biomarker.
The study, “Paramagnetic Rim Lesions Are Specific To Multiple Sclerosis: An International Multicenter 3T MRI Study,” was published in the journal Annals of Neurology.
Accurate and early diagnosis is critical in MS, where certain treatments can offer profound health benefits. But misdiagnoses can run as high as 20%, according to some estimates.
Two potential biomarkers that can be measured non-invasively by MRI are brain lesions caused by inflammation, called central vein sign (CVS) and paramagnetic rim lesions (PRL).
CVS is gaining acceptance as a biomarker for MS, while how specific PRL — found in over 50% of MS cases — is to MS is not well known.
An international team of researchers reviewed MRI records covering 329 people with MS and 83 people with non-MS neuroinflammation, looking for how frequently PRL occurred between the two.
Of the MS cases, seven were diagnosed with clinically isolated syndrome, 226 with relapsing-remitting MS, and 96 with progressive MS.
The researchers detected PRL in 172 MS patients (52%), and in six of the non-MS cases (7%).
Among those with MS, at least one paramagnetic rim lesion was found in 58% of the progressive cases and in 50% of the relapsing cases. The number of these positively correlated with disability severity scores, as measured by the expanded disability status scale (EDSS) — meaning the higher the number of PRLs, the greater was the patient’s disability level.
Although PRL detection appeared highly specific to MS (93% specificity), it did not prove to be highly sensitive (52% sensitivity), meaning that it did not always correctly identify those without MS.
By comparison, the specificity and sensitivity of using central vein sign as a diagnostic biomarker were 96% and 99%, respectively.
Combining the two biomarkers improved overall specificity to 99%, but sensitivity remained low (59%).
Still, the research team noted that this combination might prove useful in two specific scenarios. First, in cases where MS is suspected but MRI finds few CVS lesions. Second, in cases with a high frequency of CVS lesions, but where MS is not suspected.
“PRL detection might prove a valuable tool in the differential diagnostic work-up, especially for improving diagnostic specificity,” the researchers wrote. “Future prospective multicenter studies should further validate its role as a diagnostic biomarker.”


Leave a comment
Fill in the required fields to post. Your email address will not be published.