Scientists Create Oligodendrocytes From Stem Cells in Lab Dish in Just Three Weeks
Written by |
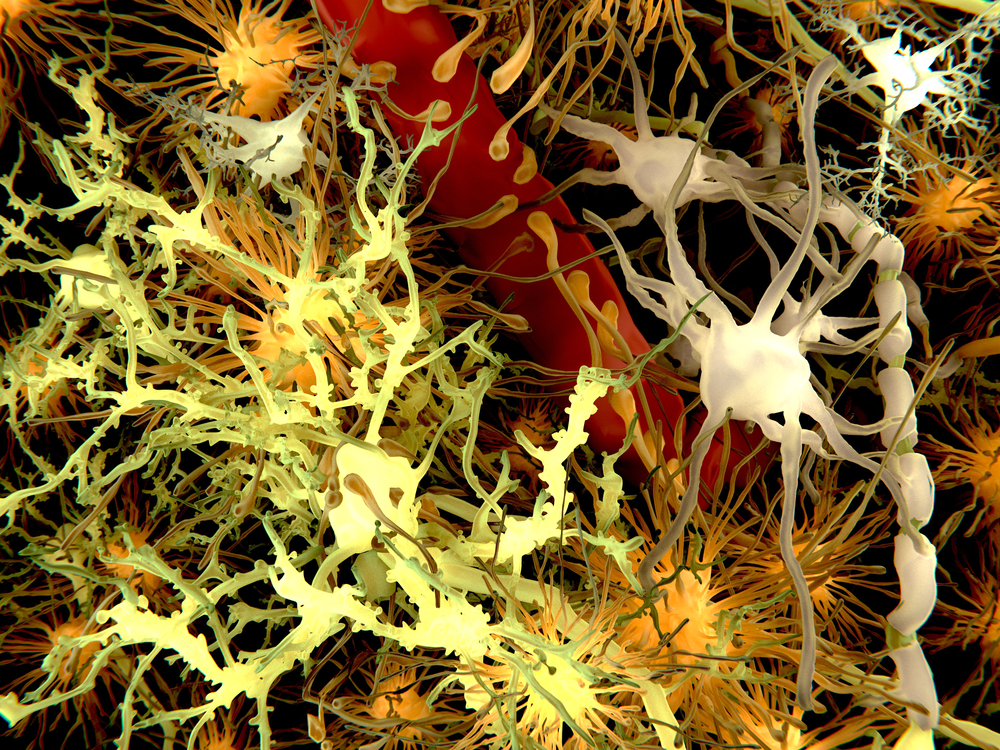
Scientists have created myelin-producing cells, called oligodendrocytes, from pluripotent stem cells derived from patients with multiple sclerosis (MS) and amyotrophic lateral sclerosis (ALS) in just three weeks.
They also demonstrated these lab-made oligodendrocytes were able to produce myelin — the fatty substance that normally wraps around neurons’ endings to protect them and is destroyed over the course of MS — when transplanted into the brain of a mouse model.
According to investigators, these specialized lab-made cells have the same properties and capacities as those found in the human brain, and therefore may be used as a platform to discover new treatments that promote myelination, as well as a cellular model of disease.
“So far, no one has developed any treatment that reverts the loss of myelin and [oligodendrocytes] in these patients, probably because there hasn’t been an appropriate platform available to study these phenomena,” Juan Antonio García-León, PhD, said in a press release. García-León is a post doctoral researcher at the University of Malaga, Spain, and first author of the study.
The experimental protocol to create these cells was detailed in the study, “Generation of oligodendrocytes and establishment of an all-human myelinating platform from human pluripotent stem cells,” published in the journal Nature Protocols.
In patients with neurodegenerative disorders like MS, the loss of oligodendrocytes — highly specialized nerve cells that are responsible for producing myelin in the central nervous system (CNS, brain and spinal cord) — is common.
The lack of oligodendrocytes can lead to a shortage of myelin in the CNS, one of the key hallmarks of MS. In addition, the loss of these specialized cells, which also are known to support neurons’ metabolic needs, can impair neurons’ metabolism and contribute to the onset and progression of ALS.
“Our knowledge and understanding of [oligodendrocyte] biology in disease conditions are limited, probably in part because available animal models poorly reproduce some … specific features of these diseases,” the investigators wrote.
Furthermore, “poor access to primary human oligodendroglia and difficulties in maintaining and expanding these cells … have hampered research in this area,” they added.
Investigators now described a method that allowed them to rapidly and efficiently create oligodendrocytes in a lab dish from eight different lines of pluripotent stem cells derived from human donors, including four from patients with MS and ALS.
As a first step, investigators treated pluripotent stem cells with a combination of factors for approximately eight days to transform them into oligodendrocyte precursor cells.
These progenitor cells then were induced to grow into mature oligodendrocytes by forcing them to produce SOX10, a transcription factor that is known to promote oligodendrocyte differentiation. (Transcription factors are proteins that can control the activity of certain genes.)
After about 10 days, more than 60% of the cells were producing O4, a marker of oligodendrocyte progenitors that are well on their way to become oligodendrocytes. In this subset of cells, about 20% also produced myelin basic protein (MBP), a marker of mature oligodendrocytes.
Investigators also showed that when transplanted into the brain of mice that lacked myelin as well as a functional immune system, the lab-made oligodendrocytes were able to produce myelin.
The entire procedure — from immature pluripotent stem cells to mature oligodendrocytes — took approximately three weeks (20–22 days) to complete. According to the researchers, this protocol is faster and more efficient than previous methods, which normally require three to six months to generate low numbers of fully mature oligodendrocytes.
“In summary, here, we present a protocol for fast and efficient generation of human oligodendrocytes from a virtually infinite cell source that have functional properties similar to primary oligodendrocytes and can be used for assessing the effect of myelinating strategies and for disease modeling,” the researchers wrote.
According to García-León, a biotechnology company already implemented this new method in an attempt to develop new therapies to revert myelin loss in MS patients.
The team is now collaborating with other groups of investigators to expand the application of the new protocol to other diseases.
Leave a comment
Fill in the required fields to post. Your email address will not be published.