Are MS Patients Using Too Many Medications?
Written by |
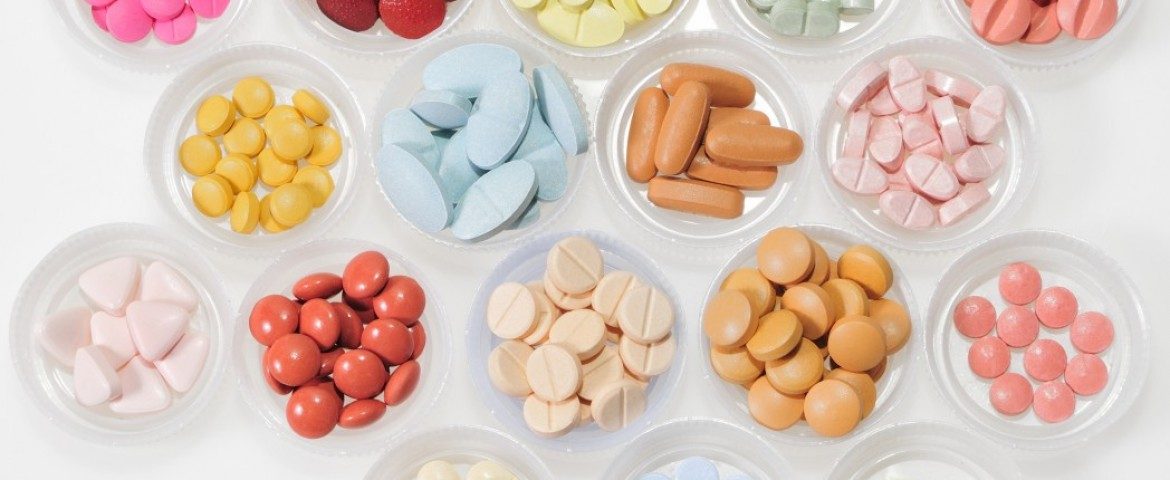
Have you ever heard of the word “polypharmacy”? I saw the word for the first time today. It’s generally defined as taking many medications together. There’s been debate over how many is “many,” but a number generally used is five or more.
That describes me. I take six prescription drugs every day. Four of them are directly related to my MS, the fifth is to moderate my cholesterol, and the sixth is to keep my thyroid level where it should be. There’s also a baby aspirin, vitamin D3, and calcium. But who’s counting? It’s probably a good bet that you take as many medications as I do, so we both probably should be counting, because polypharmacy could be particularly troubling for us.
Polypharmacy is usually considered primarily to be a problem for older people. But according to a study recently published by Plus One, “In persons with chronic morbidity such as MS patients, polypharmacy can give rise to considerable health problems.”
The research, from the University of Rostock in Germany, found that 30.3 percent of the 145 relapsing-remitting MS patients who participated were taking five or more meds every day. The average number of meds was 3.6. The most common medication was one of the disease-modifying therapies — nearly 95.9 percent were using one. Dietary supplements were used by 33.8 percent. An analgesic for pain control was used by 29 percent. Strangely, at least to me, only 9 percent were using medications for bladder control and only 6.9 percent used muscle relaxants.
Discuss the latest research in the MS News Today forums!
According to a 2017 article on the U.S. Pharmacist website, “Polypharmacy increases the risk of adverse reactions to medications. The more drugs, the higher the risk of drug interactions. Research has shown that patients taking five to nine medications have a 50% chance of an adverse drug interaction, increasing to 100% when they are taking 20 or more medications.”
This can really become a problem when more than one doctor is prescribing medications and when our prescriptions are filled at more than one pharmacy. We all know that too many of our primary care physicians and neurologists have difficulty communicating with each other.
What to do?
The authors of the University of Rostock study write, “For avoiding drug interactions and their clinical consequences, a well thought-out medication management that is based on the optimization of drug use is vital.” They suggest that physicians routinely check to see if “all medications are indeed essential and up-to-date.” They also suggest that doctors consider “non-drug approaches such as physiotherapy” to reduce the use of medications.
But we as patients can also do things to help ourselves. An article on the JAMA Network website lists several ideas. They include:
- Make a list of your medications, including over-the-counter, and review it with all of your physicians.
- Know the purpose of each of your meds.
- Ask your physicians if you might eliminate some of your meds to avoid polypharmacy problems.
How many meds are you on? When was the last time you reviewed all of them with your doctors or pharmacist?
You’re invited to visit my personal blog at www.themswire.com.
***
Note: Multiple Sclerosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Multiple Sclerosis News Today or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to multiple sclerosis.



Cyn Doyle
I noticed that you have MS and also thyroid problems.....I wonder how many people with MS also have underactive thyroid....as I do , too.
I only take 4 prescribed drugs...Fampyra [ to aid walking] , Synthroid, Oxybutanin [for bladder problems] and medical cannabis [for pain , spasticity, and to help me sleep]
I have never taken DMD'S
I take 4000iu of vit.D3, too.
Interesting that so many people , especially seniors, are on so many prescription drugs.I am fortunate to have a doctor who believes that seniors are given too many prescriptions.
Interesting article....thanks
Ed Tobias
Good question about thyroid problems.
I haven't read anything about a connection, though I do know that a variation in thyroid function is one of the side effects of Lemtrada.
I wish you well with your meds, vitamins and MMJ for your symptoms without needing any DMTs.
Ed
Julie Farkas
You don't have a polypharma problem, you have a multiple autoimmune problem. It's called Multiple Autoimmune Syndrome (MAS) and it's time that more research be devoted to this problem.
Cynthia Kingo
I have Hashimoto's thyroid as well as ms.
Julie Farkas
Thyroid problems are the foundation of a dysfunctional immune system. If you have Multiple Autoimmune Syndrome (MAS) you almost always have an autoimmune thyroid problem, an autoimmune skin disorder, and one or more of the other 80 autoimmune disorders.
Lisa
Hypothyroidism in 2011 and ND in 2018. I take levothyroxine, vitamin D and glatiramer acetate shots. Refused to take the baclofen cos it made me feel sick. Actually could use a few more (numb legs, balance issues, bladder blahs, migraines, chronic anxiety, etc) but I hate taking meds as it is so I guess it works out.
LINDA Fitch
Yes I do take many medications, I always carry an updated list including dose, times per day and why and who prescribed it for me in my purse. I hand it over at each Dr. appt making sure the date as “last updated on” as that day and include my name and date of birth and allergies. I have them make a copy every visit, then I make changes as needed change the date for the next doctor and so forth.
I’d rather not take so many but several, and I mean several have replaced the one minimal dose one opiate I was on for pain. I don’t like the several substitutes I have been forced to try just to function at a level I was minimally successfully at before Uncle has inserted his nose into my and my doctors healthcare relationship.
BTW, everyone should know what they are on and why they are on it! They should also know when prescribed a new drug if it will adversely react with what they are on already and what side effects to watch for! Don’t expect your doctor to monitor your medications for you, or your insurance co, or your pharmacy.... Especially when you have an incurable disease and are getting on in years, they may think you cost too much already.
Allan Newson
Cheese and rice I'm the definition of the story. I'm currently on lemtrada and 18 pills in the morning and during the day three pills of baclofen 20mg then at night I ONLY take six at night including a "doctor approved" overdose of lyrica due to the extreme burning sensation in both my feet. I have sometimes had a blunt instead of all the pills. I feel a lot better afterwards not taking anything but lyrica. I would completely go to a weed based therapy but,it's not legal in Wisconsin. Hopefully sooner than later weed will be legalized in the state.
Catherine
I have an under active thyroid too, and also rheumatoid arthritis that I understand is common for others with MS. I take tecfidera and gabapentin for MS, hydroxychloroquine for the arthritis and levothyroxine for my thyroid problem. My Rheum consultant thought tecfidera might help with the arthritis too, and certainly I have been stable since starting tecfidera 2 years ago. I also take vitamins D3 & B12, Biotin and CBD oil for MS, and Macushield for eye-health. I try not to rattle when I walk!
Stacey Guenther
I take ten pills in the morning and ten at night. i’m only 40 years old. Two of the pills in the morning are my daily vitamin and a Super B-Complex vitamin. The rest are prescriptions. I have GERD, lots of MS pills for the various symptoms and pills for the depression and anxiety. My GP doesn’t like me being on so many pills and I’m going to try to stop taking some of the depression and anxiety pills and just live with the depression. I may also be able to give up the medication I am taking for cognitive and memory problems because it doesn’t seem to be helping. So, if doctors agree with me, I would like to give up three of the prescriptions. I don’t like being on so many presciptions.
Laurie
I was on 16 meds at one time. After having heart issues, and my cardiologist being serious, that a 49 year old woman was on so many meds I took myself off all but three I have recently found myself slowly, getting back on the majority of the meds that I had came off of. I hate having to be on so many meds, but I hate MS more I do believe that when we have an incurable disease, we must have quality of life and sometimes that is having to be on a lot of meds, unfortunately. My new team of doctors do well at working together and trying to use as fewer meds possible and meds that address multiple issues with 1 pill vs multiple pills. However, I still worry about the affects off so many meds on my body and drug interactions. My biggest issues are pain control and, heart issues, and insomnia. To all my warrior friends/family....keep fighting the daily fight and praying that someday they find a cure for this cruel disease!