Hematopoietic Stem Cell Transplantation: MS Breakthrough Treatment Or Another “Liberation Therapy” Disappointment Shaping Up?
Written by |
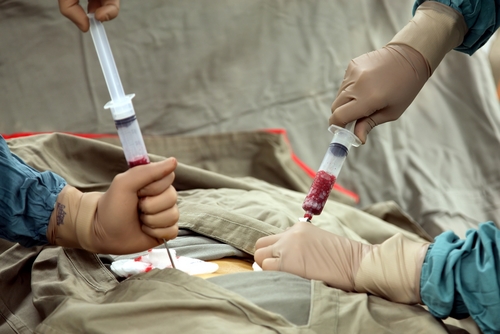
 Multiple Sclerosis (MS) is a devastating disease for many who become afflicted with the disease’s progressive form, often in the prime of their lives, with no cure and when the effectiveness of established MS treatment is so often disappointing. Discouragement can lead to pinning premature hope on unproven therapies that seem to hold promise.
Multiple Sclerosis (MS) is a devastating disease for many who become afflicted with the disease’s progressive form, often in the prime of their lives, with no cure and when the effectiveness of established MS treatment is so often disappointing. Discouragement can lead to pinning premature hope on unproven therapies that seem to hold promise.
For example, with chronic cerebrospinal venous insufficiency (CCSVI or CCVI) — the so-called “liberation therapy” developed by Italian researcher Paolo Zamboni in 2008, — Dr. Zamboni hypothesized that compromised flow of blood in the veins draining the central nervous system played a role as the cause or in the development of multiple sclerosis, and devised a procedure dubbed “liberation therapy” by the media that involves angioplasty (stenting) of key veins in an attempt to improve blood flow.
CCSVI was and still is greeted with skepticism within the medical community, and Wikipedia’s entry on the topic notes that Dr. Zamboni’s first published research was neither blinded nor did it have a comparison group, and that Dr. Zamboni also did not disclose his financial ties to Esaote, manufacturer of the ultrasound specifically used in CCSVI diagnosis.
The so-called “liberation procedure” has also been criticized for possibly resulting in serious complications and deaths while its benefits have not been proven, with the United States Food and Drug Administration’s position being that it is not clear if CCSVI exists as a clinical entity, and that these treatments may cause more harm. Wikipedia notes that CCSVI research has been fast-tracked, but researchers thus far still have been unable to confirm whether CCSVI has a role in causing MS, consequently raising serious objection to the hypothesis of CCSVI originating multiple sclerosis. Research continues, and a 2013 study found that CCSVI is equally rare in people with and without MS, while narrowing of the cervical veins is equally common.
This writer is personally aware of specific cases in which CCSVI has seemed to result in substantial improvement in MS symptoms, and others where it proved ineffective. The jury, as they say, is still out, but a cautious approach seems to be prudent.
[adrotate group=”4″]
Likewise for another controversial new therapy being advocated for MS and other autoimmune diseases, known as “high-dose immunosuppressive therapy with hematopoietic stem cell transplantation in MS and other autoimmune diseases,” in which clinicians destroy the patient’s immune system with chemotherapy, and then “reboot” it with stem cells. Dr. Denis Federenko of the A.A. Maximov Hematology and Cell Therapy Department of the National Pirogov Medical Surgical Centre in Russia specializes in this treatment, pointing out that conventional therapies do not provide satisfactory control of multiple sclerosis; hormonal therapy helps to limit acute manifestations of the disease, but doesn’t stop its progression; and Interferon therapy may help some patients, but in most cases it does not provide a stable long-term effect.
The Russian proponents of this approach to treating MS contend that chemotherapy eliminates the cause of the disease — the autoimmune T-cells that are responsible for nerve tissue damage. Then the patient is transplanted with his/her own (autologous) stem cells, which were collected and frozen in advance. They say that over the past decade more than 700 patients have received this treatment, which they claim “may” stop progression of the disease in “most” patients and prevent further deterioration of their quality of life, and that MS patients will not need any maintenance therapy after transplantation. Claimed efficiency of high-dose immunosuppressive therapy with hematopoietic stem cell transplantation in multiple sclerosis approximates 75%-80%, and is most effective in young patients with rapidly progressing multiple sclerosis in its early stages, when the leading mechanism of the damage to the nervous system is autoimmune inflammation. In later stages of the disease, after irreversible damage is done, they caution that transplantation’s effect is limited.
 In an opinion statement entitled ” Autologous hematopoietic stem cell transplantation as a treatment option for aggressive multiple sclerosis” (Curr Treat Options Neurol. 2013 Jun;15(3):270-80. doi: 10.1007/s11940-013-0234-9) published in the journal Current Treatment Options in Neurology, N. Pfender, R. Saccardi, and R. Martin of the Department of Neurology at University Hospital Zurich in Zurich, Switzerland, observe that “Despite the development of several injectable or oral treatments for relapsing-remitting multiple sclerosis (RRMS), it remains difficult to treat patients with aggressive disease, and many of these continue to develop severe disability.”
In an opinion statement entitled ” Autologous hematopoietic stem cell transplantation as a treatment option for aggressive multiple sclerosis” (Curr Treat Options Neurol. 2013 Jun;15(3):270-80. doi: 10.1007/s11940-013-0234-9) published in the journal Current Treatment Options in Neurology, N. Pfender, R. Saccardi, and R. Martin of the Department of Neurology at University Hospital Zurich in Zurich, Switzerland, observe that “Despite the development of several injectable or oral treatments for relapsing-remitting multiple sclerosis (RRMS), it remains difficult to treat patients with aggressive disease, and many of these continue to develop severe disability.”
The authors observe that over the last two decades, hematopoietic stem cell transplantation (aHSCT or HSCT) has been explored, and clinical studies have shown that aHSCT is able to completely halt disease activity in the majority of patients with aggressive RRMS, and that research on the mechanisms of action supports that aHSCT indeed leads to renewal of a healthy immune system.
However, not everyone is on board. The Australian government has issued two public statements on HSCT therapy (https://sixtyminutes.ninemsn.com.au/img/2014/StemCells1.pdf and https://sixtyminutes.ninemsn.com.au/img/2014/StemCells2.pdf), both noting that while stem cell transplant is an accepted therapy for conditions such as multiple myeloma (cancer of the plasma cells) and lymphoma (a type of blood cancer) and is routinely provided at Canberra Hospital for these conditions, and while HSCT has also been used for patients with severe and rapidly progressive multiple sclerosis (MS), it is not widely accepted for this use, with limited research data on the efficacy and outcomes of this treatment from studies undertaken to date.
Furthermore, the statement contends that for the majority of patients with MS, particularly those with the remitting/relapsing form of the disease, HSCT may pose more risks than long term benefits, and accordingly is only suitable for a very specific group of patients, with St. Vincent’s Hospital in Sydney having a program for stem cell transplant for patients with MS, but with strict eligibility criteria, reflecting the limited cohort of patients for whom this treatment may be considered an option.
This policy has convinced some Australian MS patients to consider medical tourism to Russia’s National Pirogov Medical Surgical Centre for HSCT therapy according to a report last weekend in the Brisbane East News about one such case that also quotes Griffith School of Medicine Dean Professor Simon Broadley saying HSCT treatment had not proven its effectiveness in phase-three trials and anecdotal evidence suggested it may only work in the early stages of MS.
Producer Stephen Rice of the antipodean version of the investigative newsmagazine TV program 60 Minutes, challenges the Canberra Hospital/ACT Health stance on HCST in a set of questions he says have gone largely unanswered. For example:
“You say this treatment (stem cell transplant) is ‘not widely accepted for this use, with limited data on the efficacy and outcomes of this treatment from studies undertaken to date.’ Are you aware of multiple peer-reviewed studies by Dr Richard Burt, Dr. Nikolai Pfender, Dr Riccardo Saccardi and others, published in journals such as the Lancet, JAMA and Current Treatment Options in Neurology, confirming the treatment ‘is able to completely halt disease activity in the majority of patients’?” and “Are you aware that Dr Colin Andrews has successfully used this treatment at Canberra Hospital on at least six patients with good results in all cases?”…. so “why has Canberra Hospital stopped Dr. Andrews offering this procedure?”
You can read all twelve of Mr. Rice’s questions at:
https://sixtyminutes.ninemsn.com.au/img/2014/StemCells3.pdf
 And official Aussie skepticism notwithstanding, back in the U.S. Dr. Richard K. Burt, Chief, Division of Immunotherapy at the Northwestern University Feinberg School of Medicine in Chicago, Illinois is an established international researcher in the field of hematopoietic stem cell transplantation for autoimmune diseases. Dr. Burt performed either America’s first or the world’s first autologous (one’s own) hematopoietic stem cell transplants for numerous immune mediated diseases.
And official Aussie skepticism notwithstanding, back in the U.S. Dr. Richard K. Burt, Chief, Division of Immunotherapy at the Northwestern University Feinberg School of Medicine in Chicago, Illinois is an established international researcher in the field of hematopoietic stem cell transplantation for autoimmune diseases. Dr. Burt performed either America’s first or the world’s first autologous (one’s own) hematopoietic stem cell transplants for numerous immune mediated diseases.
Among Dr. Burt’s many published works, he is lead co-author of a 2009 report on HSCT published in the journal The Lancet Neurology entitled “Autologous non-myeloablative haemopoietic stem cell transplantation in relapsing-remitting multiple sclerosis: a phase I/II study “ (Published online January 30, 2009 DOI:10.1016/S1474-4422(09)70017-1 1) evaluating the safety and clinical outcome of autologous non-myeloablative haemopoietic stem cell transplantation in patients at Northwestern Memorial Hospital with relapsing-remitting multiple sclerosis (MS) who had not responded to treatment with interferon beta. Among the study’s conclusions is that most patients with MS initially present with intermittent symptoms that are commonly, at least partially, reversible — the form of the disease is termed relapsing-remitting MS. However, the researchers report that over time, most patients eventually develop secondary-progressive MS, which manifests as irreversible and gradual neurological impairments that often progress without acute relapses.
The Division of Immunotherapy and Autoimmune Diseases (DIAD) at Northwestern University claims to be the only center in the world devoted to the area of treatment and research that provides intensive immunosuppression and hematopoietic stem cell transplantation for patients with severe autoimmune diseases, and since its establishment, basic and clinical research has been an integral part of the DIAD’s work. Working collaboratively with the scientists of Northwestern University Feinberg School of Medicine, DIAD physicians are translating research advances discovered in the laboratory into more effective treatment approaches and prevention strategies for our patients.
Additionally, Northwestern University, the University of Calgary, Canada, and the University of Sao Paulo, Brazil, have partnered to offer patients with relapsing-remitting inflammatory MS, a randomized study utilizing autologous stem cell transplantation versus the FDA approved standard of care (i.e. interferon, Copaxone, mitoxantrone or Tysabri.
A report by H.L. Atkins and M.S. Freedman of the Ottawa Hospital Research Institute in Ottawa, Canada, published in the Neurotherapeutics (2013 Jan;10(1):68-76. doi: 10.1007/s13311-012-0162-5) notes that “Increasing clinical experience has refined patient selection criteria and management in the peri-transplant period leading to a reduction in treatment-related complications,” and that “HSCT, when used to treat patients with aggressive highly active multiple sclerosis, can reduce or eliminate ongoing clinical relapses, halt further progression, and reduce the burden of disability in some patients, in the absence of chronic treatment with disease-modifying agent.” The coauthors go on to discuss what they deem the top 10 lessons learned about aHSCT in reviewing the more than 600 autologous hematopoietic stem cell transplants that have appeared in the medical literature over the last one and one-half decades.
These are:
Lesson 1: While MS Patients Generally Behave like Other Patients Undergoing HSCT, They Experience Unique Issues
Lesson 2: Increasing Experience Using HSCT for Patients with MS Reduces Morbidity and Mortality
Lesson 3: CNS Toxicity of Very High-Dose Regimens may Adversely Influence Outcomes
Lesson 4: HSCT is More Likely to be Effective for MS Patients with Active CNS Inflammation
Lesson 5: HSCT is Effective at Controlling Inflammatory MS Activity, with Higher Response Rate Observed with More Intense Conditioning Regimens
Lesson 6: HSCT can Result in Long-Term Progression-Free Outcomes
Lesson 7: The Recovery of Functional Ability can Occur in HSCT Recipients
Disability, as measured by the EDSS can improve after HSCT, at least for some patients.
Lesson 8: Tolerance can Develop Resulting in Obliteration of Autoimmunity while Preserving Protective Immunity
Lesson 9: The Reconstituted Immune System Retains a Predisposition to Autoimmunity
Lesson 10: Information on the Economics and Health Resource Usefulness of HSCT for MS Needs to be Gathered
For full elucidation of these ten points, visit:
https://www.ncbi.nlm.nih.gov/pubmed/23192675
 Drs. Atkins and Freedman summarize that in the worldwide experience big picture, HSCT performed for patients with severe MS for the last 15 years has shown us the usefulness of this treatment, and more importantly has provided a new treatment paradigm in which the immune system is repaired rather than suppressed. They observe that HSCT appears most beneficial for patients with highly active MS who are progressing and who are refractory to conventional MS therapies, and that HSCT can be performed with acceptable treatment-related morbidity and little mortality. Moreover, they say selected subpopulations, such as patients with malignant MS, may benefit even more substantially from HSCT. However they caution that further studies are required with more evidence regarding the role of HSCT in the treatment of MS provided from a long-term, follow-up study of patients. They say the body of evidence demonstrating a role for HSCT in MS has helped to refine which questions remain unanswered, such as why although HSCT can be used as a salvage therapy, it seems to work better earlier in the course of MS, when relapses dominate the clinical picture, and could HSCT provide better outcomes in this group of patients compared to current or new immunosuppressive agents, especially with the increasing risk of toxicity with long-term use of newer agents?
Drs. Atkins and Freedman summarize that in the worldwide experience big picture, HSCT performed for patients with severe MS for the last 15 years has shown us the usefulness of this treatment, and more importantly has provided a new treatment paradigm in which the immune system is repaired rather than suppressed. They observe that HSCT appears most beneficial for patients with highly active MS who are progressing and who are refractory to conventional MS therapies, and that HSCT can be performed with acceptable treatment-related morbidity and little mortality. Moreover, they say selected subpopulations, such as patients with malignant MS, may benefit even more substantially from HSCT. However they caution that further studies are required with more evidence regarding the role of HSCT in the treatment of MS provided from a long-term, follow-up study of patients. They say the body of evidence demonstrating a role for HSCT in MS has helped to refine which questions remain unanswered, such as why although HSCT can be used as a salvage therapy, it seems to work better earlier in the course of MS, when relapses dominate the clinical picture, and could HSCT provide better outcomes in this group of patients compared to current or new immunosuppressive agents, especially with the increasing risk of toxicity with long-term use of newer agents?
The Canadian researchers say a proposed international multicenter, collaborative, randomized clinical trial of HSCT compared to the best standard-of-care treatment will improve the understanding of the role that HSCT should play in the management of MS, and that clinical experience using HSCT for patients with other CNS autoimmune demyelinating diseases (e.g., neuromyelitis optica) is just starting to be documented. Further detailed cohort and registry studies will help determine whether HSCT is able to fill this unmet clinical need, and they conclude that although HSCT remains a “sledgehammer approach” to treating MS, reserved for those with the most aggressive forms, opportunity exists to capitalize on growing knowledge and experience in the field in order to create less toxic methodologies for eliminating and replacing the immune system toward the goal of broader applicability of this promising therapy.
It does seem that hematopoietic stem cell transplantation has a vastly deeper and sounder base of research supporting it as an MS treatment option than does chronic cerebrospinal venous insufficiency , and Drs. Atkins and Freedman’s positive but cautious approach seems most commendable pending results of the further research they recommend.
Sources:
A.A. Maximov Hematology and Cell Therapy Department of the National Pirogov Medical Surgical Centre
Division of Immunotherapy and Autoimmune Diseases (DIAD), Northwestern University Feinberg School of Medicine
Current Treatment Options in Neurology
Neurotherapeutics
The Lancet Neurology
Sixty Minutes (Australia)
Canberra Hospital/ ACT Health (Government of Australia)
Wikipedia