Lipoatrophy Occurrence for MS Patients Higher than Originally Thought
Written by |
 The risk of developing lipoatrophy for multiple sclerosis (MS) patients administrated with glatiramer acetate is greater than 60 percent, according to a study developed at the Riverside Medical Clinic that reviewed 73 MS patients. It was already known that the drug could cause the condition, however the rate is higher than what was originally thought, according to the study.
The risk of developing lipoatrophy for multiple sclerosis (MS) patients administrated with glatiramer acetate is greater than 60 percent, according to a study developed at the Riverside Medical Clinic that reviewed 73 MS patients. It was already known that the drug could cause the condition, however the rate is higher than what was originally thought, according to the study.
It is “substantially higher than previously reported and is often the sole factor prompting patients to switch to another MS disease-modifying therapy. Our data also suggest that a heightened risk of lipoatrophy is an inherent autoimmune problem and is not necessarily mitigated by vigilant injection-site rotation. The psychological consequences may be significant,” said investigator Dr. Ronald Bailey, director of the MS clinic at the Riverside Medical Clinic.
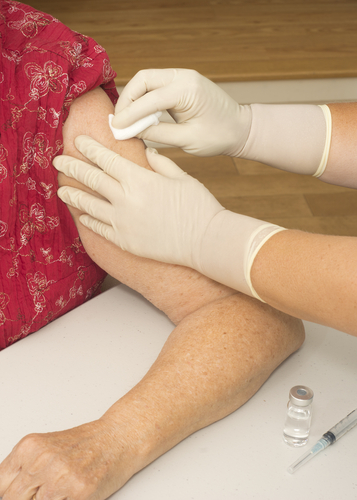
From the patients who received the glatiramer acetate (Copaxone) therapy, 63 percent, or 46 participants in the study, developed lipoatrophy. Most of the patients were women, and 55% of them were administrated the drug with an auto injector. Copaxone is a daily subcutaneous injection that works as a disease-modifying therapy, and is widely used n treatment of RRMS. Lipoatrophy is a condition characterized by the loss of subcutaneous fat, and may lead to disfiguration.
In the research, it was also noted that there was no improvement in the dents that appear on the surface of the skin associated with the condition during the 3-year observation period. Scientists also performed photographic documentation and instructive guides about the proper injection process. The reason for the correlation between Copaxone and lipoatrophy is still not fully understood, but Dr. Baily believes that perhaps “an elevation in tumor necrosis factor–alpha causes a dedifferentiation of adipocytes in the subcutaneous tissue.”
The disease “appears to progress, even when you stop the injections. It’s a pretty impressive disfiguration. It’s important to emphasize that this isn’t necessarily going to be remedied with plastic surgery. However, if patients were stable, most of them thought that this was a small price to pay to be in remission,” Dr. Bailey said at a meeting of the Consortium of Multiple Sclerosis Centers and the Americas Committee for Treatment and Research in Multiple Sclerosis.
Some of the patients developed Lipoatrophy in the first three months of the treatment, which suggested an autoimmune reaction, according to the research. “Upon GA treatment discontinuation, lipoatrophy remained permanent,” he noted. GA labeling alerts to a 2 percent risk with a 20-mg/mL daily dose and 0.5% with the 40-mg/mL three times weekly option. The former one is used for almost two decades, while the latter was approved this year by the Food and Drug Administration.
“Lipoatrophy is thought to be permanent. There is no known therapy. To assist in possibly minimizing these events, the patient should be advised to follow proper injection technique and to rotate injection sites with each injection,” according to the GA label. However, another study performed at the Riverside Clinic concluded that site rotation wouldn’t decrease the probabilities of developing the condition.
A different study reported, on the other hand, that copaxone could block the induction of autoimmune encephalomyelitis. An experiment performed with mice suggested that glatiramer acetate-specific suppressor T-cells are induced and activated in the periphery. The combination of the estrogen hormone estriol with Copaxone was proven effective to improve the symptoms of relapsing remitting multiple sclerosis patients.



Maggie LaCombe
My thighs, inside and out, are terribly indented from Copaxone. I see insurance is now paying for HIV lipoatrophy surgery/treatment. Do you know if it has been looked into about MS patients who were on copaxone to get surgery/treatments?
Lee Marshall
My brother has injected copaxon successfully for 15 years. This year he had to start injecting long acting insulin, and now he has lipohypertrophy so badly that when he tries to inject copaxon, the liquid won't come out of autoinjector. Any suggestions for him? He's going to have to go off the copaxon, and we're worried about his MS.
Thanks,
Ms. Lee Marshall