#AANAM — Tysabri Lowers Serum Neurofilament Light Levels in SPMS Patients, Phase 3 Trial Finds
Written by |

Treatment with Tysabri (natalizumab) lowers the levels of the biomarker serum neurofilament light chain (sNfL) in patients with secondary progressive multiple sclerosis (SPMS), according to data from a Phase 3 trial.
Findings also revealed that higher levels of sNfL correlated with MS lesions and disease activity prior to starting the therapy, and with the extent of future brain atrophy.
Hans-Peter Hartung, MD, presented the study, “Natalizumab Reduces Serum Concentrations of Neurofilament Light Chain in Secondary Progressive Multiple Sclerosis Patients From the Phase 3 ASCEND Study,” at the 2019 American Academy of Neurology (AAN) annual meeting, being held through May 10 in Philadelphia. Hartung is a professor and chairman of the department of neurology at Heinrich Heine University in Germany.
Although not specific to MS, sNfL has been proposed as a biomarker of nerve cell damage, disease activity, and treatment response in relapsing-remitting MS (RRMS). However, the potential of sNfL as a biomarker in SPMS patients is unclear.
Aiming to address this, the team of researchers evaluated the link between sNfL levels and disease activity, disability progression, and response to Biogen’s Tysabri in patients who had had SPMS for at least two years and who participated in the Phase 3 ASCEND trial (NCT01416181).
sNfL levels were measured with the SIMOA NF-light Advantage Kit (developed by Quanterix) at the start of the Biogen-sponsored ASCEND trial, and at 48 and 96 weeks. A total of 379 patients taking Tysabri (mean age of 47.4 years), and 365 on placebo (mean age of 47.5 years) were evaluated.
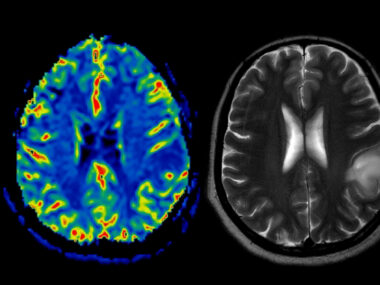
Results showed that sNfL levels at baseline (start of the study) were significantly associated with the number of gadolinium (Gd+)-enhancing T1 lesions on magnetic resonance imaging (MRI) scans — areas of active inflammation and disease activity — and T2 lesion volume, which refer to both old and new lesions.
At baseline, higher sNfL levels also correlated with less ability to walk, as assessed by the Timed 25-Foot Walk test (T25FW) — or the time it takes to walk 25 feet as quickly and safely as possible — and with fewer hand and finger skills, measured with the Nine-Hole Peg Test (9HPT). The data further showed that higher sNfL levels were also linked to more brain shrinkage, or atrophy, over 96 weeks.
At 96 weeks, sNfL concentrations were significantly higher in patients with disability progression than in those without progression during the study, as assessed through the Expanded Disability Status Scale, plus the T25FW and 9HPT tests.
Compared with placebo, patients treated with Tysabri had significantly lower sNfL levels at 48 and 96 weeks.
Significantly different sNfL levels were observed in patients with and without T1 lesions at baseline, relapses in the two years preceding the study, and with inflammatory activity — T1/T2 lesions or relapses — during the trial. However, sNfL concentrations were reduced in all patients treated with Tysabri regardless of initial lesion load (Gd+ status), “regardless of relapses over two years before the study,” and “regardless of inflammatory activity during the trial,” Hartung said.
These results indicate that Tysabri decreased sNfL levels in SPMS patients “with or without evidence of acute inflammatory activity (Gd+ lesions, new T2 lesions, and relapses),” Hartung said, suggesting that this biomarker may reflect both acute inflammation-driven lesions and chronic neurodegeneration in MS.
Similar to observations in RRMS patients, “baseline sNfL concentrations in participants with SPMS in the ASCEND study were associated with baseline disease activity measures and future brain atrophy rates over a 96-week period,” Hartung concluded.
However, he emphasized that more studies are needed to better understand the role of sNfL as a potential biomarker in SPMS.
Of note, 20 of the study’s authors have received research support or personal compensation for consulting, serving on a scientific advisory board/board of directors, speaking, or other activities by Biogen. Thirteen hold stock and/or stock options in the company.


Loisanne Abraham
I have been on tecfidera,Copaxone and gilenya so far and none has helped. What would u suggest I should try next. My doctor is no help she just dismisses me always and I don't know what is the best route to take. So any help would be nice.
Martin
Save MS Healthcare Facilitate Research & Establish Venous Cerebrospinal Blood Flow Treatment/s, as Baseline Primary Care Optionl Treating Neurovascular Disease! Many Feel/Know #CCSVI is a Recognized Medical Condition Science Confirmed Causative Factor so called MS Role/Part 43 Other So Called Neurological Afflictions!
'“To be effective, our health care system needs restructuring to focus on prevention and addressing root causes of disease. Overcoming this challenge is the greatest hurdle facing public health today. It has little to do with science or with technology, but rather with regulation and public policy."'
Supplying Oxygen & Nutrients to Every Cell in the Body, Blood & Circulation including activity and exercise ARE Building Blocks of life, having made yourself what you are functioning today! #CCSVI is a congenital Science confirmed recognized Medical condition established causative factor MS & Role/Part 43 other so called Neurological afflictions!
#CCSVI
Venous Hypertension
>microbleedings
>iron
>inflammation
>free radicals
>neurodegeneration
#multiplesclerosis
M.S. - Mystery Solved
Mysterious Autoimmunity
= CCSVI Neurodegeneration
DJ Hartt
Why do these these results matter when Tysabri has already failed to halt progression in the SPMS ASCEND trial?
Why do the results matter when other studies show loss of brain volume in grey matter or progression of disease despite being on Tysabri ("Gray matter atrophy in multiple sclerosis despite clinical and lesion stability during natalizumab treatment,” was published in the journal PLOS ONE)?
It is time for a revolution in progressive MS research. The only person that immunosuppressants are helping is Pharma, along with its shareholders and COI researchers + neurologists.
Jennifer
I have had MS for 31 years now and am now 58 yo. Have taken supplements incl. D, flaxseed, B12 and multiple vitamin. Am waiting on the ok from my nephrologist to increase D from 1to 4,000 units/day. I am minimally disabled..can still walk, just not fast. Believe any cure will include D.