How sleep apnea and multiple sclerosis cause me relentless fatigue
People with MS are at a higher risk of having both types of sleep apnea
Written by |

I feel like I’ve written a lot of negative, maybe even depressing, columns lately. While multiple sclerosis (MS) can be a pretty negative and depressing subject, I’m normally a bit more upbeat. We’ve been having cold and gloomy weather lately, and I’d like to blame my low spirits on seasonal affective disorder (aka the winter blues), but that’s not it. I’ve just felt more fatigued than usual, and it’s showing in my mood.
Fatigue has probably been the most consistent part of my MS journey in the years since my diagnosis. But for the past six months, it feels like it has shifted into overdrive, plaguing my life daily. It’s come with all the usual symptoms like tiredness, brain fog, heavy limbs, and a depressed mood.
A number of factors may contribute to fatigue in MS, but one in particular caught my eye: poor sleep quality. I haven’t been getting the best sleep lately, and I think it has been affecting my waking hours.
A new diagnosis
A while back, I wrote about getting a full night’s sleep after having an intrathecal Lioresal (baclofen) pump implanted. That helped to get my spasticity (mostly) under control, which allowed me to sleep through the night for the first time in a while. I still experience some leg movement while I sleep, which could mean it’s time to adjust my Lioresal dosage.
In the past year, though, I’ve started waking up in the middle of the night again, often with an extremely dry mouth, which also is common when I wake up in the morning. My wife told me that while I only occasionally snore, I periodically stop breathing and then gasp and breathe heavily for almost a minute afterward.
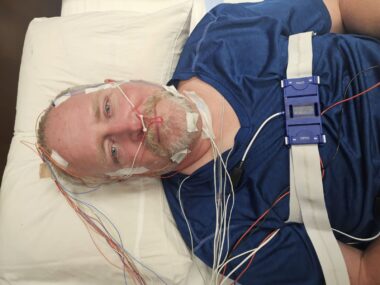
Ben Hofmeister settles in for his first sleep study. (Photo by Michala Hofmeister)
That’s when I started noticing my worsening fatigue and depressed mood. Others noticed it, too, so I decided to do three sleep studies, the last of which was last month.
Five or more apnea or hypopnea events an hour is the threshold for diagnosing sleep apnea. During the first sleep study, I had 44 such events. Those who administered the test assured me that I hadn’t come close to a record, but my number was far from ideal. I was diagnosed with both obstructive sleep apnea (OSA) and central sleep apnea (CSA), which also isn’t ideal.
OSA is exactly what it sounds like: Throat muscles relax and block the airway, restricting breathing. In CSA, brain signaling to muscles that control breathing doesn’t work, causing a person to stop breathing during sleep.
While it’s still poorly understood in people with multiple sclerosis, those with MS are at a higher risk of having both OSA and CSA, according to the Multiple Sclerosis Foundation. CSA in people with MS is thought to be linked to lesions that form in the brainstem, which controls the muscles that maintain an open airway during sleep.
Sleep studies aren’t much fun. I usually sleep on my back, so I didn’t mind that part, but the procedure involves a lot of wires and sensors. Add in a mask or nasal plugs for the positive airway pressure devices and sleep is — difficult.
A chin strap kept my jaw from sagging and made me look like someone with the mumps in an old photograph. This was my least favorite part but was necessary because, apparently, I’m a mouth breather. Yes, those exact words are in the study’s notes. I wasn’t offended because I was already aware of it, and besides, how else would you phrase it? My wife and I got a good laugh out of that one.
The first study diagnosed the problem and determined that the same airway pressure from a CPAP machine for both inhalation and exhalation wasn’t the solution. During the second and third studies, they tried different pressure settings using a BIPAP device, adjusting them to fit my breathing pattern.
The entire process has taken about five months, and there’s no guarantee it will be a perfect fix. If CSA continues to be a problem for me, we may have to try a machine that detects a halt in breathing and delivers a breath to get the cycle going again.
We’ll see how it goes. No matter what, I feel like it’s a step in the right direction. And that’s what a journey with MS is: lots of steps. Maybe I’ll sleep better after this step and feel less fatigued when it’s time to take the next one.
Note: Multiple Sclerosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Multiple Sclerosis News Today or its parent company, Bionews, and are intended to spark discussion about issues pertaining to multiple sclerosis.




Dr Elizabeth Swaffield
I too have extreme fatigue and MS. Sleep studies last year confirmed significant sleep apnoea episodes especially during REM. I'm female with a low BMI so not your typical person to have obstructive sleep apnoea. The sleep studies also confirmed high levels of leg spasticity/twitching throughout the entire night. I am awaiting a device fitting by the dental department as a first trial to help.
It was such a relief to read this article and realise I'm not alone in this situation!
Figgis
I am from the United kingdon. I was diagnosed with M.S around 15 years ago but they think I have had it for many years before judging by my medical records. I also have epilepsy, colitis, osteoarthritis, cluster migraines, severe restless leg syndrome. I take over 25 tables a day. My m.s in my opinion has got worse, the fatigue is so bad as my r.l.s causes me to have at least 2 nights a week where I will spend around 20 plus hours a night just walking up and down as I cannot sit down, in turn I do not sleep.
No one seems to take me seriously, no one does anything about it, no one seems concerned and no one not even my m..s. Consultant comments on it, no one seems to be interested at all.
I do not understand why, they wonder why my fatigue is so bad.
In my opinion in this country I do not think there is much help and I do not think the doctors listen to you or take your problems seriously. Do not know where to go from here. Feel let down and lost.
Claudia N Chamberlain
Five studies! I suspect my 23 year old son has apnea. The doctor is considering an at home sleep study with a machine that reports the results to the center electronically after training on how to apply it. Is this something you tried or are "at home" studies bogus?
Stephen Atkinson
My wife wakes me most nights saying I am dreaming of being with women and having sex. I just can’t convince her that I am not. It’s going to cause problems. I am getting very little sleep .( Something I need . ). I don’t thinking I am dreaming about anything but she says I am making crying and whimpering noises. A good thing in the morning she can’t remember a thing.
I am at my wit's end
Chris Jackson-Smith
Hi Ben, I too have OSA and had to chuckle at your description of the paraphernalia involved in a sleep study - not the most comfortable as I recall! As a result of that test I have a CPAP machine, my 2nd, that involves steam to alleviate the dry throat that the basic machine created. I have also tried all of the masks and eventually settled on nasal plugs. The only thing I haven't managed to resolve is preventing my cat from attacking the hose, I think he thinks it's a hissing snake trying to hurt me!!
My very best to you and your family x
Leigh Milford
Ben, I really enjoyed your article and the picture. I didn't know there were 2 types of apnea, so I found that very interesting. I'm going for a consultation with a sleep study specialist this week. My understanding is that I won't be hooked up and analyzed YET. I highly suspect that when they do wire me up, they will detect apnea of some kind, though it certainly would not necessarily be the chief culprit of any sleep disruption I experience nightly. I believe my biggest bullies robbing me of sleep are 1) spasticity in my legs 2) sopping wet "Depends" and bed pads and 3) kitties that love to sleep on my chest (good) or face (bad). I doubt that the 3rd factor will be allowed in the sleep lab and I love them too much to lock them out of my room, so I may be a stubborn, unsolvable problem.
Shirley Burneff
I have eight felines that share my twin bed. For some reason theyall choose to congregate on me at night, and leave my roommate alone. I thought purchasing some large , plush cat beds and placing them in the room would lure them to sleep in them, but to no avail. They prefer nesting all over me.
Shirley Burneff
I was diagnosed years before my MS diagnosis with sleep apnea. Been diagnosed with the MS for almost 2yrs, although I had many symptoms that plagued me before my formal diagnosis of MS. I , too, experience difficulty sleeping, tossing and turning due to leg spasticity. I have forsaken my CPAP machine, as I experience strange itching sensations and pain while wearing the apparatus. My daytime fatigue is horrible as a result. I take Adderall, 20 mg, tid for my ADHD, but it doesn't seem to help combat the lethargy. In fact, it often initially contributes to onset of sudden somnolence. Go figure.
Benjamin Hofmeister
Hi Shirley! I hope my BIPAP works for me (when it finally gets here). Daytime fatigue is the worst as you seem to know all too well. I hope we both find something that works for us.