The ‘Rare but Serious Side Effect’ that Could Have Killed My Sister
Written by |

Editor’s note: This is a guest column by Kristin Hardy, who was diagnosed with primary progressive multiple sclerosis in 2002. Her sister Margaret was diagnosed the same year with relapsing-remitting MS, complicated by trigeminal neuralgia. You are invited to follow Kristin’s blog at www.hackmyms.com.
***
It started out with mosquito bites — three of them — high up on my sister’s thigh.
At the time, we didn’t think much about it. It was a weird spot, but in New Hampshire, late-season mosquitoes are persistent little buggers. Margaret just scratched and bought a tube of After Bite at the pharmacy, where she’d gone to pick up antacids.
The next day, it was cream for a yeast infection. A day or two after that, she had a sore throat, then a rash, then a fever spiking so quickly that in the amount of time it took to shake down the thermometer from one reading to the next, her temperature rose half a degree. By then, we knew the red spots weren’t mosquito bites, they were hives. It would be another three days before we had an official diagnosis that tied together all of her symptoms: Stevens-Johnson syndrome (SJS), a skin and mucous-membrane disorder with a significant mortality rate.
Think of that line from the drug commercials that usually follows the rapid-fire listing of side effects: “Call your doctor immediately if [insert phrase here], as this may be a sign of a rare but serious side effect.” For therapies as varied as carbamazepine, Naprosyn, and even ibuprofen and acetaminophen, the U.S. Food and Drug Administration doesn’t mince words: The reaction is characterized as not just serious, but sometimes fatal. And its name is SJS.
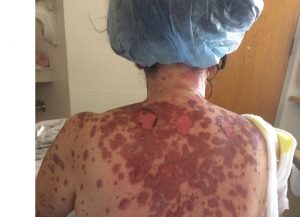
A “mild” case of Stevens-Johnson syndrome. The raw patches are where the skin has peeled away. Margaret has already begun to heal in this picture. (Courtesy of Kristin Hardy)
Want to learn more about the latest research in MS? Ask your questions in our research forum.
Stevens-Johnson syndrome is not a drug allergy. It is a chemical reaction that takes place in the cells of the skin and mucous membranes such as the mouth, ears, nose, eyes, lungs, G.I. tract, and genitals. Basically, exposure to some agent causes the immune system to go haywire and begin releasing signaling chemicals that trigger cell death. A red or purple rash springs up that forms blisters that burst and then peel. This is the danger with SJS: As the spots grow together, large swaths of skin can be stripped away, leaving the sufferer vulnerable to infection. SJS requires immediate hospitalization, frequently in the ICU or burn unit.
Treating SJS
In the case of my sister Margaret, who was visiting me, the expertise at my small-town hospital was just good enough to identify the syndrome. Fortunately, we live an hour away from Boston. We were able to get her transferred to Brigham and Women’s Hospital, a facility listed on the U.S. News & World Report Honor Roll of top U.S. hospitals.
No sooner had she been admitted than — like somebody in an Edward Jones commercial — she had people around her, including a dermatology team, an ophthalmology team, a gynecology team, and a general medicine team. They put tissue grafts in her eyes to protect her vision, as the eyelids are lined by mucous membranes and affected by SJS as well. They can form blisters that during the healing process can grow onto the cornea, leading to vision damage or even blindness. In Margaret’s case, the grafts prevented this issue.
In fact, she was pronounced by the doctors to have a mild case. Then again, it’s difficult to even think about using that word about a person who spends nearly a month in the hospital in agonizing pain while her body wars with itself.
For Margaret, the culprit appeared to be carbamazepine, a treatment her neurologist had recently prescribed for pain caused by her trigeminal neuralgia. For years, she has practiced self-hypnosis for pain control, resorting to medications only in her most agonizing moments. Now, that has been taken from her. She can’t ever take any medication from that family again.
Know the symptoms
You’re reading this story because we both feel that it is important to educate the MS community on SJS. It’s a very rare disorder, and you’re more likely to be struck by lightning than to contract it. For carbamazepine users, however, SJS is far more common. FDA labeling estimates that as many as six of every 10,000 new users will experience SJS. And carbamazepine is the go-to medication for treating trigeminal neuralgia.
None of this is to suggest that you quit or avoid taking carbamazepine. Just educate yourself. Speed of response has an enormous effect on prognosis. Talk to your doctor and make sure you know the symptoms. Be aware that the disorder can occur at any time, whether on your first dose of a new medication or your hundredth. And most of all, educate those around you so that if anyone begins to contract SJS, they get to a hospital as quickly as possible.
Over a year has passed since Margaret’s illness. While not entirely recovered, she is past the worst of it, and it appears she won’t have significant lasting effects. One thing is certain, though: We will never look at a simple mosquito bite the same way again.
***
Note: Multiple Sclerosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Multiple Sclerosis News Today or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to multiple sclerosis.
Danielle Stone
WOW! Thank you so much for writing and sharing your sister's horrible but courageous story. Not at all what I expected. But something we all need to be aware of. I personally am hypersensitive to most drugs prescribed in relation to my MS. Gabapentin for one, it gave me something similar to face shingles. Very painful. Copaxone I couldn't tolerate. The list goes on and on. Brio for some lung exhaling issues I developed last summer during the heat, caused 4 side effects that were intolerable. One was vision related and the other was easy bruising. Nothing like your sister, but I value my vision. That was unfortunate as the lung and breathing is still a problem. Anyway, thank you for sharing her story!
Kristin Hardy
Hi Danielle, thanks for writing (and reading). Yup, it was pretty scary but she came through it like a trouper. Just a reminder to all of us to read the packaging.Take care!
Theresa
Thank you for alerting all. Was so thoughtful of you as I never knew. Do hope you sister is on the up and up and you as well. And those yuchy mosquitos, living in the south it's like run and hide!
Kristin Hardy
Credit goes to my sister for being willing to share her story. As to mosquitoes in the South, I heard they're big enough to vote!
Carlos
One day I will have to write up the story of our son's fight with SJS. He actually contracted the "3rd degree burn" level of Stevens Johnson called TEN, Toxic Epidermal Necrolysis. This is when more than 30% of your body is covered with a rash that then blisters. He was above 40% and climbed higher. Mortality rate for such cases is over 30%.... so we are fortunate he is still with us. More people need to be made aware of this syndrome. Doctors are responsible for making sure patients know what to look for and what are the worst case scenarios.
Kristin Hardy
Hi Carlos, thanks for writing. What a terrifying experience to go through with your son. I'm so glad to hear that he made it through. I agree about the need for awareness. My sister's doctor didn't even mention the possibility of SJS. It ought to be required.Take care.
JoAnn
Thank you so much for sharing your story. Our son has MS as well (diagnosed at 21 and is 45 now). In January 2018 they change his MS meds from Copaxon to Galenia (daily pill). We thought this was going to help, but he got worse. Six months later he had a Grand Mal seizure (we can not prove if it was the new med or not). He was seizing for about 55 minutes. They had to put in a coma to get it under control.
While in the ICU he developed this horrible rash (which turned into big blisters with liquid)on his back. They brought in the dermatology department to look and treat this, but it took some time. The blisters would break and become more painful. He had his back checked several times a day, each time they check it it became more painful and they realized that changing his dressings was causing much more pain for him. It took a long time for this to clear up. This totally sounds like what your sister had. Sound familiar?
So I want to thank you for bringing this up in you blog. This is how we learn from each other.
My preaching word to our son is attitude! Attitude is 9/10s of a crappy diagnoses.
I hope you and your sister are on the up and up. Be the BEST that YOU can BE!!
Kristin Hardy
Hi JoAnn, I'm so sorry to hear about your son's ordeal. It's so scary when you don't know what's happening. It's even worse when the doctors don't know, either. Here's hoping the best for him going forward. Thanks for writing!
Cary Sue gray
I have two aumontie imume disase and keep getting persritpion for deppsion but alot of them can cause this I am scared to take them .what y'all think?
Penina
Just an FYI, anti-depressant Welbutrin (buproprion) is known to cause rash sometimes extending to SJS... How did I find this out? Three weeks into taking it, I currently have the rash for the last five days...tapering off the med as quickly as I safely can and keeping a close watch that the rash does not get worse. Feels like sunburn at times, itchy at others. Comes and goes, things pursuing against my skin can bring it on.
My dear daughter was hospitalized just short of SJS from Bactrim DS. That was scary.
Debbie Neufeld
SJS just took the life of my beautiful niece. She had taken some ibuprofen for the flu and within two days she had developed SJS which killed her liver. She fought a hard fight for almost six months but her body just got too weak to fight. We had never heard of SJS but it is very real and the scariest thing our family has had to deal with. People need to know about SJS. She had taken ibuprofen before and to be honest they don’t know exactly that it was the iboprofen, Tamiflu or zoysin that caused it. Our lives will never be the same but we are now on a mission to get the word out about SJS.
Shellee
My sister, very recently, was rushed to the hospital with SJS. She has MS and has been thru so much - We don't know the extent of the damage this has done to her. Thank you for the note on the eyes - I have let my sister's daughter know to have the hospital to protect them. Thank all of you for your comments.
Gerrund
How long did she take the medicine for before she noticed the symptoms?
Christine
Thank you so much for sharing your story with all of us.You will save many lives by sharing your story.I am an SJS survivor and would like to make others aware that SJS can present itself suddenly. I had taken different sulfa based medications and lotions for months and began to have what appeared to be hyperpigmentation on different areas of my body. After many months of feeling very ill and being photosensitive, I put a pin tip size of Benzaclins on my face where this hyperpigmentation was and immediately my entire face swelled up and turned charred black looking. When I put my face into water to bring down the intense heat I was experiencing, my entire outer skin sloughed off. For me, SJS was not blistering and bumps, it was complete sudden black necrosis from a combination of sulfa antibiotics and Benzaclins which I found out later contained sulfa, benzoyl, and clindomycin. It burns from the inside and burned my esophagus, eyes, nose, and face.
Please read up on the ingredients of everything you take.