Imaging That Captures Damage to Brain in CIS Helps in Determining Likelihood of MS, Study Says
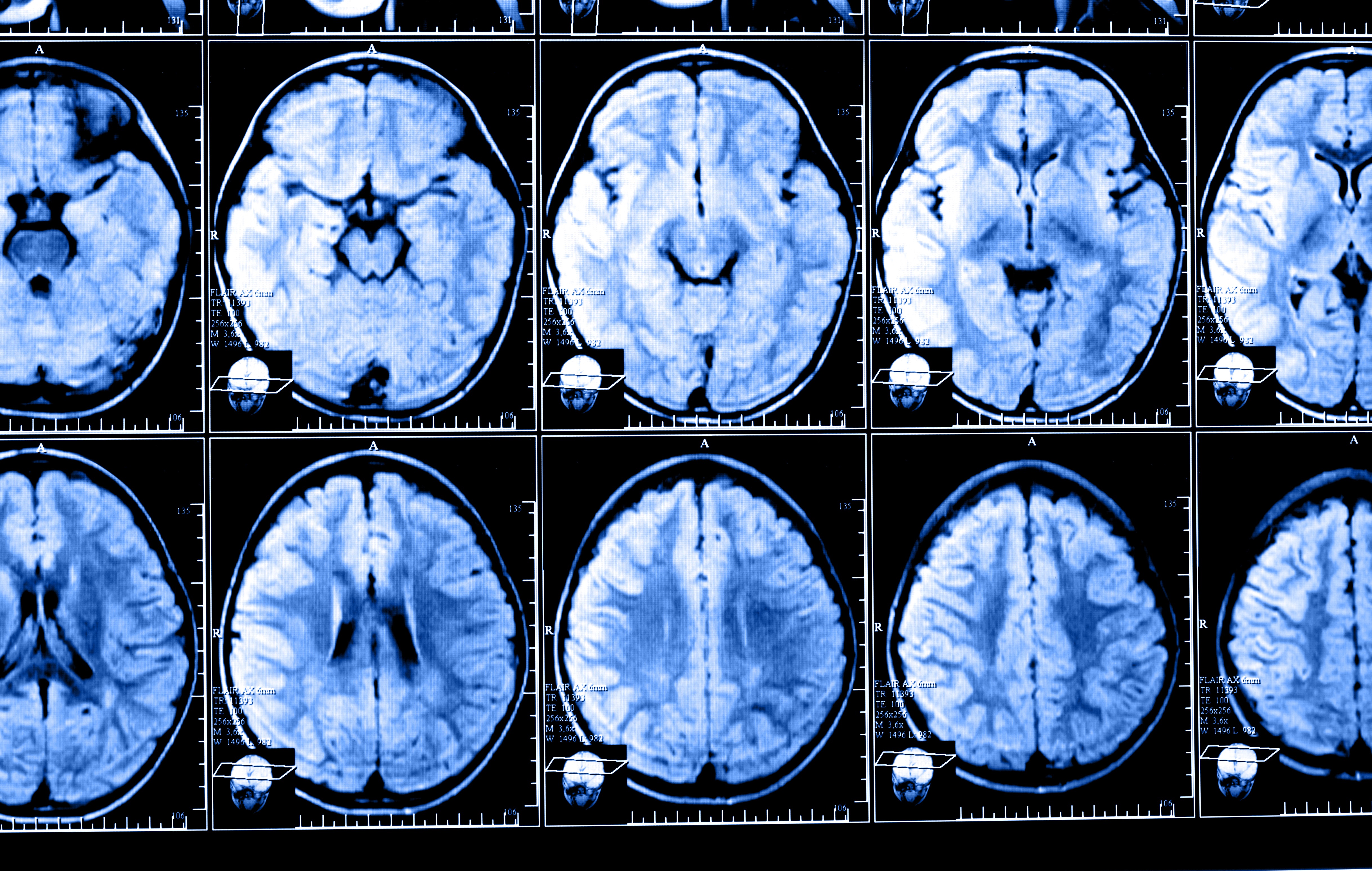
Imaging techniques that measure damage to the brain, in addition to those that detect lesions, may be useful in predicting likely disease progression in people with clinically isolated syndrome (CIS), a study found.
The study, “Early imaging predictors of longer term multiple sclerosis risk and severity in acute optic neuritis,” was published in the Multiple Sclerosis Journal – Experimental, Translational and Clinical.
Multiple sclerosis (MS) starts out as CIS, where there has only been one neurologic episode like optic neuritis, so it’s not “multiple” sclerosis yet. Many people with CIS will eventually progress to MS, but some won’t, and distinguishing between the two is a clinical challenge.
Brain imaging for MS usually involves magnetic resonance imaging (MRI) that is focused on looking for lesions, spots of active inflammation. But these may not tell the full story, as disease progression in MS is not just affected by lesions visible on a scan, but by widespread damage to brain cells (neurodegeneration).
To investigate predictors of long-term MS progression and severity in CIS patients, researchers in Australia recruited 36 people with CIS and imaged their brains at presentation (the lone neurologic event) and again one year later. A group of 23 people without CIS (control group) were also imaged to serve as controls.
The team assessed lesions through conventional MRIs, and through diffusion tensor imaging (DTI) and optical coherence tomography (OCT) — both of which can more directly measure neurodegeneration.
Participants were followed for a median of eight and a half years. Over the course of this time, 25 people progressed from CIS to MS, while the remaining 11 did not.
Compared to those who held stable, patients who progressed to MS had significantly more and larger lesions develop in the first year after presentation. They also had significantly lower DTI measurements in certain brain regions (specifically in the corpus callosum and cortico-spinal tract), and more thinning of the retinal nerve fiber layer (RNFL, which is what OCT actually measures; of note, RNFL thickness decreases over time, and it correlates with axonal damage in the visual pathways and whole brain atrophy).
In statistical models, the only factor that was significantly predictive of time to a second neurologic episode (relapse), once all factors were taken into account, was the number of new lesions that appeared in the first year. This result suggested that markers of inflammation (i.e., lesions) would have the most predictive power.
“The number of newly appearing lesion was the only significant predictor of rate of second relapse, demonstrating that clinical relapses are strongly associated with early MRI inflammatory activity. This confirms previous studies reporting that baseline lesion load is significantly greater in patients who develop MS,” the researchers wrote.
However, none of the variables assessed were significantly predictive of the number of relapses.
Researchers also found that a greater decrease in RNFL thickness in MS patients was significantly correlated with higher scores on the Expanded Disability Status Scale, which indicates more severe disability.
Taken together, the data suggested that incorporating new imaging techniques, not just measuring lesions, can provide valuable prognostic information for people with CIS, the team concluded.
“Novel prognostic algorithms that integrate standard radiological assessments of lesions, together with newer imaging assessments that are sensitive to neurodegenerative changes, could improve the prediction of longer term clinical outcomes in MS, and should be explored in larger cohorts to inform clinical practice,” the researchers wrote.