$7.2M NIH Grant Supports Study of MS Diagnostic Biomarker
Written by |
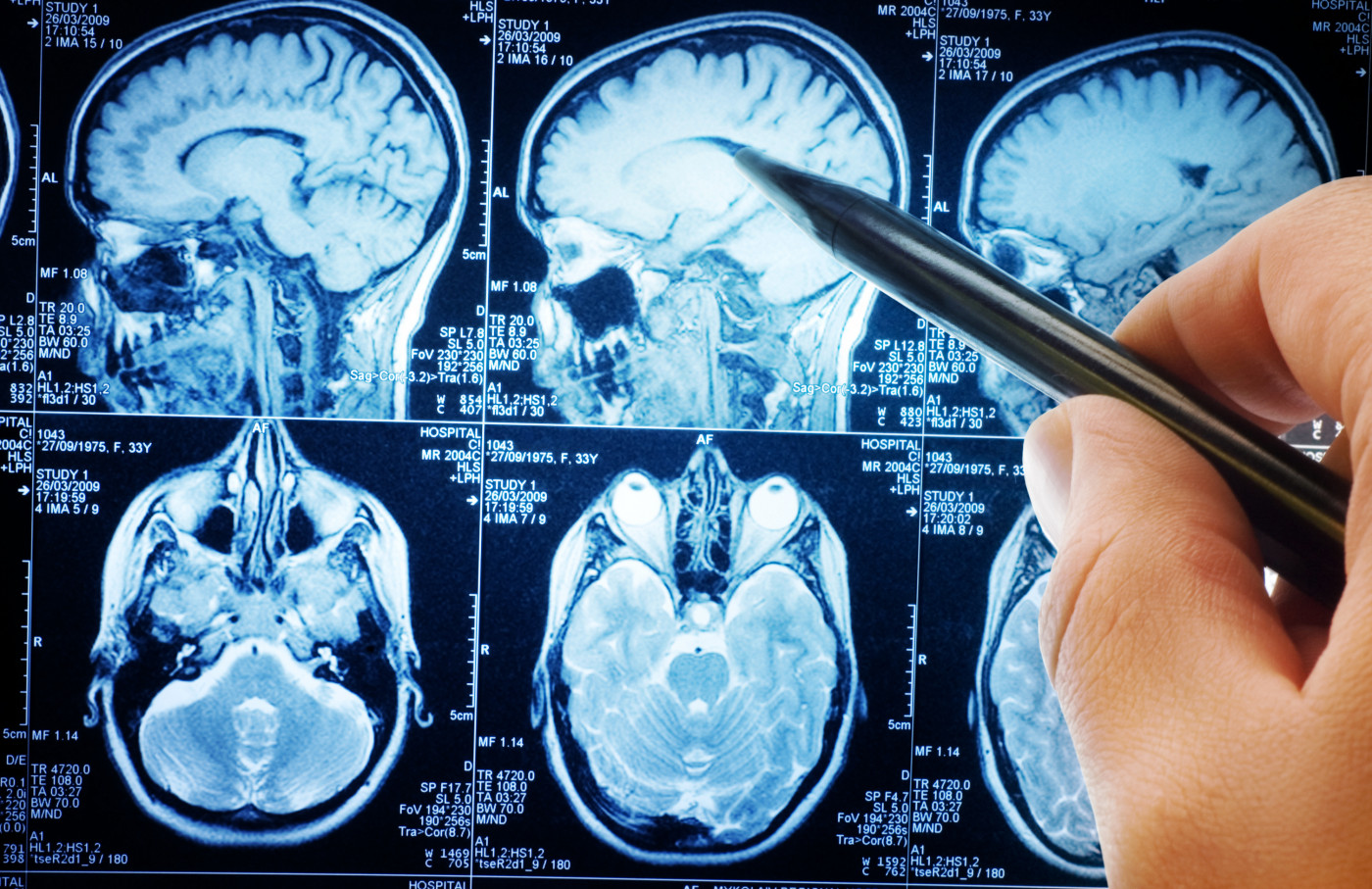
The National Institutes of Health (NIH) awarded a $7.2 million grant to a team led by Cleveland Clinic researchers that will study whether a new biomarker might more accurately diagnose multiple sclerosis (MS).
Grant money will support a study in 400 adults suspected of having MS to determine if the proposed biomarker, called the central vein sign (CVS), is a reliable diagnostic marker for this disease.
“Up to 20% of MS diagnoses turn out to be inaccurate. Our new multicenter study aims to reduce that number by evaluating if this new biomarker can improve diagnostic accuracy and simplify clinical decision-making,” Daniel Ontaneda, MD, PhD, with the Cleveland Clinic’s Mellen Center for Multiple Sclerosis, said in a news release.
The study, called CAVS-MS, will enroll people with evidence of typical and atypical MS symptom at 11 sites across North America, overseen and coordinated by the Cleveland Clinic. It will be led by Ontaneda and Nancy Sicotte, MD, with Cedars-Sinai, and conducted under the auspices of the North American Imaging in MS Cooperative.
The area surrounding the brain’s central vessels is thought to be where inflammation more likely occurs, leading to lesions that can be detected on MRI scans. CVS refers to the visualization of these veins inside brain lesions, which is thought to reflect the loss of myelin — a protective sheath of nerve cells — due to inflammation.
CVS has been proposed as a sensitive and specific biomarker, one able to help differentiate MS from other conditions with similar brain lesions captured on imaging, from meningitis to strokes, lupus to Alzheimer’s.
A recent study showed that detecting changes to the brain’s central vein captured through MRI is a useful and accurate way to improve MS diagnoses. In the study, an analysis of more than 4,000 brain lesions — collected from eight neuroimaging European centers — showed that capturing CVS changes enabled researchers to distinguish people with MS, including those with clinically isolated syndrome, from people without this disease but comparable brain lesions.
“We aim to show that the CVS is a simple and reliable diagnostic biomarker that can be immediately translated into clinical care,” Ontaneda said. “We are evaluating if this sign can improve sensitivity and specificity relative to current approaches and streamline the clinical decision-making process.”
No single test can diagnose MS, and MRI is currently the most non-invasive and sensitive way of imaging the brain and spinal cord. Still, diagnostic inaccuracies persist. According to Ontaneda, up to 1 in 5 people diagnosed with MS are later found not to have the disease.
MS diagnoses are also based on criteria — called the McDonald Criteria — that do not apply to the nearly half of all patients with atypical presentation.
The goal of the CAVS-MS study is to determine whether CVS can lead to earlier and more accurate MS diagnoses. Researchers will also assess the best and most cost-efficient ways to integrate CVS findings into MS diagnostic criteria.
“These initial exploratory analyses will be important to how readily positive findings about the utility of CVS criteria can impact clinical practice,” Ontaneda said.
Funding comes through the NIH’s National Institutes of Neurological Disorders and Stroke.



Leave a comment
Fill in the required fields to post. Your email address will not be published.