Number, Location, Size of Lesions on MRI Can Predict Progression to MS, Study Shows
Written by |
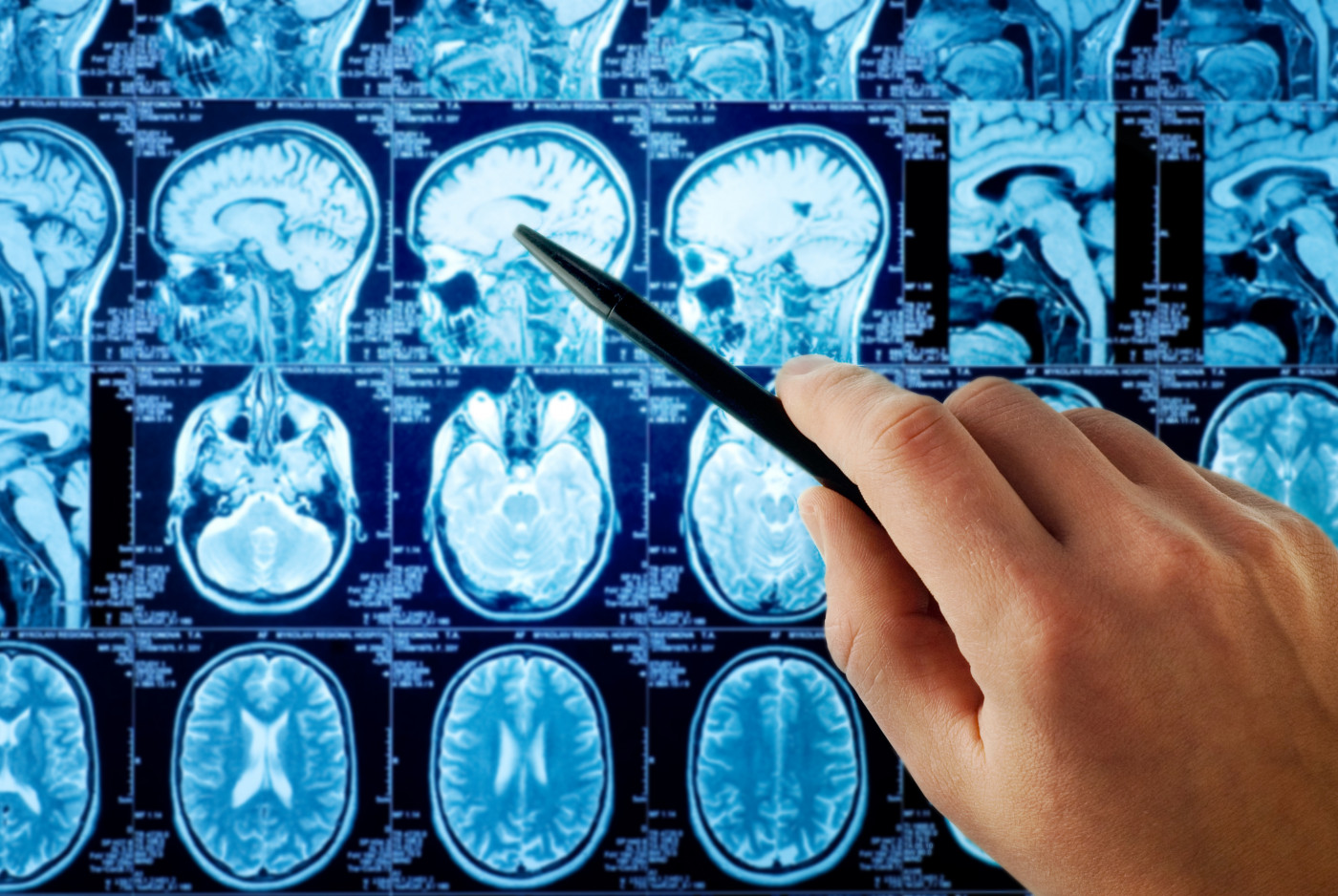
The number, location, and size of lesions can help predict the risk of progression from clinically isolated syndrome (CIS) to multiple sclerosis (MS) within one year, a new study shows.
The study, “MRI in predicting conversion to multiple sclerosis within 1 year,” was published in the journal Brain and Behavior.
Most patients diagnosed with MS initially present with CIS. In 50-70% of patients, magnetic resonance imaging (MRI) is taken at the time of CIS diagnosis, and it usually reveals multiple white matter brain lesions that suggest the presence of demyelination (or myelin loss, the process that underlies the pathology of MS).
Studies have shown that in about 30% of patients with an abnormal MRI scan, a second clinical attack, or a change in MRI occurs within one year, confirming the diagnosis of MS. But long-term studies have shown that up to 20% of patients do not have another clinical attack for at least 20 years.
This wide clinical spectrum puts physicians and patients in a situation of uncertainty at the time of disease presentation, as guidelines suggest that early treatment is the key to slowing the progression of MS.
So, researchers set out to identify the MRI characteristics of patients at first presentation that would predict either a second clinical episode or conversion to MS within the first year.
For this purpose, researchers assessed the medical records of 46 individuals who presented with an episode of CIS, and who were followed both clinically and through imaging for a year.
Ask questions and share your knowledge of MS in our forums.
A neuroradiologist, who did not have access to the clinical data, reviewed the MRI images from CIS patients and recorded the number, location, and the largest diameter of the lesions.
One year after the first MRI, 25 patients (54%) progressed to MS.
The cerebral cortex, the largest part of the human brain, is composed of four major lobes – temporal, occipital, parietal, and frontal – and each has its own individual roles.
The corpus callosum is the region of the brain that connects the two hemispheres. It is responsible for integrating motor, sensory, and cognitive signals between the two hemispheres of the cerebral cortex.
When looking at the location of lesions, CIS patients with lesions that were either in the temporal lobe, occipital lobe or perpendicular to the corpus callosum were more likely to have recurrence of a clinical episode.
Researchers also identified a specific combination of location, number, and size of lesions that would significantly increase chances of progressing to MS. According to the team, patients with a combination of more than 13 lesions, with a maximal lesion diameter greater than 0.75 cm, and lesions perpendicular to the corpus callosum, had a 19 times greater chance of progressing to MS during the following year.
“Assessment of the number of lesions, lesion location, and maximal lesion size can predict the risk to develop another clinical episode or a new lesion/new enhancement in MRI during the year after CIS,” the researchers concluded.
“For patients with a higher risk of recurrence, we recommend closer follow‐up,” they added.



Donna
I have had MS for 11 years meaning 11 MRI’s every year I’ve been told no changes in lesion size, or location Which is absolutely good news . My question is : Is this normal for no changes?
marwa elhanafy
Yes could be normal as long as you have given a deinitive diagnosis of MS before.
Tjis could be either : You are on DMT whock works well with you or you are of people of low activity MS.
Gina
I have a frontal lobe brain leision that measures 8.7cm. Is thus big?
rachele childers
I was told I have 75 lesions is this alot ??? they are in white matter of my brain non on my spine or neck. I have tremors when upset stressed or in a hurry. and I have balance issues ... i trip over my own feet.
M. M.
I'm in the same boat as you. I wish us both the best. 60-80 for me.
Lori wilcox
I had 22 leisons with one on the Pons in January, now I have 36 with 5 of them on the Pons in August, but so far, none in my spine. Still have no diagnosis. Feeling very frustrated.....
Renee O'brien
I have ms ..diagnosed in 2012 at the time I had 16 lessons on right side of my brain and 19 on the left side...now I have 39 total is that too many..knock on wood none on my spine
Jenn
My physician told me I have five lesions. I had zero in 2013. My mother has Primary Progressive and is quite ill. I should seek a second opinion, correct?