Newly Published NMSS Study Confirms Nearly 1 Million Americans Have MS
Written by |
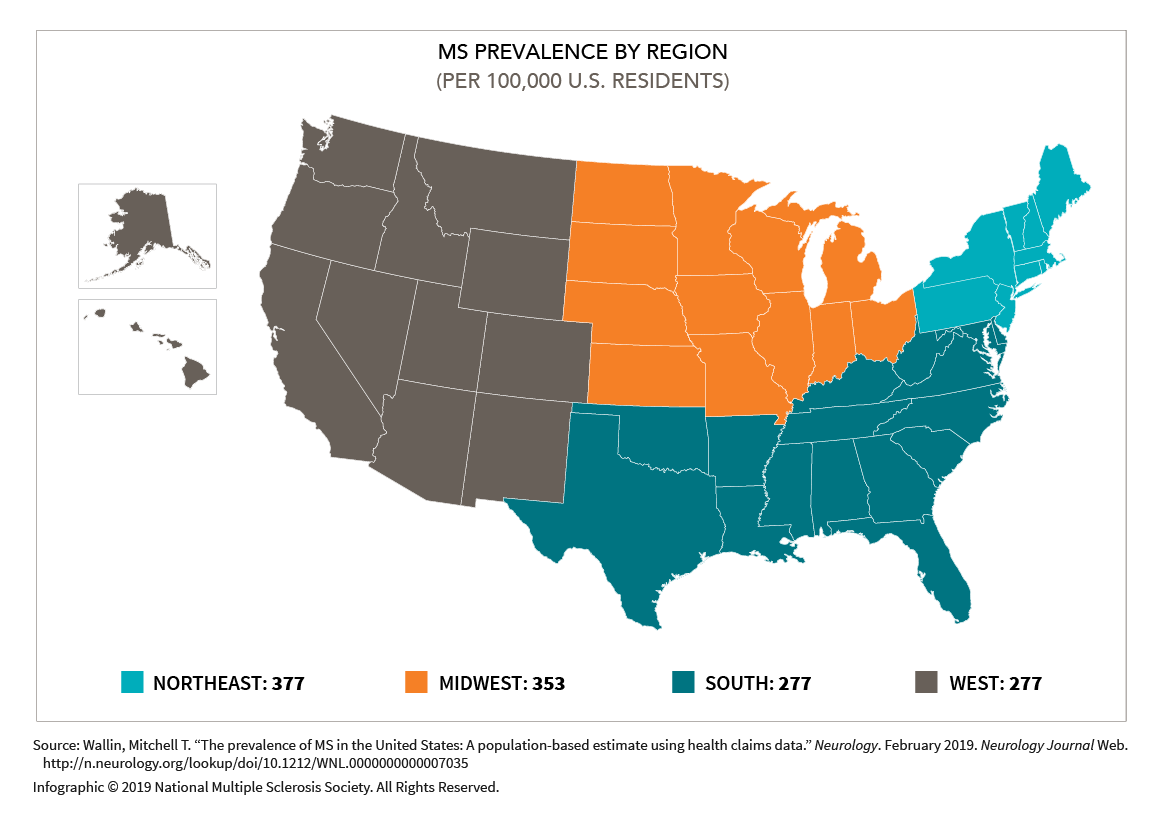
U.S. map shows MS prevalence in the Northeast is far higher than anywhere else in the country.
It’s finally official: Around 900,000 Americans and quite possibly more than that have multiple sclerosis (MS) — easily double the long-accepted figure of 400,000.
Since MS News Today first reported on this finding in November 2017, the National Multiple Sclerosis Society (NMSS) study, which reached that conclusion, has undergone a peer review process and has been accepted for publication in Neurology, the journal of the American Academy of Neurology (AAN).
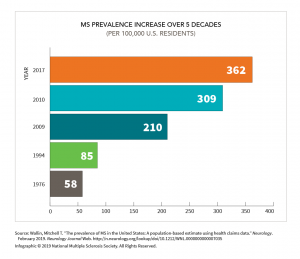
US study confirms that prevalence of MS has jumped six-fold since 1976. (Graphics courtesy of NMSS)
It appeared online Feb. 15 in the form of three articles: “Validation of an algorithm for identifying MS cases in administrative health claims datasets,” “The prevalence of MS in the United States: A population-based estimate using health claims data,” and “A new way to estimate neurologic disease prevalence in the United States: Illustrated with MS”. The print edition will be published March 5.
The $1 million NMSS study — nearly five years in the making — followed complaints that scientists had deeply underestimated the number of people living with the disease.
“After a lot of time hearing about how the original estimates were based on the best science at the time, our supporters felt we weren’t getting everyone,” Tim Coetzee, who heads advocacy, services, and research at the NMSS, said in a phone interview.
Join the MS forums: an online community especially for patients with MS.
“This study and the innovation behind it give us confidence that we now have a stronger representation of the number of people living with MS in the United States,” Coetzee said. “This gives us the ability to engage with policymakers, legislators, and companies about the impact MS has on people, and talk about the burden of the disease.”
Women now make up 74% of MS patients
Coetzee also said the unique approach pioneered by the 15 or so researchers involved in the study can be applied to other neurological diseases that don’t have national registries, such as Parkinson’s or Alzheimer’s.
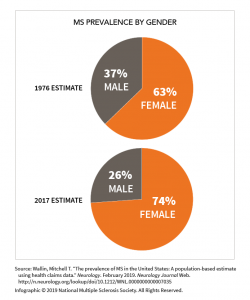
Women make up nearly three-fourths of all U.S. patients with MS. (Graphic courtesy of NMSS)
“This taught us we could use existing data from government and private insurance companies to be able to get to an estimate fairly modestly,” he said. “The algorithms can be adapted. You’d need to tweak it for that particular disease, but it can be done.”
The study drew on data from five national databases — Optum, Truven Health Market Scan, Department of Veterans Affairs, Medicare, and Medicaid — and one regional database, Kaiser Permanente of Southern California. Collectively, these six databases provided information on well over a third of the U.S. population, with the rationale that “nearly all persons with MS, except the uninsured, would be captured in one of these programs.”
“What this means is that we have to work harder, because there’s more of a need than we had realized,” said Nick LaRocca, vice-president of healthcare, delivery and policy research for the NMSS, which is headquartered in Hackensack, New Jersey. “For people living with MS, it means we have a larger constituency, and that we have clarified something important about the nature of MS as a medical condition.”
That constituency numbers anywhere from 851,749 to 913,925 people, according to the study, which extrapolated 2010 data out to 2017. The study — which excluded children, prisoners, and undocumented immigrants — does not break down the prevalence of specific types of MS, such as relapsing-remitting multiple sclerosis (RRMS) or primary-progressive multiple sclerosis (PPMS).
But it does reach some notable conclusions. MS now affects 362 of every 100,000 inhabitants, up from 309 per 100,000 in 2010, 85 per 100,000 in 1994, and 58 per 100,000 in 1976. And 74% of today’s MS patients are women, up from 63% in 1976.
“I don’t know if that means women are being diagnosed more quickly than men,” said LaRocca, who has headed the MS Prevalence Initiative since its 2014 launch. “It could be that now that we’re counting more accurately, we’re able to get a better estimate.”
Geography a big factor in MS prevalence
There’s also a correlation with MS prevalence and distance from the Equator. People living in the nine U.S. states comprising the Northeast — Connecticut, Maine, Massachusetts, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, and Vermont — had a prevalence of 377 per 100,000 inhabitants, while those in the South and West each had prevalence rates of 277 per 100,000.
U.S. map shows MS prevalence in the Northeast is far higher than anywhere else in the country.
The NMSS study does not attempt to calculate disease prevalence on a state-by-state basis, though it cites an earlier set of studies conducted between 1985 and 2011 that showed the nation’s lowest MS prevalence in a 19-county region surrounding Lubbock, Texas (39.9 per 100,000) and its highest MS prevalence in Olmstead County, Minnesota (191.2 per 100,000).
Among all age, gender, and regional groupings surveyed by NMSS, the highest prevalence of all was found among women 45 to 54 years old in the Northeast (762.3 per 100,000), while the lowest was among men 18 to 24 in the South (19.2 per 100,000).
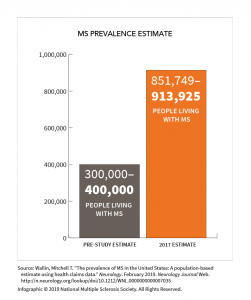
More than twice as many Americans now have MS than previously believed, a new study shows.
“There are a couple of reasons for this geographic variation,” LaRocca said. “One theory is that MS is related to exposure to ultraviolet radiation, also known as sunlight, which — in conjunction with the human body — has the effect of producing vitamin D, which seems somewhat protective. So people exposed to less sunlight, especially in their early years, tend to be at greater risk.”
In fact, Canada has historically had the world’s highest prevalence of MS, with high rates also in northern Europe — particularly Scandinavian countries — while the disease is practically unheard of in the tropical regions of Africa and South America.
LaRocca said: “Migration studies have shown that people who migrated very early from an area of higher risk to an area of lower risk will retain the risk of the area they came from. And Australian studies have shown that the amount of variance in MS risk is not associated with vitamin D but something else instead. It’s possible that ultraviolet radiation may have a direct impact on the immune system.”



Brian Baldwin
If you want to see where MS is really concentrated you should expand the map to show Canada and the fact that Manitoba is MS Central.
Saloua
Very intresting
There is a published article of this data ?
Jack
You’ll see the links to the three studies in the third paragraph of the article, to the right of the graph (on my screen, anyway). They are the highlighted titles.
Laurie Tossava
ethnic origin is not the only likely predictor. Another recent article pointed out the relationship of the gut and the likelihood that if a person has MS they were likely on antibiotics as a young child.
Jenny Bookwalter
I agree with this theory, I was outside from morning till night as a kid. Always had a tan I didn't prep for! But I had earaches and sinusitis, and was on antibiotics non stop. By 10 I had a stomach ulcer.
Christopher
This is a horrible statistic. Especially since there's a dearth of knowledge about MS, a brutally unfair stigma that accompanies it, and the lack of adequate assistance and resources for everyone completely sucks!
The truth is cruel.
ALAN S
Maybe it was a conspiracy theory, but I had always been told that the number of MS sufferers was kept low so that the drugs could be manufactured under an orphan drug statute which gave the pharmaceutical companies a more favorable tax structure and therefore allowed for more medicines to be created.
Laura Brown
Actually I remember reading somewhere that the numbers in the orphan drug statute were come up with making sure MS qualified at that point in time.
Many doctors would not even diagnose MS due to the negative effect it had on employment and insurance once diagnosed.
Christina Wilson
Even more reason to look at community support for housing people with MS and need for assisted living centers as aging occurs. These numbers demonstrate rising need, especially for single women without family resources. Please help as aging and MS does not necessarily get less demanding.
Catherine
Another study should be performed to see what the number of children is and where.
Linda
Sadly as a nurse that’s no longer working due to MS these findings don’t surprise me. I still believe the number is higher due to uninsured people and so many undiagnosed or diagnosed wrongly.
Kevin Keplinger
I don't believe this for a second. The NMSS had been using that old 400,000 figure so long that everyone knew that it couldn't possibly be true. They just got tired of people like those of us in the HSCT community criticizing them about it so they just came up with this new nice figure of 1 million. How convenient!!!!