A Friend Under the Skin: My Intrathecal Baclofen Pump
The muscle relaxant helps relieve my spasticity and other MS symptoms
Written by |

In my last column, I mentioned that I had an intrathecal baclofen pump. I’d make a bad pun, but I don’t have it in me.
Spasticity, spasms, and hyperreflexivity were some of my first symptoms, which steadily got worse as my multiple sclerosis (MS) progressed. I was prescribed oral baclofen (a muscle relaxant often known by the brand name Lioresal), but I was sensitive to it and could only tolerate about 40 mg a day. At that dose, it barely touched my spasticity while leaving me slumped in my recliner, weak and half asleep, unable to think clearly.
Unfortunately, that dose wasn’t enough to prevent the occasional spasm from arching my back and extending my arms and legs straight out, sending me sliding out of the recliner like a burial at sea.
I tried to ignore it and let the spasticity go on until I became dependent on the rigidity to function. A stiff torso held me upright, and I made a habit of levering myself up on unbending legs to totter and turn like a circus performer on stilts. This was also the time of my worst bladder and bowel incontinence, which I blame on an almost constantly clenched abdomen.
Sleep was inconsistent at best. I desperately needed it since the almost constant stiffness exhausted me, but it turns out that rigid immobility isn’t conducive to a restful night. That, combined with a puff of cool air or the sheet touching me the wrong way and setting off a spasm, meant that a four-hour stretch of dreamless sleep was about as much as I could manage.
Something had to give.
After discussing it with my neurologist, I had a test dose of intrathecal baclofen administered via lumbar puncture. The test produced positive results, and several months later, I had the pump implanted under the skin of my abdomen, on the right side, just above the waist. From there, a thin catheter goes around to my lower back and inserts into the lumbar region of my spinal column, where it’s threaded up to the T10 vertebra.
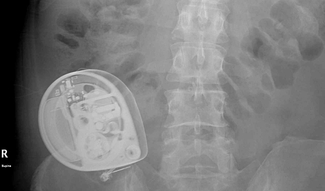
An X-ray confirms the placement of Benjamin’s baclofen pump. (Courtesy of Benjamin Hofmeister)
It turns out I’m sensitive to the intrathecal version of baclofen, too, and an initial dosing hiccup turned my one-night stay in the hospital into four. After being rigid for so long, I went limp from about the bottom of my rib cage down and spent nearly a month in bed before I rebuilt the strength to even sit up without being completely dependent on my wife. This passive immobility sounds terrible, and I suppose it would’ve been if it weren’t for the blissful relaxation and the ability to sleep through the night, deeply enough to dream again.
Because of the catheter’s placement, my arms and hands are unaffected. There are a number of issues with a higher placement on the spine, making it the rare exception rather than the rule. Fortunately, those arm and hand muscles are much smaller than the muscles of my legs and abdomen and were less spastic to begin with.
Bladder and bowel incontinence continued, this time because of a relaxed torso rather than a rigid one. Fortunately, this has improved with strength-building therapy in a way it never did when it was clenched nearly all the time.
My intrathecal dose is a tiny fraction of the oral one. This means I get all the good effects without any of the bad. I’ll have had the pump for two years in September, and we’ve worked our way up to 73.4 mcg a day, nowhere near the level others with a pump are at. Dosing is regularly adjusted with a tablet-type device and its attached probe. The idea is to tailor it so that the spasticity is controlled well while my muscles still have enough tone to be useful.
The pump has to be refilled at regular intervals. It might look gruesome, but the pump is right under the skin, and the needle just breaks it before clicking into the port. It’s in me, but it’s not really “in me.” Feeling it “click” in can be unnerving, too. It’s such a distinct feeling to me that it’s still surprising that no one in the room can hear it.
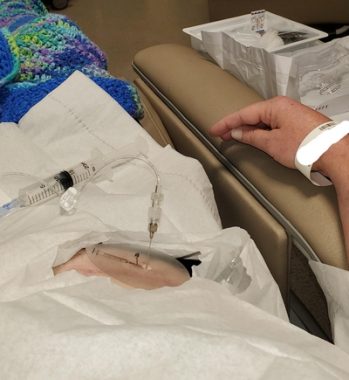
The refilling of Benjamin’s baclofen pump. (Courtesy of Benjamin Hofmeister)
The pump’s battery lasts for about six years, at which point the entire pump has to be replaced. The catheter remains, so getting the replacement is much less involved than the original surgery. Still, it’s a lifetime commitment to regular replacements, and no surgery is without risk.
This should not be considered lightly — especially, in my opinion, if one’s spasticity can be controlled through less invasive means. Spasticity was my biggest, most uncontrolled symptom. This was the right choice for me, but not one made without careful consideration by myself and my neurologist.
Ask anything you want in the comments, and I’ll do my best to answer.
Note: Multiple Sclerosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Multiple Sclerosis News Today or its parent company, Bionews, and are intended to spark discussion about issues pertaining to multiple sclerosis.
Mark Forrette
Hi Benjamin, nice write up about the baclofen pump and like you I have PPMS diagnosed in 2010 and I am completely wheelchair dependent. Prior to my pump placement, I met another guy with MS who asked me if I had a baclofen pump and of course I said no. He then commented “I’m sure you’ll get one soon” and of course I didn’t know what that meant. After experiencing severe spasms, I finally had the pump placed over five years ago. I also experienced the initial spaghetti noodle phenomena requiring another hospitalization and steroids. Once my body got used to the pump it has worked beautifully with incremental increases in dosing. I had the pump replaced in January 2022 and it was a very easy procedure. To anybody who is struggling with spasm and oral baclofen I would highly recommend looking into an intrathecal baclofen pump.
Benjamin Hofmeister
Thanks for the comment Mark!
It was absolutely the right option for me and I would recommend it to anyone if they can't control their spasticity with less invasive means, (oral baclofen, or another muscle relaxer and therapy). I'm thrilled to know that replacement is just an outpatient procedure. The initial placement was less than fun.
Ben
David Claytor
Ben: Thanks for your article. My experience is very similar to yours…general relaxation, blessed sleep, clear-headedness, and the ability to focus and concentrate. ITB really gave my life back to me. True, there are trade-offs like reliance upon a power wheelchair, but that, too, has saved me tons of energy and it is so much safer just getting around. FYI, I just had my third replacement pump installed a couple of weeks ago. All it required was a ten minute operation under sedation, and I was home in time for lunch!
Benjamin Hofmeister
Thanks David! I would love it if this wasn't the right answer for me, but it absolutely was. Like you said, the trade off is being able to be involved in my own life, so it's absolutely worth it.
Have you ever set the alarm(s) off? I stayed too close to the MRI suite between scans and set off the critical 2 tone alarm when it stayed off too long (it was still detecting the magnetic field). Everything was fine, but everyone on an elevator stared at me once they identified the source of the noise and I had to look at everyone and confess that, yes, that alarm is coming from me and no , I'm not going to explode.
Ben
Kate Frazier
About how large is the pump itself? My Physiatrist described it as the size of a hockey puck, which sounds huge to me.
Benjamin Hofmeister
Hi Kate!
Hockey puck size seems to be the standard answer, but it's really about 1/4" thinner and nearly 1/2" wider. If an Oreo cookie was twice its own size (diameter and thickness) that would be about right. Maybe not a great example, but I have a lot more experience with Oreo cookies than hockey pucks.
It could be smaller if it didn't have a 40ml reservoir, but that would mean more refills. I don't mind the doubled oreo sized lump in my abdomen, but there's a scar that has to be freshened every 6 or so years to consider too.
Ben
Kathy Walter
I've had my pump for 17 years! Couldn't live without it!!!
Benjamin Hofmeister
Thank you Kathy! I'm almost at 2 years and am already grateful for the relief it provides.
Ben
Karen Smith
I’ve had my pump for 11 years and had the pump replaced once. I still am able to drive and go to various exercise classes.
My balance is terrible and I’m totally dependent on using a rollator to walk. Wish there was a medicine for balance problems that could be added to the Baclofen in my pump. I can’t imagine how my life with MS would be without the pump.
Benjamin Hofmeister
Thanks Karen! It's definetly a life changer. I often wonder if I hadn't put it off for so long, if I'd have retained more ability. I can stand with support and am working with therapy to take a step or two, but time will tell.
I don't have an answer to balance or fatigue. Please let me know when you do. lol
Ben
Gardenlady
Thanks for writing about this. I’ve wondered how it worked , it’s placement , and it’s effectiveness in reducing spasticity. I too suffer from this problem and currently take Baclafan. It’s putting a damper on the stiffness but it’s good to know there is something else that may be helpful.
Benjamin Hofmeister
Thank you for commenting Gardenlady. It's a big decision and a lifelong commitment, but it is an option when lesser means fail to get spasticity under control.
Ben
Marilyn Assenheim
Dear Mr. Hofmeister,
This is not a question OI would ordinarily ask but, would you please tell me how old you are? I am 70 years old and am waffling between Secondary and Primary MS. I had begun having your Baclofen-treated symptoms (not nearly as severe) about a year ago. I am currently on a 20 mg. oral dose of Baclofen and I was quite alarmed, based on your experience, to see just how severe these symptoms can get.
Thank you for sharing your experience and being open to questions. And thank you, sir, for your service!
Best regards,
Marilyn
Ed Tobias
Hi Marilyn,
I hope you won't mind my jumping in with an answer to your question, sort of. I'm doing because I'll be 74 next month and have lived with MS for over 40 years. I have very spastic legs. I'm not in a chair but I have used 2 canes or a scooter to get around for the past 15 years, or so. I use an extremely low dose of Baclofen, only 10 mg once a day before bed. It helps a little bit to calm my restless legs. I don't use it during the day because it slows me down too much. I find that physical therapy is much more useful.
Ed (The MS Wire column)
Benjamin Hofmeister
Thanks for the comment Marilyn and thanks for jumping in Ed. If you reverse Ed's age you get my age of 47. (Not rubbing it in, Ed. You are much more spry). Many, many people do very well on oral baclofen. Some of us are just sensitive and my experiences with spasticity are not the norm. The pump was the right choice for me but I would never have considered it if my spasticity could have been controlled any other way.
Ben
Cathy Mollohan
I am allergic to Baclofin, I get very nauseous and can’t function. I had a trial with the Baclofin injected directyinto my spine to see how it worked, well I was completely paralyzed from the waist down and was in the hospital overnight until it wore off. The Dr said I had all of the bad effects and none of the good ones. I have stiffness and can’t bend my legs and have to slide across the car seat to get my legs in. I noticed you said you are completely wheelchair bound, is that because the stiffness was the only thing keeping you standing and did the Baclofin make you too week to stand or were you already chair bound? I’m wondering if the trials dose I had was too strong or if I just can’t take it. ?
Benjamin Hofmeister
Thanks for reading and commenting Cathy.
I was already using a wheelchair before the baclofen pump, but would often have to secure my legs if they were spasming, or staightened. I could stand with support, but it was just the stiffness in my legs and torso holding me upright.
Even with intrathecal baclofen, I had to be at a very low dose and drug concentration. I had to work my way up to 50 mcg per day and after almost 2 years am just now at 73.4 mcg per day. Many people take a much higher dose, but like you, I am very sensitive to it. Then again, the 25mg of benadryl (diphenhydramine) they give me before an Ocrevus infusion still puts me to sleep .
Ben
Anneliesa Gaunt
Wow! This is the first time I've gotten to read stories from people with an intrathecal Baclofen pump. I've had M.S. for about 25 years and got my first pump in 2016 and was in the hospital for 9 days. Months of getting strength back but never back to pre pump. Then had it replaced in 2020 due to a problem with the catheter kinking 3x and having no clue why the Dr. kept having to increase the dosage . Always ask questions and trust your body when it tells you something is wrong.
With the second one I was home in under 10 hours and am on more than 50 % less than the first one. I have the 20 ml. pump and can't imagine the 40 ml. one on my 5' 4" frame. As it is now I live in drawstring pants or loose legged yoga pants. I use a rollator inside or wheelchair when out in public. Oh , i'm 53 years old.
I'm on Ocrevus IV every 6 months and take Ampyra twice a day .
Benjamin Hofmeister
Hi Anneliesa! We take all the same meds. I don't walk, but I've stuck with the Ampyra for the cognitive and dexterity benefits. I wasn't given the option of a 20ml pump, which is ironic because I'm on such a low dose that we only refill my 40ml pump with 20ml. I'd like to get a zipper, etc tattooed over the scar, but since it's going to be reopened every so often, it would just get messed up.
Thanks for reading.
Ben
Karen Daniels
Can you swim in a pool with the pump? Does it preclude you from getting MRIs?
Benjamin Hofmeister
Hi Karen! Yes and no. The pump, catheter, etc, is all inside me like an additional (man-made) organ, so swimming is no problem.
The pump was made MRI safe. It's non-magnetic and turns itself off when it detects the magnetic field. It turns back on when you’re clear of the field, but it’s standard procedure to have a rep check it after to make sure. I've had 4 MRIs with mine with no issues other than making the techs nervous.
"Now be sure to tell us if you feel it move, ok?)
"Thanks, but really, if this hockey puck sized object starts trying to escape from me, I wasn’t planning on keeping it to myself."
Ben
Michael Samson
Hi I’m a quadriplegic with little movement to my arms. I’ve been on baclofen orally for a little longer than five years. I find that my spasms are just getting worse my neurologist has just recently recommended it to me. I’ve been unsure about it because I’m only 40 and hopefully have a lot more life in me. Thank you for your post and anything you think would better help me.
Benjamin Hofmeister
I would normally say to try every other means to control the spasticity before considering the pump, but if your neurologist is recommending it, then I'll assume you have. It is not a treatment for MS, just one of the symptoms. In my case, the worst symptom. My spasms were getting painful and even dangerous. I remember being so blissfully relaxed after that I told myself that even if my strength never improved, (it did), not being rigid and being able to sleep through the night was worth it.
That said, it is a lifetime commitment to refills and replacement surgeries. It was the right choice for me.
Ben
Allie
Thanks for the article. I've been considering the pump. My neurologist had mentioned it many times when I talk of spasticity. I've been dismissing it because it SOUNDS so extreme and invasive. But my spasticity isn't going to go away and I'm losing more and more mobility to it as my body is forgetting things it was once able to do. Your comment about how you wonder what mobility you could have kept if you'd gotten it earlier really resounded with me.
I'm going to talk to my neurologist about it this Thursday. Do you have any recommended questions that I should be sure to ask?
Thanks
Benjamin Hofmeister
Hi Allie, it is extreme and invasive, not to mention a lifelong commitment to refills and replacements.
That said, it was the right choice for me since my spasticity couldn't be controlled with oral baclofen and was really interfering with my life.
I'd talk to my Dr about dosing. I was very sensitive to oral baclofen and took a very small dose. Turns out, i was just as sensitive to the intrathecal baclifen too. Initially my pump was set at 100mcg and was way too high.
Ben
Susan Youngbuck
Hi Ben - Thank you for telling your story. I am scheduled for the epidural trial in two weeks and I’m getting more and more nervous as it approaches! So I’m reading every possible thing I can find about Baclofen pump surgery, pros and cons.
I am 60 years old living with MS since 27. Spasticity started about 7 years ago and has gotten so bad that I’m now considering this pump. As with you, all other options failed. I couldn’t even do physical therapy and stretching because of the stiffness!
And I have fallen off the toilet like you fell out of the wheelchair when my legs decided to stiffen and shoot straight out! I now have bars installed so that doesn’t happen again, and i laugh about it now.
I’m glad you explained the overdosing as that is one of my biggest fears - becoming paralyzed! I’ll be sure to discuss this with my doc. You mentioned your incontinence was at its worst before the pump. Did that improve after? I can’t sleep more than two or sometimes three hours at a time because my spastic bladder wakes me up to go, again!
Thank you SO much for this information. It really is invaluable when making this difficult lifelong decision. I’m hoping it turns out to be the best thing for me also!
Best regards, Susan
Benjamin Hofmeister
Hi Susan. Don't expect anything too dramatic from the spinal tap/ test dose. I think I did and was a little disappointed after, but all the test is for is to see if the intrathecal Baclofen affects your muscle tone. For me, it was such a little effect that I thought they were going to tell me that I wasn't a good candidate for a pump, but I was very wrong.
The actual surgery usually keeps people in the hospital for one night, but mine turned into four because they started the pump at 100 micrograms which I'm just now up to nearly 5 years later. Apparently I was as sensitive to the intrathecal dose as I was to oral.
About the bowel and bladder effects....If memory serves me, I don't think Baclofen as any effect on bladder or bowel spasticity, but not having a clinched up abdomen sure helps. I still have issues with urgency, but my accidents are few and far between. I used to take a medication specifically for bladder spasticity, but after the pump I didn't have to. Is that because I'm more tuned in to my bladder, or because my muscles in my stomach aren't squeezing it so much? I'm not sure but I'll take the results regardless.
I still have some sleep issues, but mine are due to sleep apnea. For the most part I don't get woken up by spasticity and if my legs seem to be jerking more at bedtime, or when waking up, that is usually my clue to have the pumps rate turned up.
You can have the pump set to increase the dose at night and return to normal in the morning, but I haven't done that yet. I think I made my neurologist nervous with the initial dosing problem and he doesn't want to experiment with fluctuating doses.
I don't know that I answered all your questions. Feel free to contact me at [email protected]