#ECTRIMS2021 – Spinal Cord Lesions Predictive of SPMS Conversion in CIS
Written by |
Editor’s note: The Multiple Sclerosis News Today team is providing in-depth coverage of the virtual 37th Congress of the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS), Oct. 13–15. Go here to see the latest stories from the conference.
Lesions in the cervical spinal cord (neck region) at the time of a clinically isolated syndrome (CIS) diagnosis can significantly predict future progression to secondary progressive MS (SPMS), a study shows.
Notably, brain lesions were not as strong predictors of disease progression as those of the cervical spinal cord.
The findings add to prior studies reporting a link between more spinal cord lesions and a higher risk of SPMS conversion, supporting the predictive value of these lesions at CIS diagnosis.
This may help identify patients at higher risk of progression and improve treatment decisions.
The data were shared by Laura Lacruz Ballester, PhD, with the La Fe Health Research Institute, in Spain, at the 37th Congress of the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS), held virtually Oct. 13–15.
The oral presentation was titled “Cervical spinal cord T2 lesions independently predict early conversion to secondary progressive multiple sclerosis: a longitudinal 10-year study.”
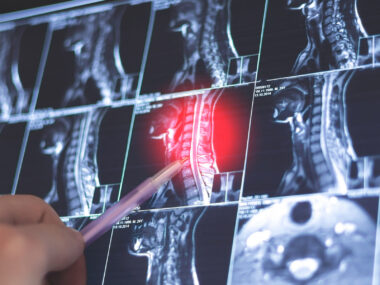
CIS, a neurologic episode that lasts at least 24 hours, often is the first clinical presentation of multiple sclerosis (MS). Magnetic resonance imaging (MRI) is used routinely to diagnose and monitor the progression of CIS and MS by looking for evidence of inflammation and lesions in the central nervous system (CNS, the brain and spinal cord).
In MRI, a T1 image offers information about current disease activity by highlighting areas of active inflammation, while T2 images provide information about disease burden or lesion load — essentially the total amount of lesion area, both old and new.
Several studies have focused on the identification of predictive markers of disease progression and conversion in CIS patients. The number of T2 lesions in the brain has been studied as a predictor of SPMS, but whether T2 lesions in the cervical spinal cord can predict CIS-to-SPMS conversion remains unknown.
To address this, Lacruz-Ballester and colleagues in Spain retrospectively analyzed MRI and clinical data from 242 CIS patients followed at six Spanish hospitals for at least eight years.
Patients’ mean age was 32.3 years, 71.1% were women, and they were followed for a mean of 12.7 years.
All had a brain and cervical spinal cord MRI at diagnosis, were treated according to clinical practice guidelines, and were assessed every three to six months and whenever they experienced a disease relapse.
Two independent neurologists and one neuroradiologist evaluated the participants’ MRIs.
Results showed that 205 patients (85.6%) received treatment, including 87 (42.4%) who started treatment after their first relapse — meaning their treatment started right after the diagnosis of CIS.
Most CIS patients (92.6%) experienced a second relapse, meeting the criteria for clinically definite MS, and 36 of them (14.9%) progressed further to SPMS.
There were no significant differences between patients who converted to SPMS (converters) and those who remained with CIS or relapsing-remitting MS (non-converters) in terms of demographic characteristics and disease duration. The proportion of patients who received treatment at CIS also was similar among both groups.
At CIS presentation, myelitis (spinal cord inflammation) was more common among converters (48.4% vs. 37.9%), while optic neuritis (inflammatory damage to the optic nerve) was more frequent in non-converters (19.7% vs. 6.5%).
Notably, both the presence and number of cervical spinal cord T2 lesions, as well as the number of brain T2 lesions, were significantly higher in patients who converted to SPMS, compared with those who did not.
The presence of oligoclonal bands in the cerebrospinal fluid, the liquid that surrounds the brain and spinal cord, also was significantly more frequent among converters. Oligoclonal bands are bands of proteins called immunoglobulins that indicate CNS inflammation.
When analyzing potential predictors of SPMS progression, the researchers found that brain and spinal cord T2 lesions, as well as oligoclonal bands, were significantly associated with an early SPMS conversion.
However, after adjusting for confounding factors, such as age, sex, and treatment initiation with CIS, spinal cord lesions were the only independent predictor of SPMS conversion; patients exhibiting such lesions at CIS diagnosis were more than two-times more likely to progress to SPMS than those without them.
The findings highlight cervical spinal cord T2 lesions at CIS diagnosis “as a strong predictor of SPMS,” and “should encourage us to study how spinal cord lesions can trigger neurodegeneration process in progressive MS,” Lacruz-Ballester said.
Currently, spinal cord lesions are believed to induce either atrophy, or shrinkage, of the corticospinal tract or a chronic inflammatory mechanism, Lacruz-Ballester noted. The corticospinal tract is a collection of nerve cell fibers that carry movement-related information from the brain to the spinal cord.
These results also “favor the use of high efficacious therapies from disease onset to prevent future disability,” the researchers wrote.


Leave a comment
Fill in the required fields to post. Your email address will not be published.