Atara Biotherapeutics Study Links Epstein-Barr Virus Infection with MS
Written by |
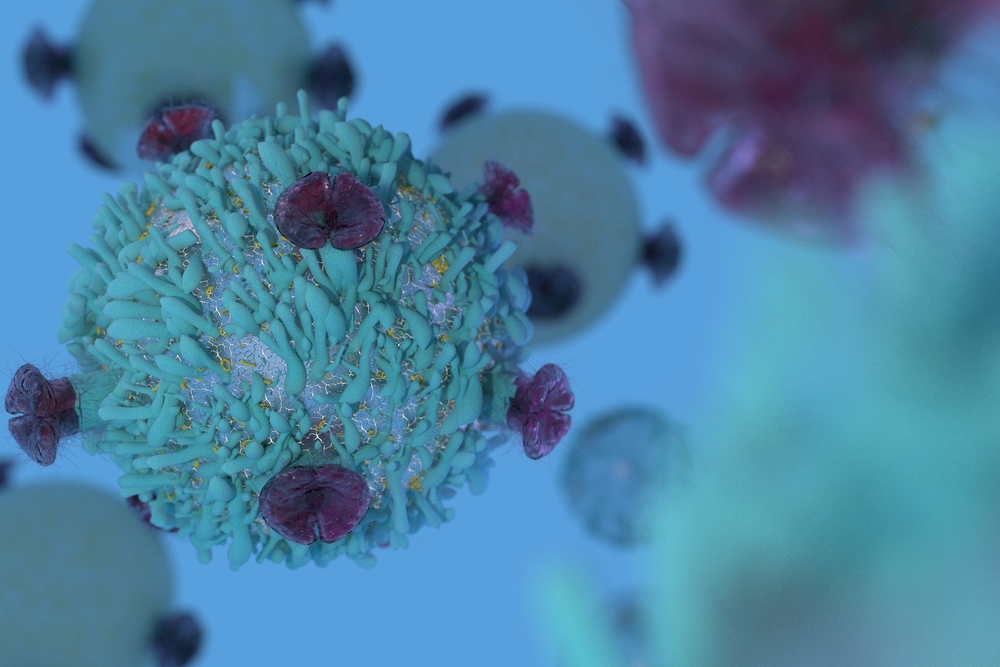
Analysis of post-mortem brain samples from multiple sclerosis (MS) patients and healthy individuals (without neurologic disease) showed that while signs of Epstein-Barr virus (EBV) infection are present in both groups of brains, EBV-positive immune cells were more prevalent and densely populated in the MS brain.
The study reporting those findings, “Molecular signature of Epstein-Barr virus infection in MS brain lesions,” was published in the journal Neurology: Neuroimmunology & Neuroinflammation, the official journal of the American Academy of Neurology.
EBV infection is estimated to affect about 95% of adults worldwide, and previous studies have suggested a potential causal link between EBV infection and the risk for MS. These studies reported that MS patients had higher levels of antibodies against EBV than non-MS individuals, but follow-up studies have failed to find the same results.
Now, researchers analyzed autopsied brain samples from a MS brain tissue bank and from healthy, non-MS samples (controls).
They detected signs for the presence of EBV in 93% of MS brain samples, but also in the controls, although to a less extent (78%).
Share your thoughts on the link between Epstein-Barr virus and MS!
EBV infects immune B-cells, and the results showed that 85% of MS brain samples contained a higher percentage of B-cells positive for EBV-encoded RNA. In contrast, almost none of these cells were found in brain samples from controls.
“The Neurology publication extends the growing body of evidence linking EBV infection and MS using a well-characterized MS brain tissue bank,” Chris Haqq, MD, PhD, said in a press release. Haqq is executive vice president of research and development and chief scientific officer of Atara Biotherapeutics.
“We observed that EBV is present in both MS and control brains, with EBV-infected B-cells and plasma cells more prevalent and localized to MS brain lesions,” Haqq said.
Within immune B-cells, EBV switches between latent and lytic forms. The latent form is a way for the virus to evade the host’s immune system, whereas the lytic form corresponds to a state in which the virus replicates more actively. EBV infection was detectable in both MS and non-MS brains. although latent virus was more prevalent in MS brains, and lytic virus was restricted to chronic MS lesions.
“Taken together, our results that are derived from a well-characterized MS brain tissue bank support previous studies demonstrating the presence of EBV in the MS brain,” the team concluded.
“These findings advance the understanding of EBV’s potential role in MS pathogenesis and provide support for targeting EBV-infected immune cells associated with chronic MS lesions as a potential treatment for this severe autoimmune disorder,” Haqq said.
Atara is developing two therapies, ATA188 and ATA190, to eliminate EBV-infected B-cells in the central nervous system that can induce autoimmune responses and potentially contribute to MS development. Early results suggest these therapies can induce clinical improvements in MS symptoms.


Brenda
No ms doctor is doing this therapy. Why do you think that is. Is it very expensive or are the side effects bad? Non of my friends are getting this treatment.
Burton
If you access the link for ATA188, the article states that it shows promise in Phase 1 clinical trials, which was conducted with a small group of subjects. It still has to go through both Phase 2 and 3 studies, then an NDA (New Drug Application) must be filed. The FDA has to approve it after review. It is not so simple to state that an MS doctor, or any doctor should use it, and you should read the information from the link to learn more about what steps are necessary before a therapy can be approved.
Katherine
I have PPMS and am doing Ocrevus infusions as it was recently FDA approved for PPMS(first med!!!) as well as RRMS I just finished my 2nd dosing and will have my next one in 6 months - I am very excited by this med - almost no reactions and I had a ton of reactions and new lesions when on Copaxone 40mg injections.. my insurance covers the med and Ocrevus manufacturer will cover anything that isn't ... I think comparing is a slippery slope as we are all snowflakes after all; we have MS but each case is unique even if similiar .. I work full time - watch what I eat/healthy -take vitamins - keep stress to a minimum -try to get plenty of rest and while I use a cane I am walking ... PML has not been linked to this med which is huge !! As I said I am very excited to have this treatment.
Joerg Richter
Of course PML is linked to OCREVUS as well and herpes virus infection and cancer on top. I am scared of this infusion cause I will have it soon. I suffer under herpes when my immune system is down.
Maria
Dear Katherine, thank you for your comment. I have had Ppms for 6 years and I have never taken any meds because as you know the first approved drug is Ocrevus. Like you I have problems with walking - but I still walk some hundred meters without help. Does Ocrevus help you with your walking difficulties?? Does it improve any symptoms?
I know all of us are different or unique as you say - but I am so much interested in your experience. Thank you so much.
Joni Mercado
Many very expensive MS drugs claim to reduce the amount of relapses in MS by ~30%. What about the other 70%, and how do we know whether it isn’t MS going into remission on its own?! My doctors have no answer to that. If a cure for MS was ever recognized and made public, pharmaceutical companies would stand to lose billions of dollars for themselves and their investors! The same would hold true for other diseases. Have you heard of a cure for any diseases lately? Makes you wonder!
I was diagnosed with MS in 1991 (could have had it way before, though). I started injecting these toxic drugs into my system which left me feeling flu-like symptoms and produced injection-marks on my legs. I felt no improvement after a couple of years so I stopped taking them. After 27 years, I feel very little difference. My only problem is a bit of difficulty with balance and walking which has resulted in lower back pain from this. I use only a walker. I have more plaque now but my Ms is still stable!
My theory is that if you were ever bitten by a Lyme-disease-carrying tick which is the size of a poppy seed and didn’t know it, the Lyme disease could remain dormant in your system and, over time, could alter the immune system and become MS (i.e. Lyme could be a precursor to MS!) liken to Chicken Pox becoming Shingles decades later!
In 1991, I was tested and diagnosed by two separate doctors. Results from each indicated I had borderline Lyme & borderline MS. I had only one plaque on my brainstem then which almost went unnoticed on my MRI!
The ELISE test, done in a Petri dish (results take about a week or two), showed I had a slight indication of Lyme Disease.
If a map exists indicating the prevalence of both those with Lyme Disease and MS in certain areas (mostly rural, I would think), that would be interesting to take note of.
Any comments?
Kate H
If you have Lyme disease then one needs to take a whole bunch of antibiotics, but there is also CBD which has been proven to kill lyme bugs. Please see Dr.Murakami's website at lymechat.freehostia.com
Do the questionnaire on there and submit it and then he will call you and discuss your situation and advise you further. He is a passionate caring but retired Doctor that has studied lyme for most of his career. Please see if he can help you!
Joni Mercado
In reference to my comment above, I forgot to mention that in 1982, I had optic neuritis in one eye. It was treated with oral prednisone to make it go away. However, because I wasn’t treated with both oral prednisone along with intravenous prednisilone, it came back two years later in the other eye. According to MedLine, both used together would have returned. When my husband told the doctor about that, he said we’re too busy to read about everything! What did they know then.
Anyway, 9 years later, I was coming home from work during rush hour when double vision kicked in. That was from the one dot of plaque found on my brainstem in my MRI. I was treated by the Lyme specialist with 6 months of an intravenous antibiotic called Rocefin. My double vision went away. I felt great and stronger. I had Rocefin treatment again twice several years later and, again felt stronger. Because Rocefin use was not accepted as treatment for MS, my insurance company denied any further or continuous treatment.
Stress could make MS surface. My car was hit at a highway exit in 1996, went into a tailspin, hitting a sign. I was shaken but unhurt. However, a year later, I started having trouble walking. When I previously had double vision, this occurred about a year after the car my husband was driving on the way to the Post Office, with me in it, was hit by a woman’s out-of-control car on a wet, slippery road curving around a bend. None of us were badly hurt. Another stressful event.
How many of you got MS after a stressful event occurred?
Catherine Owings
Stress definitely caused mine to surface. My ex-husband and I were living with my grandmother with our one-year old when she threw him out. She told me that my baby and I could stay but he had to go. He was a pretty miserable person and we later divorced, but this certainly was a stressful situation. My younger sister has MS too, and she and her husband were going through some stressful times when hers surfaced. We have two other sisters with no problems. In regards to the epstein-barr virus, she and I had strep throat, mononucleosis, and constant upper respiratory infections throughout our childhood
while the other two didn't. I've always thought that the EBV was a suspect; I'm not surprised that they are finding more about it in relation to MS.
Jill
I believe I got it when my husband walked out after 5 years of marriage when I was 26 years old in 1996. I was completely traumatized. Five months later I was very sick with what I now believe was Epstein- Barr virus. I couldn't get out of bed for a week or more. Soon after, the migraines and the hiccups 5-6 times a day began. Fast forward to 2015 and my upper lip went numb. A Cat scan indicated a scar on my brain, and I had no insurance to get an MRI, (It took me 2 years to pay for that scan) meanwhile they began treating me for a stroke. We decided to wait 9 months for the Affordable Care Act to begin and get an MRI at that time. Two weeks after the insurance began, I ended up in the E.R. w/ extreme dizziness. Nine hours later I was diagnosed w/ advanced brain cancer, and multiple brain tumors. I began seeing an oncologist.
She thought I had about a year to live. I was 45. The radiation Oncologist wanted to start radiation on my brain, but needed the type of cancer to be identified. The lymph node they took out of my neck was negative. The Mammogram, PET scan, all tests were negative, so they decided to do a brain biopsy. The couldn't figure it out even w/ my brain tissue, so they sent the sample all over the country and finally, I got the news a month later. My oncologist called me at work...and tells me "you don't have cancer". The Mayo clinic in Rochester MN. got some of the sample, and the brilliant research Doctor there determined it was demylinating disease(MS).
Gia
Jill, wow, just wow. That's why I don't trust the ER for any diagnoses. That is horrible!