Metformin Works to Promote Remyelination in Ways Similar to Fasting, Study Says
Written by |

Metformin, a common diabetes treatment that works to mimic dietary fasting, was seen to promote remyelination in the stem cells of elderly rats, suggesting it may be useful in treating multiple sclerosis.
“Metformin Restores CNS Remyelination Capacity by Rejuvenating Aged Stem Cells” was published in the journal Cell Stem Cell.
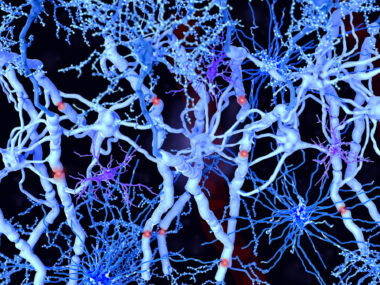
MS is characterized by the loss of myelin, the protective sheath around neurons (nerve cells) that helps them to communicate. As such, MS treatments that promote the replacement of lost myelin — a process called remyelination — are needed.
Myelin is made by cells called oligodendrocytes. These oligodendrocytes derive from specialized stem cells, which are called oligodendrocyte progenitor cells (OPCs).
Researchers in this study first showed that, as rats age, their OPCs lose the ability to readily mature into functional oligodendrocytes, a process common to aging. They found that, if given the proper stimuli, about 60% of OPCs from young rats grow into mature oligodendrocytes, while in aged rats less than 20% mature to oligodendrocyte cells.
The researchers then compared OPCs from old (20–24 months) and young animals (2–3 months), and found that aged OPCs exhibit certain cellular changes that are associated with cellular aging, particularly changes to their mitochondria (the cell’s powerhouses where energy is produced).
“As with most regenerative processes, the efficiency of remyelination declines progressively with aging to the extent that it becomes so slow that it eventually fails,” they wrote. “This has important implications for chronic demyelinating diseases such as multiple sclerosis (MS) that can extend over several decades. Delayed remyelination renders demyelinated axons susceptible to [the] irreversible degeneration” evident in later MS stages.
The team wondered if targeting these cellular changes could improve the ability of oligodendrocyte progenitor cells to turn into oligodendrocytes and, by extension, promote remyelination.
Researchers used two approaches with the animals. The first was a alternate day fasting, where rats only ate every other day, which is known to limit cellular aging; the second was giving them metformin, a “small-molecule fasting mimetic” used to lower blood-sugar levels in diabetics, which acts through a protein called AMPK. This protein plays an important role in helping mitochondria work to produce cellular energy as intended.
Results showed that both approaches could promote the formation of oligodendrocytes in elderly rats, leading to better myelin repair.
In rats with chemically induced lesions of myelin loss, both alternate day fasting and metformin also improved remyelination relative to rats given neither treatment approach.
“Overcoming the effects of aging on OPCs is important in generating a permissive environment for remyelination. Interventions such as dietary restriction or drugs that mimic its effects will likely alter the function of OPCs and other cell types that contribute to remyelination … and may thus have dual benefits for the treatment of chronic demyelinating neurodegenerative diseases,” the study concluded.
Robin Franklin, PhD, a professor at the University of Cambridge and study co-author, called the finding “one of the most significant advances in myelin repair therapies there has ever been,” he said in a U.K. MS Society news release.
“The findings shed light on why cells lose their ability to regenerate myelin, and how this process might be reversed. Although research so far has been done in rats, we hope to move it forward into humans soon,” Franklin added.

Esther S. Barth, D. O.
I worked at Bristol Myers to bring metmformin onto the market in the USA. Now as an a MS patent I would most interested in finding out how to become involved in finding out if it. Could help me. Please advise how I can find out how to proceed.
David Cortese
I too would like to participate in studies with humans. What do I do? I already take Metformin for type 2 diabetes.
Rosemary Conte
Why would anyone take a toxic drug like Metformin that mimics fasting every other day, when they could get the same result by --- FASTING EVERY OTHER DAY?
William Dods
I believe the answer to your question is that most people would rather not fast if they are offered a pill that might achieve the same result. Most people do not walk into the doctor's office and ask what lifestyle changes they can make, they go in and ask for a pill. And many doctors are quite willing to accommodate them.
Daisy
Why would anyone ask for an infusion able drug that memics chemo? We're all hoping and looking for help.
Puya
I have tried fasting. The issue for me is that I can't maintain my weight. It approaches a dangerously low level when I do. I know it is hard to believe for many people, but for me it is surprisingly hard to gain weight while eating healthy. Sure I can gain weight if I eat tons of processed foods and sugars but I have so far failed to do so on a healthy diet.
That is one reason why I would welcome such a drug. I'm sure others may have other reasons.
Angela
Or a ketogenic diet with intermittent fasting 16hrs overnight fast, and then keto or very low carb clean foods. That is what I do, and how I reversed 99% of my MS symptoms. I was given metformin once, just because I wanted to see if it would help me lose a few pounds and I felt sick. After three days, I stopped it. Keto and fasting 16:8 works well.
Shane
Using Keto I have have eliminated so many of my medications for so many of ailments! A life change for me! MS is my last one & I still have Metformin on my daily regimen along with my multivitamins ?
Ray Ibarra
Is metformin available for ms treatment??
Concerned Caregiver
Interesting. Seems like other medications often produce better results than ms medications. There have also been positive studies showing Viagra can help ms patients! Also, placebos seem to be helpful in some cases as well, definitely safer! Like a previous reply states: why not just fast every other day? Sounds easy enough, but my wife loves to eat, so I don't think the fasting would work. Why does this help? Does it reduce toxic (pesticide) build up in fatty tissue? Is this also why low fat diets like the Swank diet have shown benefits? Didn't Neurology Today magazine draw a comparison between pesticides and Parkinson's disease? Seems like the focus should be to lighten one's toxic load, not add to it. Am I wrong or am I right?
Lisa
I’m living with MS And found the most natural way a nutritional eating plan and learn how to treat parasites. Lots of people have lots of improvement. It just takes a will power.
Irini
One of the reasons that fasting helps re-myelination I guess is because induces the production of human growth hormone, which somehow triggers cell growth, rejuvenation, and stem cells production. Don't you agree?
Ebrahim Soleimannejadian
my daughter, 46, suffers from ms and neuralogia. The pain is so bad that she satisfies ms, however she is with whelchair. She injects Ritoximab (1g) every 6 months and Dolphyra two pills/day. It is getting worse. Can she try Metformin?
Zarita
Rituximab seems to have some side effects in many patients. consult with her doctor for a shift to DMTs like dimethyl fuamarate. it is not wise to use metformin in MS patients while the results are just come out of the lab and the medicine may cause blood sugar decreases to the level not safe for everybody. fasting may also be a good option due to its many benefits for healthy people. But for patients all aspects of their health status should be considered.the patients should see if they really could tolerate not to eat for a couple of hours every other day. and consult their doctor too.
Hope-Emily Wilkins
Until I read this I hadn't thought about my Diabetes and my MS together. However I have noticed worse flair ups since I changed from Metformin to Insulin. I never thought the tablet may be helping my MS.
jagdish kheterpal
It is a great news that Metformin is useful in other body problems besides treating diabetes 2.
I just want to know what is the maximum dose can be taken in this case
Donna
Would like to know doseage to treat ms side effects also
Hannah
I have a demyelinated spinal cord from pesticide exposure, could this help me? I also have diabetes.
Jo
The side effects of Metformin makes it impossible for me to take. It lessens the quality of life for me. I was shocked that one of the worse side effects (For me) was to have a bowel movement without warning.
My sister takes the highest dose and she has diarrhea. I was on the lowest dose.
I told my doctor this med was unacceptable. Anyone else have ideas of a replacement drug for early stages of diabetes 2? So happy to hear promising news for MS.
Angela
Low carb or keto diet... best way to reverse diabetes’
Zarita
please try a 3 hours daily working hard on a garden not actually as a replacement but add it as an option to your life style and your blood sugar will decrease to better levels as i saw this in other diabetes 2 patient.
Ana
That’s a doctors neurologists question there are so many false articles being posted
R Miller
I have been taking metformin for my diabetes for years and I don't see any positive response involving my MS. I would think there are a lot of MS patients like me that are taking metformin for diabetes that could already contribute to a study.
Linda Lear MD
This is in animal models only at this point. There have been no studies on doses and response in humans. I'm a ms patient also.
Dianne Welgan
Linda Do you think there will ever be human trials?
chris
Does the metformin cross the blood brain barrier without being injected?
jagdish kheterpal
Regarding metformin, here are certain questions for clarification and knowledge:
1: how much time it takes to act to start reducing blood sugar after food if it is taken half hour before it.
2. Is there any chart which
decides quantity of metformin dose and the blood glucose number testing with blood with pricking....
3. Can metformin check the dawn phenomenon in Diebetese 2.
What is the suitable maximum dose which is not harmful when Blood sugar is more than 250
Cindy
I’m a diabetic and was given this drug by a nurse practitioner and it was one of the most frightening things I’ve experienced. I literally took the prescribed amount two times and was shaking and could not think or speak normally. I was lucky enough I had a pharmacist that called knowing my living situation who call during the worst of it and he took action immediately. To this day I’m scared to take anything for diabetes. Do your homework!
Connie Cannon
I am on metformin and feel great! I have type two diabetes. When I was younger I fasted a lot and had a very good weight but menopause has done something to me and I wasn’t able to lose weight .