Need to Know: How a Spinal Tap Can Help to Diagnose MS
Written by |

Editor’s note: “Need to Know” is a series inspired by common forum questions and comments from readers. Have a comment or question about MS? Visit our forum. This week’s question is inspired by the forum topic “Have you had a lumbar puncture to help diagnose your MS?” from Jan. 29.
I got a spinal tap to help confirm my MS diagnosis.
Two amazing nurses kept my attention somewhat diverted while the physician performed the procedure using the aid of a fluoroscope. I say “somewhat” because the science nerd in me was fascinated with the view on the fluoroscope monitor, which resembled a livestreamed version of the spinal tap.
No, it didn’t hurt.
A few weeks later, I met with my MS neurologist. Based on all the data collected from my tests — MRIs, blood tests, and evoked potential tests, among others — I was diagnosed with relapsing-remitting MS.
Did I need the spinal tap? Maybe. Maybe not. Did it help confirm my MS diagnosis? Yes.
What is the diagnostic necessity of a spinal tap?
There’s some uncertainty among patients over the necessity of a spinal tap procedure to help diagnose MS.
On the one hand, the procedure provides good data on the presence of MS and can expedite a diagnosis. However, this test is expensive and may be subject to insurance qualifiers. It might be sought only when other diagnostic data are less conclusive. Some doctors may even forgo a spinal tap entirely if they have enough information from other tests to meet the McDonald diagnostic criteria.
A spinal tap is one of many diagnostic tools for confirming the presence of demyelinating disease. It might uncover evidence that other tests did not.
However, many other tests for diagnosing MS can also be inconclusive — even an MRI might not be conclusive enough to support an MS diagnosis on its own. It’s only after several tests are performed and the results compiled that a clearer picture of this hard-to-identify condition can be assembled.
A diagnosis of MS is considered a “diagnosis of elimination.” Many of the tests used to diagnose MS are performed to rule out other conditions, such as Lyme disease or lupus, two common MS “mimics.”
According to the National Multiple Sclerosis Society (NMSS) website, “It is important to know that an abnormal immune response in the [cerebral spinal fluid] is found in a number of other diseases, so the [spinal tap] test is not specific for MS. … The results are used in combination with the history, neurological examination, MRI and other tests to help make an accurate diagnosis.”
What is a spinal tap, anyway?
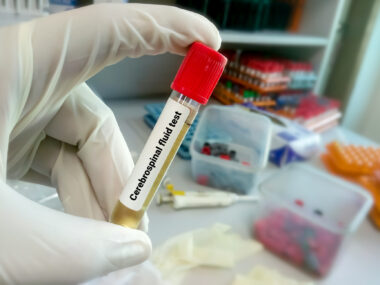
Also known as a lumbar puncture, the spinal tap is a procedure in which a trained specialist inserts a hollow syringe between two vertebrae in the lumbar (lower) region of the spine to remove a tiny amount of cerebral spinal fluid (CSF) from the spinal column. This fluid is sent to a lab for testing.
Sometimes the specialist will use a device known as a fluoroscope — a tool that incorporates camera technology in order to give the specialist visual guidance during the procedure.
The patient undergoing the procedure is asked to lie on their side or bend forward in a seated position. An area on the lower back is cleaned, then treated with a numbing agent before the puncture takes place.
How does a spinal tap identify MS?
According to the NMSS: “The CSF of people with MS usually contains: a specific group of proteins called oligoclonal bands; elevation of the level of protein. These findings indicate an abnormal immune response within the central nervous system, and may be suggestive of MS.”
However, up to 10 percent of all patients undergoing a spinal tap do not show these abnormal findings in their CSF. This demonstrates that the spinal tap, while a useful tool for identifying MS, may not always lead to conclusive findings in people with MS and cannot be relied upon as a stand-alone diagnostic measure.
Spinal tap risks
The most common concern about receiving a spinal tap is a post-lumbar puncture headache, which can occur within a few hours, or up to two days, following the procedure. It is caused by the leak of CSF into nearby tissues. It can be mild to severe and involve nausea, vomiting, and dizziness.
As many as 1 in 4 patients will experience these, so it’s typical for your specialist to discuss protocols for treating these headaches prior to a spinal tap procedure.
Are you facing a decision about whether to undergo a spinal tap to diagnose MS? Have you had the procedure, and if so, what was your experience like? Post your replies in the comments below or at the original topic “Have you had a lumbar puncture to help diagnose your MS?” forum entry.
***
Note: Multiple Sclerosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Multiple Sclerosis News Today or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to multiple sclerosis.

Kathryn
I had a spinal tap done to help with my diagnosis, which was CIS at the time. I was told about the migraine like headache that was possible with a 10-15% chance of this reaction. Accordingly I had the procedure done on a Friday and a friend friend stayed with me over the weekend. No reaction until I was on the interstate in the fast lane going to work on Monday. Terrifying but I make it to work. I needed what was called a blood patch to get rid of the headache and it cost $1000 in 2006. They take blood from your wrist and inject it into the spinal fluid to fill any bubble left from the spinal tap. It gets rid of the headache almost instantly but I was home bound until the next day. In summary it showed I had oligoclonul 7 bands suggesting MS and luckily I had great insurance and friends to get me through it.
Tamara Sellman
That's a familiar story (I, too, had the headache while driving to work, and missed a shift; however, I did not get a blood patch as the only place to do this is a ferry ride and commute into the city... I just powered through it for a day). It was worth it to get confirming information, indeed. Thanks for sharing your story, Kathryn!
Tamara
P sheppard
I had a lumbar puncture in the process of diagnosing my MS. The Dr. who did the lumbar puncture was fabulous...I felt no pain and had no headache at all. While I had heard several very negative stories of lumbar puncture outcomes, this was the last test to be done to offer a confirmation of my MRI diagnosis. I am grateful for all Dr's and nurses involved in the entire process, they all were superb.
Tamara Sellman
Thanks for sharing your experience, P sheppard. My own procedure (aside from the headache, which was manageable, if painful) was also done well and I felt like I had the best care. I like to hear that people have positive experiences when it comes to LP as so many negative "horror" stories exist out there. Not that bad things don't/can't happen, but people facing the possibility of this procedure need to know it's not necessarily going to be a terrible experience and that, in fact, it can be a very positive one. Everyone is different.
Tamara
Jan Beko-Nathan
I had a spinal tap as well in May 2017 as the MRI showed MS but not which type... the spinal tap was conclusive in diagnosing my Primary Progressive MS... I had wonderful doctor and nurse as well who gave me the choice of being kept in the loop of what was happening or idle chit chat... I opted for idle chit chat and we even discussed the iodine solution for cleansing the area being close to the cheap stuff we used to lay out in the sun as kids... when they confirmed the doctor wanted 20cc of fluid but they were going to take 5cc extra to make sure, I piped up that they should take 10cc extra cuz this was a one and done thing... they giggled like school kids, it was so refreshing! they would ask me how I was doing and I would reply it wasn't like eating cheesecake... the right staff sure make a world of difference for any procedure that one is not looking forward to! No pain, no headache, drank plenty of water the first day and stayed laying down... Positive thoughts work!!
Tamara Sellman
Jan, sounds like you had a wonderful medical team on board! You're absolutely right... positive thinking has many benefits!
Tamara
Lou Fashioni
Slightly misleading. Lumbar punctures do hurt. There is a risk of damage to the spinal cord (sometimes to the detriment of future mobility). There are plenty of other methods of MS diagnosis. This, in 2019 is a medieval practice best left in the past,
Catherine Schwaegler
I totally agree! I had my lumbar puncture in 2001 and it really, really hurt. Not only that, but the radiologist doing the test was very patient even though it took him two hours to obtain enough spinal fluid to run tests. Mine was not a walk in the park, for sure! However, the lumbar puncture was the last piece of the puzzle and I was diagnosed with M.S. The lumbar puncture showed cloudy, olygodendrite (sp)? filled fluid. Needless to say, I was very grateful to receive the diagnosis of Multiple Sclerosis. At least I could be put on a medication that has slowed the progress of this disease.
Tamara Sellman
Sorry you had a bad experience, Catherine. I am willing to bet that the tools and techniques for drawing CSF these days are far superior and more comfortable than they were in 2001. I agree that the confirming of MS from an LP is worth the discomfort, it helped me move forward, as well.
Tamara
Tamara Sellman
I'm not sure what you mean by misleading. The procedure is done using anesthesia, so if you're feeling it at all, then that is a shortcoming of the practitioner. You shouldn't feel anything. As with any medical procedure, there is always a risk for complications, but the risk is extremely small and, from a risk-benefit analysis, worth taking for the information the test can provide. Of course there are plenty of methods for diagnosing MS but for some complex cases, more information is going to make a big difference.
Tamara
oSandi
In 1990 I had a spinal tap done prior to receiving five days of (solu medrol?) intravenously as an outpatient. I don't remember if the headache/dizziness/nauseousness came on immediately but each morning my husband drove me to the hospital for treatment with my 22-month old in tow and then returned 2 hours later to pick me up again. The pain was immediate when I sat up - like being hit in the forehead with a sledge hammer - so I had to lie down across the backseat and fight nausea to and from the hospital on each of the 5 days before being put on oral steroids to begin weaning down. The situation was dire to begin with because I had lost the sight in my right eye over a 2-day period.
Tamara Sellman
I've heard similar stories from people using LP back in the early days of MS diagnosis. I think it's safe to say that today's LP is not going to be as uncomfortable as it was in 1990. Thank goodness!
Tamara
DS
How do I determine whether it’s MS or not? Since 1 & 1/2 year I am feeling numbness in my right thigh intermittently that last for 10-15 seconds. Suspected MS and did contrast brain and spine MRI scan 6 months back, no lesion shown up in result. Should I go for Spinal Tap now?